-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

April 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30
Uncategorized
How to Treat GTPS With Acupuncture and TCM
By Qineng Tan, L.Ac. Ph.d. and Xiaomei Cai, L.Ac., Ph.D.

Chronic pain in your outer hip? Hip pain when lying on your side? This can be a sign of Greater Trochanteric Pain Syndrome (GTPS), or gluteal tendinopathy. Acupuncture treatment can help relieve lateral hip pain due to GTPS, hip bursitis, and gluteal tendinopathy.
Lateral hip pain is a common problem, particularly for women over 40. In some cases, hip pain can be related to perimenopause and menopause, as changes in estrogen levels trigger inflammation in the tendons, causing tendinitis (inflammation or irritation of a tendon) or tendinopathy (general degeneration of a tendon that causes pain and swelling).
Bursitis can also be a common cause of hip pain. Bursa are small sacs of fluid that provide cushioning in the joints. When bursae (plural) become inflamed and stiff, it causes pain and swelling in the area.
What is GTPS?
The term “greater trochanteric pain syndrome” is a general way to refer to any discomfort or pain in the outer hip and thigh area that is caused by tendinitis, gluteal tendinopathy, bursitis, IT band problems, or trauma/injury to this area. Other types of hip pain can include: sciatica.
The greater trochanter is the rounded, bulbous part of the hip bone that juts out to the side; when you lie on your side, your weight is partially balanced on that bone.
The gluteal muscles (gluteus maximus and gluteus medius) are attached to this bone by tendons; these muscles and tendons are largely responsible for the movement and stabilization of the hip joint.
The loss of estrogen during perimenopause and menopause can weaken tendons, which have estrogen receptors. The hips abductor muscles can also become weaker, which puts extra stress on the tendons to keep the hip joint stable. When the chronic pain and tenderness leads to women reducing their physical activity, the whole problem can become worse.
Strengthening the muscles and tendons with the right exercise is crucial for keeping the hip joint stable and pain-free. Reducing hip pain and inflammation with acupuncture and TCM can help you feel better and return to your strength training and walking routines.
GTPS Symptoms
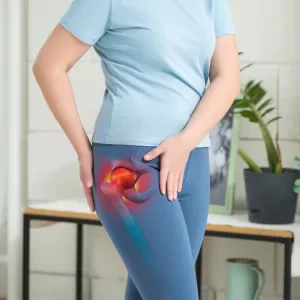
Greater trochanteric pain syndrome is chronic and can change over time. The pain might be sharp and come on suddenly, or build up slowly over time.
Symptoms of GTPS include:
- Chronic hip pain or soreness of the outer hip area
- Pain that radiates from the hip to the buttocks, low back pain, or thigh
- Pain that is pronounced when you lie on your side, or sleep disrupted by hip pain
- Numbness in the hip and thigh area
- Swelling in the hip and thigh area
What does GTPS pain feel like? This type of persistent hip pain can feel like a deep ache in the hip joint, a general tenderness just under the skin, or a sharp pain when you put weight on the affected leg.
The pain may be particularly triggered when you stand for long periods of time, sit with your legs crossed, or climb stairs.
Treatment for GTPS
Generally, GTPS, hip bursitis, and gluteal tendinopathy are considered to be problems with the soft tissues (muscles, tendons, and bursae) in and around the hip joint that will eventually improve on their own.
The goal of most treatments is to reduce pain symptoms, while making conservative modifications (like changing the way you stand or your sleep position) and engaging in gentle exercise. Recovery from this type of hip pain may take months.
Pain remedies such as icing, heat, massage, over the counter pain medications and anti-inflammatories may be recommended, as well as corticosteroid injections.
Acupuncture and TCM offer a way to help reduce pain and inflammation without side effects.
Can Acupuncture Help GTPS?
Acupuncture has been shown to be an effective treatment for pain of all kinds, due to its effect on the secretion of natural peptides in the body that reduce pain.
A review of studies concluded the acupuncture treatment for hip pain produced significant benefits compared to conventional treatment alone and combined treatments.
According to TCM theory, problems with painful, stiff tendons are considered a type of Bi Syndrome. Bi Syndromes are obstructions of Qi in the body that are caused by invasion of wind, cold and dampness. This type of invasion can happen due to external factors like weather, habits that expose you to cold and dampness, overuse or repetitive motions of the joints the weaken the tissues, underlying deficiencies in nutrition or specific organ systems, or even emotional issues that can block or deplete your energy.
Acupuncture treatment helps by improving blood flow to the area to nourish soft tissues and help relieve stiffness and improve flexibility. Based on the overall type of Bi Syndrome that is observed in a person’s symptoms, the acupuncture practitioner will choose acupoints along the affected meridians to help bring Qi and blood to the painful area, and the organ systems that are underlying causes of the blockage.
Herbs that strengthen and tonify the organs and tissues will also be prescribed.
Cupping is another TCM healing modality that can reduce muscle tension and improve the body’s natural ability to heal the tissues. Moxibusion can bring warmth, reducing pathogenic cold and dampness.
TCM and acupuncture also work on a hormonal level to help relieve tendinopathy pain. Balancing estrogen levels can help to keep the soft tissues supple and relieve muscle tension and pain in the tendons. Many women going through perimenopause and menopause can find relief from their symptoms, not only of joint pain, but sleep problems, vasomotor symptoms, itchiness, and more, through acupuncture treatment and herbs.
Acupuncture Near Me for GTPS in Santa Monica, West Los Angeles
Dr. Tan and Dr. Cai at Art of Wellness Acupuncture and TCM in Brentwood have over 35 years of experience in both TCM and Western medicine, helping people find relief from pain. While both doctors treat all types of conditions, Dr. Tan specializes in pain management and orthopedic issues, while Dr. Cai specializes in women’s health and hormones. If you or someone you love has been suffering with hip pain, do not hesitate to reach out to us to schedule a consultation. Relief from hip soreness is possible through a series of acupuncture treatments.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
Acupuncture for Sciatica Pain
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac.
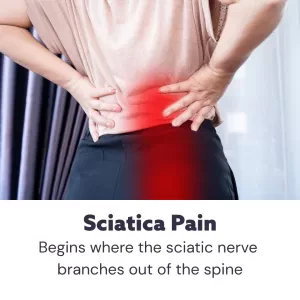
Sharp, burning pain in the buttocks that radiates down the leg? Low back pain and hip pain? These can be signs of sciatica, or nerve pain due to irritation or compression of the sciatic nerve. Acupuncture treatment can help relieve sciatic pain and promote nerve healing.
What is “sciatica?” Sciatica refers to the variety of symptoms that can arise when the sciatic nerve is irritated, due to injury, inflammation, or pinching of the nerve. These symptoms can include:
- Low back pain
- Sharp, shooting, or burning pain in the buttocks
- Nerve pain radiating down the leg
- Pain occurs with bending over or lifting legs
- Tingling or numbness, “pins and needles” sensation in the back, buttocks, leg or foot
- Muscle weakness in the leg
- “Foot drop” or dragging of foot when you walk
- In severe cases, urinary incontinence
When we say “sciatic nerve,” we are actually referring to two thick bundles of nerves that branch out of the base of the spinal cord and then run through the buttocks and down the legs. These nerves carry signals from the brain to the extremities, allowing you to make voluntary movements and communicating when there is pain or dysfunction.
Nerve pain or tingling sensations can occur at any point along the sciatic nerve bundle and tend to come and go, depending on your activity. The symptoms usually only show up on one side of the body.
Most people who experience symptoms of sciatica will find that they go away in a matter of weeks or months. In the meantime, though, sciatica pain can have a seriously negative impact on your daily life. Sciatica pain can be severe at times, affecting your motivation and ability to partake in your usual physical activities and even impacting your mental health.
Unfortunately, some people will develop chronic sciatica that can persist for months or even years. That is why it is best to address sciatic pain and not ignore it. If there are deeper problems contributing to inflammation or causing nerve damage, they need to be found and addressed.
Acupuncture treatment can help relieve sciatica pain and sensations of numbness and facilitate recovery.
What Causes Sciatica?
Sciatic nerve pain can be caused by a variety of factors or health conditions. In some cases “true sciatica” is caused by damage to or compression of the sciatic nerve. In other cases, the pain might be stemming from something else, such as piriformis syndrome, spinal disk problems, or stenosis, causing inflammation around the nerve bundle that causes pinching or compression.
Often sciatic pain develops due to improper form when lifting weight, repetitive stress from performing a task that requires bending or awkward positioning of the body, or a lack of core strength that puts too much stress on your low back when you lift something.
Some causes of sciatica include:
- Pregnancy can cause pressure on the sciatic nerve
- Osteoarthritis can damage the discs and/or cartilage in the spine
- Peripheral neuropathy related to diabetes
- Herniated disc
- Degenerative disc disease
- Spinal stenosis, or lumbar stenosis
- Bone spurs on the spine
- In rare cases, a tumor in the spine
Conventional Treatment for Sciatica

Generally, when you see your medical doctor for help with sciatic pain, the initial exam and treatment protocols will be conservative. Because imaging (x-ray, ultrasound or MRI) is not particularly helpful for showing nerve damage or impingement, typically doctors will wait to do this until the condition has gone on for more than a few months, and will be looking for herniated disks or other spinal issues.
Typical recommendations for sciatica will involve taking NSAIDs (anti-inflammatory pain medications), and using basic home remedies like cold packs and heating pads. Massage therapy may be helpful, and you might be referred to a physical therapist, who can offer some gentle exercises and stretches that may help.
If these recommendations do not help, next steps for treatment of sciatica pain may involve steroid injections or nerve root blocks, other medications, such as muscle relaxers, certain antidepressants that are known to help with nerve pain, oral corticosteroids, or opioid pain medications.
In severe, chronic cases, where the pain is related to herniated disc, spinal stenosis, or bone spurs, surgery may be suggested.
Acupuncture treatment, when used as an alternative or adjunct therapy for sciatica, can help relieve pain symptoms.
Can Acupuncture Help Sciatica?

Modern science has now been able to prove what TCM practitioners and patients have known for many centuries; acupuncture has an analgesic effect. The insertion of thin needles at specific points along the meridians can help reduce painful sensations, reduce inflammation, and help relax muscle contractions.
In fact, acupuncture is not only highly effective for the treatment of many different types of pain; it is also safer than use of pain medications, as it has no unwanted side effects.
According to TCM theory, sciatica pain is usually considered to arise due to imbalances affecting either the gallbladder (Shaoyang) meridian or the bladder (Taiyang) meridian. The presentation of pain, tingling or heaviness on one side lets the acupuncture practitioner know which meridian and system to address.
One study looked at patients who had been experiencing sciatica leg pain for at least three months due to herniated disks, but had not had surgery and were not scheduled to have surgery. Some were given ten acupuncture treatment sessions over the course of four weeks, while others were given “sham” acupuncture. (This is the control system for many studies involving acupuncture treatment.)
After two weeks, the patients who were receiving acupuncture were already reporting a significant reduction in pain and disability. At four weeks, they reported even greater improvement. At followups after 26 weeks, and a full year, the patients who had received acupuncture treatment reported continued benefits.
A systematic review of 11 clinical trials studying acupuncture treatment for sciatica found that acupuncture and acupuncture with medication were both more effective for reducing severity of pain symptoms over medication alone, and that acupuncture treatment had fewer negative side effects than taking pain medication.
Tuina massage is another TCM therapy that can help relieve low back pain or leg pain. In some cases, your acupuncture practitioner may also provide this traditional healing massage. Topical Chinese herbal analgesics, such as liniment or herbal patches may also be recommended.
Acupuncture Near Me for Sciatica in West Los Angeles
Dr. Tan and Dr. Cai of Art of Wellness Acupuncture on the Westside of Los Angeles have been treating patients for pain conditions for over 35 years. They draw upon a wealth of knowledge and experience in both Traditional Chinese Medicine and Western Medicine and are able to create an individualized treatment protocol for each patient. If you or someone you know has been suffering with low back pain, leg pain, tingling and numbness due to a pinched nerve, repetitive stress, or some other cause, please do not hesitate to reach out to Art of Wellness to schedule a consultation. Relief for sciatica pain through acupuncture treatment can help get back to your normal life again.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
Can Acupuncture Help With Bladder Control?
By Xiaomei Cai, L.Ac., Ph.D. and Qineng Tan, L.Ac., Ph.D.

Are you struggling with urinary incontinence (UI), leaking urine, or wetting the bed at night? Acupuncture and TCM can help relieve urinary urgency and help with bladder control problems.
Bladder problems are common in people or all ages and genders, but urinary incontinence becomes more common as we get older.
Women, especially, may begin to notice changes in their urinary frequency and control as early as their 40s. Recent data suggests that 30-50% of women between the ages of 45-60 experience bladder control issues.
There are many issues that can impact bladder control:
- Nerve damage, or other nervous system-related issues
- Pregnancy trauma or trauma from pelvic surgery
- Weakness in pelvic floor muscles
- UTI – urinary tract infections
- Perimenopause and menopause changes in estrogen levels
- Enlarged prostate (BPH)
- Constipation can put pressure on the bladder
Functional Incontinence or Stress Incontinence?
Nerves are a critical part of bladder function; messages from the brain let the bladder sphincter know when it is a good time to release urine. Functional incontinence is a condition that occurs when central nervous system signals between the brain and the bladder are not linking up correctly.
“Stress incontinence” may sound like it has something to do with anxiety or emotional pressures, but in this case, the term “stress” refers to mechanical stress. When there is internal physical pressure on the bladder, from things like laughing, coughing, sneezing, or any exercise that uses the abdominal muscles, the bladder can suddenly leak.
Stress urinary incontinence is more common in women, because changes in hormones during pregnancy, childbirth, perimenopause and menopause can have a dramatic effect on the tone of the pelvic floor muscles and all of the connective tissues that keep the bladder, the urethra, and other pelvic organs in place.
Urinary Retention
While it is less common, urinary retention is also a bladder control problem. In this condition, the bladder is not completely emptying when you urinate.
Acute urinary retention occurs when there is a sudden inability to urinate, even though the bladder is clearly full. This can cause serious pain and should be addressed with a medical provider immediately.
Chronic urinary retention can begin to happen gradually over time. Signs of chronic urinary retention include:
- Having trouble when starting to urinate
- Feeling like you need to urinate again when you just went
- Feeling like you always need to urinate
- Getting up multiple times during the night to urinate
- Weak flow of urine when peeing
Urinary retention can also be caused by central nervous system issues, sagging pelvic tissues, physical obstructions like an enlarged prostate or stones in the urethra, or some medications, like muscle relaxers.
Acupuncture treatment can help with urinary incontinence and retention by working on multiple levels to positively impact the central nervous system and toning the pelvic muscles.
Typical Treatment for Bladder Control Problems

Unfortunately, many people do not seek professional help for overactive bladder symptoms or incontinence, perhaps because they feel embarrassed, they think that it’s “normal,” and/or because they aren’t aware of what types of treatment for bladder control problems are available.
Medical practitioners will often suggest lifestyle changes that may help control bladder symptoms, such as managing your intake of liquids, avoiding constipation, and losing weight.
Pelvic floor physical therapy, which seeks to strengthen the pelvic floor muscles, may also be recommended. Gentle exercises can help reduce pelvic pain and pressure, and may help reduce the sensations of urinary urgency.
For many people, these natural interventions are not enough to solve the problem. Bladder training (sometimes called “timed voiding”) by scheduling when you go to the bathroom, not drinking anything all evening, and doing Kegels at stop lights are difficult habits to maintain, especially if you’re not feeling any results.
Acupuncture treatment can help support these practices in meaningful ways, so that you will notice improvement.
In more severe cases, surgery (known as “sling surgery) may be suggested. This surgery typically involves the insertion of synthetic “mesh” to support the pelvic organs. While this helps in some cases, unfortunately, some people experience serious complications after this procedure.
Acupuncture and TCM offer an alternative treatment for urinary incontinence that can help naturally improve bladder control.
Can Acupuncture Help Incontinence?
According to TCM theory, urinary incontinence is generally considered to happen due to a weakness of the kidney Qi. Strengthening the Qi of the kidneys with acupuncture and herbs helps to improve the function of the bladder.

Urinary function depends on a complex working together of the various nervous systems within the body. The autonomic, somatic, and parasympathetic nerves are all involved in stimulating, controlling and relaxing the different muscles and sphincters that allow urine to be held and released appropriately.
While TCM views organ systems in a different way than conventional medicine does, acupuncture points have been used for centuries to influence the nervous system at the brain-body connection level, as well as to help with specific, localized muscle functioning.
Acupuncture treatment that targets specific acupoints can help reduce contraction of the bladder muscles, to prevent leaking of urine and sudden feelings of urgency.
Acupuncture also has an analgesic effect, which means it can reduce pain and related sensations. Thus, it can help relieve the physical feelings associated with urinary urgency and pelvic pressure.
This can help with the process of “bladder training,” as it may allow you to wait longer before going to the bathroom and have a clearer awareness of the bladder fully emptying when you do.
Electroacupuncture, in particular, has been shown to help reduce leakage and improve the functioning of the urethra and bladder, reducing the symptoms of stress incontinence.
Acupuncture Near Me for Bladder Control in Los Angeles
Drs. Tan and Cai at Art of Wellness Acupuncture in West Lost Angeles have over 35 years of experience helping patients with bladder issues, due to pregnancy, childbirth, perimenopause, enlarged prostate. This condition can be frustrating and embarrassing. The acupuncturists at Art of Wellness are caring and easy to talk to. They can help you feel comfortable and more confident in your daily life and sleeping through the night, without urinary problems like urgency and leaking.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.
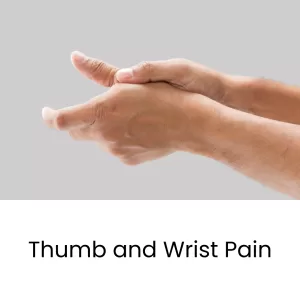
Sore thumb? Swelling around the thumb? Wrist pain on thumb side? These could all be symptoms of De Quervain’s Tenosynovitis, or inflammation in the thumb tendons. Acupuncture and TCM provide natural alternative De Quervain’s tenosynovitis treatment, to help relieve pain and improve mobility.
What Is Tenosynovitis?
Tendons are strong, flexible tissues that connect muscles to bones. Tendons are protected by sheaths, or synovial membranes. When the sheaths become inflamed, they can swell and become less able to stretch and move freely.
Wrist pain, hand pain, ankle pain, and foot pain can all be caused, in some situations, by tenosynovitis, because these are parts of the body where the tendons are long and do a lot of work. There are synovial sheaths protecting tendons all over your body, though, and anytime they become inflamed, this can be referred to as “tenosynovitis.”
What causes De Quervain’s tenosynovitis? The causes of tenosynovitis are not always apparent. Inflammation can occur due to overuse of the joints, or repetitive motion, or an injury or strain. Infections and other health problems that contribute to overall inflammation can also cause De Quervain’s disease to develop (such as rheumatoid arthritis or diabetes).
Tenosynovitis can also be related to hormonal fluctuations and imbalances, particularly in women. This condition is sometimes referred to as “mother’s wrist,” because it is more common in postpartum women, and also during the perimenopause transition.
De Quervain refers specifically to inflammation of the sheaths that protect the tendons of the thumb, and can lead to pain and swelling around the base of the thumb and the wrist.
Conventional Medical Treatment for De Quervain’s Tenosynovitis
In most cases, conventional treatment for De Quervain’s tenosynovitis focuses on reducing inflammation in the tendon sheath and preventing further irritation. Doctors typically begin with conservative approaches such as rest, activity modification, and immobilizing the thumb and wrist with a splint or brace. By limiting the motion of the inflamed tendons, the sheath has a chance to calm down and heal.
NSAIDs, such as ibuprofen or naproxen, may be recommended to help reduce swelling and ease pain. For more persistent symptoms, corticosteroid injections are often used to decrease inflammation quickly. In many cases, these injections can provide temporary relief, but symptoms sometimes return, especially if repetitive motions continue.
In severe or longstanding cases that do not respond to conservative care, surgery may be suggested. A De Quervain’s release procedure involves opening the tendon sheath to relieve pressure on the tendons and restore normal gliding. While generally effective, surgery carries risks such as scarring, nerve irritation, or reduced grip strength.
Although these treatments can provide relief, you might want to seek alternatives that address both the inflammation and the underlying imbalances contributing to chronic tendon irritation. Acupuncture and Traditional Chinese Medicine can help relieve the pain of De Quervain’s tenosynovitis, while also addressing the underlying causes of inflammation.
How Hormones Affect De Quervain’s Tenosynovitis

Interestingly, De Quervain’s is more common in women, especially during pregnancy, postpartum, and perimenopause. Hormonal fluctuations—particularly changes in estrogen levels—appear to influence tendon and connective tissue health. Studies have shown that estrogen receptor beta (ERβ) is expressed in tendon tissues, and changes in estrogen levels may alter tendon metabolism, collagen turnover, and inflammatory signaling. Lower estrogen levels, or rapid fluctuations such as those occurring postpartum or during perimenopause, may make tendons more susceptible to swelling and irritation.
This explains why many new mothers develop De Quervain’s (“mother’s wrist”). Repetitive lifting of a child, combined with hormonal changes, can create the environment for tendon sheath inflammation. Acupuncture and TCM can be especially helpful for these patients because treatment addresses both local inflammation and the systemic hormonal imbalances that contribute to tendon vulnerability.
Acupuncture and TCM Treatment for De Quervain’s
In Traditional Chinese Medicine, De Quervain’s tenosynovitis is often associated with Qi and Blood stagnation in the wrist and thumb. When the flow of Qi is blocked, whether from overuse, strain, repetitive movements, or an underlying deficiency, the tendons are not receiving adequate nourishment. This lack of nourishment leads to stiffness, swelling, and pain along the meridians.
The affected area overlaps primarily with the Lung meridian (which runs along the thumb) and the Large Intestine meridian (which crosses the wrist). If these channels become obstructed, pain and restricted motion occur.

In some patients, underlying Liver Blood deficiency or Kidney deficiency can weaken the tendons, making them more prone to inflammation. Others may present with Dampness or Heat accumulation, leading to swelling, burning pain, and difficulty gripping.
TCM treatment not only targets the painful wrist but also restores balance throughout the body, helping to prevent recurrence.
How Acupuncture Helps De Quervain’s Tenosynovitis
Acupuncture is widely used for hand and wrist pain, and research supports its effectiveness for tendon inflammation. Clinical studies have shown that acupuncture helps reduce pain, improve grip strength, and restore normal tendon movement by increasing microcirculation around the sheath, reducing local inflammation, and promoting healing of soft tissues.
One controlled study found that acupuncture significantly reduced wrist pain and improved functional mobility in patients with De Quervain’s, performing as well as or better than splinting alone.
Other research demonstrates that acupuncture modulates inflammatory pathways, including cytokines and neuropeptides involved in tendon irritation (as reviewed in the study from Frontiers in Pharmacology).
Electroacupuncture may be especially helpful for stubborn cases by stimulating deeper tissues. Patients often experience noticeable improvement in pain and mobility within a few sessions.
Moxibustion may be used to warm the channels and promote better circulation, especially for chronic cases with Cold-Damp stagnation. Cupping around the forearm and upper arm can help release tension in the muscles that control thumb movement. Tui Na massage techniques help reduce adhesions around the tendon sheath and improve range of motion.
These manual therapies complement acupuncture by addressing muscle imbalances and promoting the smooth movement of tendons along the radial side of the wrist.
Chinese herbal formulas may be prescribed to address inflammation and support tendon repair.
Topical herbal liniments or plasters can also be applied directly to the wrist to promote circulation and relieve pain.
Acupuncture treatment is highly individualized. Some patients require more focus on inflammation reduction, while others need systemic support for hormonal balance, postpartum recovery, or chronic overuse patterns. By addressing both tendon inflammation and whole-body imbalances, acupuncture offers a comprehensive approach that can improve healing and prevent future flare-ups.
Acupuncture for De Quervain’s Tenosynovitis Near Me in West Los Angeles
If thumb and wrist pain are limiting your daily activities, acupuncture and Traditional Chinese Medicine can offer natural, effective relief. Whether your symptoms began after repetitive work, new parenthood, or hormonal changes, TCM provides a personalized, holistic plan to reduce inflammation and restore comfortable movement.
Contact Art of Wellness, near Santa Monica, to schedule a consultation and let our highly experienced doctors of TCM help to heal wrist pain naturally.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
Chinese New Year 2026: Year of the Horse
by Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Strong, fiery energy is on the horizon, as the Horse Year gallops in this coming February 2026.
Chinese New Year begins on February 17, 2026, and we say goodbye to last year’s Wood Snake. The Year of the Fire Horse may bring a driving force and a sense of propulsion to your projects and dreams.
In Chinese astrology, the Horse symbolizes vitality, independence, and the pursuit of freedom. When combined with the Fire element, the Horse brings intense, passionate energy. The Fire Horse inspires bold action, confidence, and creativity, but also calls for balance and mindfulness to keep from burning out.
To find your sign in Chinese Astrology, check out our previous article about Chinese New Year and the Eastern Zodiac signs here.
Chinese Astrology and the Fire Horse
In the Chinese Zodiac, each year is associated with one of twelve animals and one of five elements (Wood, Fire, Earth, Metal, or Water). Together, they make a complete cycle every 60 years.
The Horse is naturally energetic and spirited, representing movement and strength. When paired with Fire, this energy becomes even more powerful, dynamic, and driven.
The last Year of the Fire Horse occurred in 1966, which we may remember as a year of intensity and transformation.
The Fire Horse year can bring great potential for breakthroughs and creative expansion, but it may also stir restlessness and impatience. This is a time to move forward with confidence, but also with clarity and care.
The energy of this year is fast-moving and transformative. It’s a powerful time to launch new projects, travel, or make big life changes. However, the Horse can sometimes gallop too fast, so it’s important to stay grounded and avoid overexertion or impulsive decisions. Taking time to rest and reconnect to your inner rhythm will help you make the most of this year.
Personality Traits of the Fire Horse

People born in the Year of the Horse — 1930, 1942, 1954, 1966, 1978, 1990, 2002, 2014, and 2026 — are known for their independence, enthusiasm, and drive. Horses are natural leaders who thrive on challenge and movement.
If this is you, then 2026 is your “ben ming nian.” When it is “your year,” you are beginning a new cycle. The ben ming nian is a time to plant seeds to come to fruition in future years. It can be an exciting time, but it is also necessary to protect yourself, as sometimes problems can crop up.
During a Fire Horse year, fiery traits are amplified. You may feel a renewed sense of purpose, courage, and inspiration.
Horses have strong life force energy and attract others with their warmth and vitality. They crave freedom and prefer to chart their own course. Horses are decisive, but may need to slow down and think before leaping. Fire Horse people are deeply emotional and can inspire others, but must manage stress and emotional intensity carefully.
Top 5 Health and Wellness Tips for Horse People
In Traditional Chinese Medicine, the Horse is connected with the Fire element and the Heart and Small Intestine meridians, which govern circulation, vitality, and emotional balance. The Fire Horse’s strong energy can sometimes lead to overwork, burnout, or stress-related health issues if not moderated.
To stay well during this fiery year, Horse-born individuals should focus on maintaining internal harmony and nurturing calm:
- Protect the Heart: Avoid excessive stress, caffeine, or late nights. Acupuncture can help regulate the Heart Qi and Shen (spirit), easing anxiety, palpitations, or restlessness.
- Support the Nervous System: Horses are sensitive to emotional ups and downs. Practices like Tai Chi, meditation, or Qi Gong can help smooth the flow of Qi and calm the mind.
- Watch Digestive Health: The Small Intestine meridian connects with gut function. Avoid overeating spicy or greasy foods and favor warm, nourishing meals.
- Stay Hydrated and Grounded: Balance Fire energy with cooling foods like cucumber, pears, watermelon, and green tea.
- Get Regular Rest: Sleep restores Yin energy and helps the body recover from the Horse’s natural drive and activity.
This is a wonderful year to renew your vitality and channel your passion — but remember that steady pacing will carry you farther than pure speed.
Lucky Colors and Symbols for Chinese New Year 2026
To harmonize with the Fire Horse’s energy, use colors and symbols that reflect vitality and success. Lucky colors include red, orange, and gold, representing Fire, joy, and prosperity. Add touches of green for balance and growth.
Displaying jade or citrine stones can attract abundance and protection. Plants like bamboo, citrus trees, and lucky palms bring refreshing Wood energy to balance Fire’s intensity.
For more general Feng Shui tips for the New Year, read our previous article here.
Chinese New Year Traditions for 2026

As always, preparation for the Lunar New Year is about clearing away the old and inviting in the new. In China, families will travel long distances to reunite and celebrate with loved ones.
Before the New Year, homes are cleaned from top to bottom to sweep out stagnant Qi and make space for prosperity. Decorations in red and gold fill homes and streets. Red envelopes filled with money are given to children as blessings for the year ahead.
Foods that symbolize wealth and longevity, like dumplings, spring rolls, long noodles, and tangerines, are enjoyed to usher in good fortune and abundance.
Feng Shui Tips for the Year of the Fire Horse
A few thoughtful touches around your home can help keep good energy moving smoothly.
- Activate Fire energy in the south area of your home with red candles, lamps, or artwork.
- Add Water elements (such as a small fountain or a bowl with floating flowers) to balance the intensity of Fire.
- Keep clutter minimal to allow Qi to move freely — especially near doors and pathways, symbolic of the Horse’s freedom of motion.
- Incorporate living plants with upright growth to attract prosperity and balance the dynamic Fire Horse energy.
Acupuncture and TCM for the Fire Horse Year
In Traditional Chinese Medicine, the Fire element governs both joy and agitation. When balanced, Fire brings warmth, passion, and enthusiasm for life. When excessive, it can manifest as insomnia, irritability, anxiety, or heart palpitations.
Acupuncture can help balance the Heart Fire, calm the spirit, and support overall energy flow. Herbal medicine may be prescribed to nourish Yin, clear Heat, or tonify Qi, depending on each person’s constitution. By maintaining equilibrium, we can enjoy the vitality of this year while keeping our health and emotions steady.
A New Year Message from Art of Wellness
As we gallop into the Year of the Fire Horse, may you find the courage to pursue your dreams and the wisdom to pause and breathe along the way.
From all of us at Art of Wellness Acupuncture, we wish you abundance, joy, and radiant health in the year ahead.
“马到成功!” May success come swiftly, like a galloping horse!
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.