-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

June 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30
Uncategorized
Acupuncture and TCM Treatment for Perimenopause Symptoms
By Xiaomei Cai, L.Ac., Ph.D. and Qineng Tan, L.Ac., Ph.D.

Changes in mood, sleep, energy levels, or menstrual cycle? Hot flashes, itchy skin, or joint pain? These can all be signs of perimenopause, the transitional period leading up to menopause. Acupuncture and Traditional Chinese Medicine (TCM) provide a holistic approach to managing perimenopause symptoms.
While everyone experiences the perimenopause transition differently, it is common to have disruptive perimenopausal symptoms that can affect your physical and emotional well-being. Acupuncture and herbs can help balance hormones, regulate the menstrual cycle, reduce stress, restore energy, and improve your quality of life.
What Is Perimenopause?
Perimenopause refers to the years leading up to menopause, when hormone levels, particularly estrogen and progesterone, begin to fluctuate. This transition often begins in a woman’s 40s, but can start earlier.
Perimenopause can last several years, with symptoms gradually intensifying until menstruation stops completely. “Menopause” is defined as having gone 12 months without a period, which means it technically is just one day! Most people with periods will experience perimenopause for years, and then be “post-menopausal” for up to a third of their lifetime.
Some doctors will recommend hormone replacement therapy (HRT) or medications to target specific symptoms. For some women, HRT is not recommended, due to their medical history. And some women prefer natural, non-pharmaceutical approaches.
Acupuncture and Chinese herbal medicine work by addressing the underlying imbalances that contribute to perimenopausal symptoms, offering a safe and effective alternative or adjunct treatment to hormone therapy.
Top 12 Most Common Perimenopause Symptoms

TCM practitioners look for diagnostic patterns based on the range of symptoms an individual is experiencing and then creates a treatment plan to balance the organ systems and correct the root problem that is causing them. With menopause and perimenopause, typical TCM diagnosis might be:
- liver and kidney yin deficiency
- kidney yang deficiency
- both yin and yang kidney deficiency
- disharmony of heart and kidney
- liver stagnation and spleen deficiency
- stagnation of liver qi
Insomnia
Trouble falling or staying asleep is one of the most common complaints in perimenopause. In TCM, sleep disruption often reflects Yin deficiency (lack of cooling, nourishing energy) or Heart–Kidney disharmony. Acupuncture helps calm the Shen (spirit) and regulate the nervous system, while herbal formulas and dietary guidance focus on nourishing Yin and calming the mind. Simple lifestyle suggestions—reducing late-day stimulants, winding down with gentle stretching or qigong, and keeping a cool, dark bedroom—are part of an integrated plan.
Anxiety
Perimenopausal anxiety often shows as persistent worry, tension, or a feeling of being “on edge.” From a TCM point of view this is frequently Liver Qi stagnation or Heart Shen disturbance. Acupuncture points to move Liver Qi and settle the heart, paired with calming herbs and breath-work, can substantially reduce anxiety and the physical tension that accompanies it.
Depression
Low mood or persistent sadness (depression) may be linked in TCM to Liver Qi stagnation, Spleen Qi weakness (fatigue and poor appetite), or Heart blood deficiency. Treatment is individualized: acupuncture to regulate the flow of Qi, herbal formulas to strengthen the Spleen and nourish the Heart, and lifestyle counseling—regular movement, sunlight, and social support—are all used to lift mood and restore resilience.
Itching / Pruritis
Itchy skin in perimenopause can be triggered by hormone-related dryness or underlying heat from Yin deficiency. TCM treats this by nourishing Yin, clearing deficient heat, and resolving any skin dampness. Topical herbal washes, internal formulas that nourish fluids, and acupuncture to balance the Skin and Lung channels are commonly used approaches.
Joint Pain (including hip and shoulder pain, frozen shoulder)
Joint aches and stiffness often flare during perimenopause, due to declining Yin and Lubrication for the tendons and joints. TCM diagnoses may include Wind-Cold-Damp invasion or Kidney/Liver deficiency affecting the sinews. Local and distal acupuncture, moxibustion when cold is involved, herbal anti-inflammatory formulas, and therapeutic tuina or gentle mobilization help reduce pain, improve circulation, and restore range of motion.
Hip Pain
In TCM, hip pain is frequently associated with Kidney deficiency (which governs the bones and joints) or Blood stasis. Treatments focus on nourishing Kidney essence and moving blood to relieve stiffness and referred pain. Clinical outcomes are often improved when acupuncture is combined with targeted exercises for hip stability.
Shoulder Pain / Frozen Shoulder
Frozen shoulder is treated as a painful obstruction (a kind of Bi syndrome) in TCM. Needling local shoulder points together with distal points that move Qi and break up stagnation can help restore mobility. Repeated, gentle treatment sessions with acupuncture, adjunct cupping or gua sha, and rehabilitative stretching often bring gradual, sustained improvement.
Acne
Hormone-driven acne in perimenopause can result from Liver Qi stagnation transforming into Heat or from Phlegm-Damp accumulation. TCM treatment clears Heat, transforms Phlegm, and supports digestion (the Spleen) so skin eruptions calm. Herbal formulas tailored to the pattern, dietary adjustments (reducing spicy/fried foods and dairy for some people), and acupuncture to regulate hormones are commonly used.
Brain Fog
Difficulty concentrating, forgetfulness, and mental fog often accompany hormonal transitions. In TCM this can be modeled as Qi and blood not adequately nourishing the brain (the “Sea of Marrow”), or as Kidney essence declining. Acupuncture to improve circulation and nourish Yin and blood, herbal support to improve mental clarity, and lifestyle strategies (sleep hygiene, structured routines, mild aerobic exercise) are used together to sharpen cognition.
Irregular Periods
Perimenopause often brings irregular cycles, heavier or lighter bleeding, and spotting. In TCM irregular menses result from Liver Qi stagnation, blood deficiency, or Yin-Yang imbalance. Treatment aims to regulate the menstrual cycle by harmonizing Liver and Spleen, nourishing blood, and, when needed, cooling excess heat. Acupuncture can help re-establish more predictable cycles over time while herbs address the underlying pattern.
Fatigue
Persistent low energy is commonly related to Spleen Qi deficiency in TCM (poor digestion and energy extraction) or to Kidney depletion. Acupuncture protocols focus on strengthening Spleen Qi and boosting overall vitality; herbs like astragalus-based formulas and dietary adjustments—regular, nourishing meals—support long-term recovery.
Hot Flashes and Night Sweats
Perhaps the most classic perimenopausal complaint, hot flashes reflect Yin deficiency with relative heat in TCM theory. Acupuncture has a strong evidence base for reducing the frequency and severity of hot flashes by modulating autonomic balance and calming the underlying deficient heat. Herbal formulas that nourish Yin and clear deficient heat, combined with dietary/lifestyle strategies (cooling foods, layered clothing, avoiding triggers), round out the approach.
Can Acupuncture Help Perimenopause?

Multiple clinical trials and systematic reviews support acupuncture’s effectiveness for common perimenopausal symptoms. For instance, a randomized controlled trial examining perimenopausal insomnia found that acupuncture significantly improved sleep quality, total sleep time, and reduced time to fall asleep compared to control groups. Another systematic review evaluating acupuncture for comorbid insomnia and depression reported moderate to strong benefits in sleep metrics and mood with low risk of adverse events.
In addition to the sleep and mood benefits, acupuncture has been studied for vasomotor symptoms (hot flashes). A meta-analysis pooling several trials showed that acupuncture reduced the frequency and severity of hot flashes more than sham acupuncture and often matched hormone therapy in effect size, with fewer side effects. These studies underscore acupuncture’s potential not only to alleviate surface symptoms but also to exert beneficial regulatory effects on hormonal and autonomic systems.
Perimenopause is a highly individual transition; two people can have the same complaint (like insomnia or hot flashes) for very different energetic reasons. That’s why TCM emphasizes tailored treatment—your acupuncture points, herbs, and lifestyle plan are selected based on your unique pattern. Acupuncture offers real physiologic benefits (calming the nervous system, improving sleep architecture, reducing inflammation) while herbs and diet support deeper rebuild of Yin, Blood, and Digestive Qi. Regular treatments over several months are often most effective, with maintenance “tune-ups” to keep symptoms at bay.
If you’re struggling with perimenopausal symptoms, acupuncture and TCM can be a safe, effective complement to conventional care. At Art of Wellness we create personalized plans that combine acupuncture, Chinese herbal therapy, nutritional guidance, and qigong to help you move through this transition more comfortably and regain balance.
Acupuncture Near Me for Perimenopause in West Los Angeles
If perimenopause is impacting your sleep, mood, skin, joints or day-to-day energy, please don’t hesitate to reach out. We’re happy to schedule a consultation to review your symptoms, discuss a personalized TCM treatment plan, and answer any questions about how acupuncture and herbal medicine can support you through this phase of life. Call or book online to get started.
At Art of Wellness Acupuncture in Santa Monica, we specialize in women’s health and menopause care. If you are experiencing symptoms of perimenopause, reach out today to schedule a consultation. Together, we can create a personalized treatment plan to help you feel more like yourself again.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Insulin Resistance With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Hungry and tired all the time? Gaining weight even though you’re doing all the right things? These may be signs of insulin resistance. Acupuncture and TCM offer alternative treatment to help improve insulin sensitivity and support weight loss.
What Is Insulin Resistance?
Insulin resistance is a condition where your body’s cells stop responding well to insulin, leading to elevated blood sugar levels and a cascade of metabolic stress. Left unchecked, insulin resistance can lead to prediabetes, type 2 diabetes, cardiovascular disease, and trouble managing a healthy weight.
Insulin is a hormone produced by your pancreas that helps glucose (sugar) enter cells for energy. When your body becomes resistant to insulin, more insulin is needed to keep blood sugar in a normal range. Over time, the pancreas struggles to keep up, and blood glucose levels rise.
Insulin resistance often shows up with other health problems, such as high triglycerides, low “good” HDL cholesterol, elevated fasting glucose, and sometimes high blood pressure. There may not be obvious symptoms at first, which is why many people have insulin resistance for years before they are ultimately diagnosed.
Insulin resistance is often a significant part of PCOS, which causes irregular periods and fertility issues, along with increasing the risk of diabetes. Acupuncture and TCM can be an effective way to treat PCOS and insulin resistance.
Top 10 Signs of Insulin Resistance

How do I know if I’m insulin resistant? Many people will not notice any signs of insulin resistance and will find out about it until they have a fasting blood glucose test or tests that show high cholesterol levels.
However, there are symptoms that may be indicators of insulin resistance:
- Increased hunger, especially after meals
- Frequent energy crashes or feeling tired even after rest
- Frequent urination
- Difficulty losing weight or belly fat accumulation
- Darkened skin patches (acanthosis nigricans), especially around the neck or underarms
- Elevated fasting glucose or hemoglobin A1c (if tested)
- High triglycerides, low HDL cholesterol
- Possible mild elevated blood pressure
- Fatigue
- Dizziness, headaches
Can Acupuncture Help Insulin Resistance?
In Traditional Chinese Medicine, insulin resistance is seen not just as issues with sugar, but as a broader imbalance among Qi (vital energy), Blood, Yin, and Yang, often involving the Spleen, Liver, and Kidneys.
Spleen Qi Deficiency – the Spleen is responsible for transforming food into energy. Weak Spleen Qi means sluggish digestion, poor nutrient absorption, and accumulation of Dampness.
Phlegm-Damp Obstruction – in TCM, phlegm/damp corresponds loosely to fat accumulation, insulin-resistant fat tissue, or lipid disturbances.
Liver Qi Stagnation – can lead to emotional stress, which worsens metabolism, contributes to cravings, and disrupts hormonal balance.
Kidney Yin or Yang Deficiency – either or both depending on the person’s constitution and lifestyle. This can impair energy reserves, slow recovery, and reduce resilience.
TCM treatment is thus about addressing both root (constitutional) imbalances and branch (symptomatic) relief: strengthening digestion (Spleen), moving liver Qi, clearing dampness, nourishing the kidneys, and regulating blood sugar and energy.
Recent research has begun to show how acupuncture can directly influence the mechanisms behind insulin resistance, not just the symptoms.
A comprehensive review of both clinical and laboratory studies found that acupuncture helped improve common measures of insulin sensitivity, such as fasting blood glucose, insulin levels, and the HOMA-IR index. Patients who received acupuncture also saw improvements in cholesterol and triglyceride levels, reductions in abdominal fat, and better liver function in cases of non-alcoholic fatty liver disease.

Chinese herbal formulas are tailored to each pattern—some patients may need herbs to strengthen the Spleen and resolve dampness; others might need formulas to soothe liver Qi, or nourish Yin or Yang depending on their pattern.
Diet in TCM is also crucial. Reducing sugar, refined carbohydrates, avoiding damp-producing foods, and choosing foods that support spleen function (warm, simple, easy to digest) will help, and your practitioner can give you specific dietary advice.
Lifestyle practices such as gentle exercise, stress reduction (meditation, breathing work), good sleep hygiene, and regular rest help reinforce the effects of acupuncture and herbs.
Acupuncture Near Me for Insulin Resistance in Los Angeles
If you suspect you’re dealing with insulin resistance, or if you’ve been diagnosed with prediabetes, type 2 diabetes, or PCOS, acupuncture and TCM can be helpful. At Art of Wellness Acupuncture in West Los Angeles, we tailor our treatments to your unique situation, addressing the root causes and supporting sustainable metabolic health.
Don’t wait until medication is your only option. Contact us today to schedule a consultation and see how acupuncture and TCM may support your journey toward improved insulin sensitivity, balanced hormones, and healthier weight.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Syncope With Acupuncture and TCM
By Xiaomei Cai, L.Ac., Ph.D. and Qineng Tan, L.Ac., Ph.D.

Lightheaded and dizzy? Passing out for no reason or fainting without warning? Syncope, or vasovagal passing out due to a loss of blood flow to the brain, is also known as a vasovagal attack. Acupuncture can help regulate the autonomic nervous system and blood flow to prevent fainting and syncope.
A syncope episode, or vasovagal passing out, can be scary for the person fainting and for the people around them, because it happens suddenly. Usually, the fainting spell only lasts for a minute or two. The underlying causes of syncope can be complex, involving the nervous system, heart, or circulatory system.
What Causes Syncope?
Syncope definition: The term “syncope” refers to a temporary loss of consciousness due to reduced blood flow to the brain. One of the most common forms, vasovagal syncope, occurs when the vagus nerve triggers a sudden drop in blood pressure and heart rate.
A vasovagal attack happens when a trigger, such as stress, pain, standing too long, or sudden changes in posture, causes the vagus nerve to send signals that lower heart rate and dilate blood vessels. Blood pressure drops, less blood reaches the brain, and the person loses consciousness.
Other types of syncope may be caused by cardiac arrhythmias, orthostatic hypotension, or neurological conditions.
Top 5 Symptoms of Syncope

Although fainting often comes on suddenly, many people who suffer from fainting vasovagal syncope notice warning signs beforehand. Signs that a vagal attack is imminent may include:
- Feeling lightheaded or dizzy
- Sudden nausea, queasiness
- Blurred vision, tunnel vision
- Cold, clammy skin, sweating, flushing, or sudden pallor
- Ringing in the ears (tinnitus) or muffled hearing
Afterward, some people feel tired, weak, or mentally foggy for a few minutes or a few hours.
Syncope Diagnosis
When someone has been experiencing fainting spells, a physician will usually try to identify whether the cause is cardiac, neurological, or vasovagal in origin. Tests may include ECG, echocardiography, tilt-table testing, or blood work.
If episodes are vasovagal, standard recommendations include:
- Avoiding known triggers like dehydration, overheating, or standing still for long periods
- Learning counter-pressure maneuvers (such as leg crossing or hand gripping) to increase blood pressure during early warning signs
- Medications such as beta-blockers or fludrocortisone in severe or frequent cases
- In rare cases, pacemaker implantation
While these recommendations for syncope can reduce fainting episodes, they may not always address the underlying autonomic imbalance. Acupuncture and TCM can provide a more holistic solution that addresses the deeper issues that are leading to vasavagal passing out.
Can Acupuncture Help Syncope?
In Traditional Chinese Medicine, fainting is often considered to be a sudden loss of consciousness due to Qi deficiency, Qi and Blood stagnation, or excess pathogenic factors disrupting the flow of energy to the head.
Some common TCM patterns that may underlie syncope include:
- Qi and Blood Deficiency – When the body lacks nourishment, the brain is deprived, leading to dizziness and collapse.
- Liver Qi Stagnation with Heat – Emotional stress and tension cause sudden disruptions of the flow of Qi, triggering fainting spells.
- Phlegm-Damp Obstruction – Excess dampness and phlegm block clear Yang from rising, clouding the head.
- Excess Wind or Cold – External factors can constrict channels, cutting off circulation to the brain.
An acupuncture practitioner will focus their treatment protocol on balancing pathogenic forces, such as wind and cold, or heat and dampness, and strengthening Qi energy to prevent recurrence of fainting and dizziness.

Acupuncture is an excellent modality for helping to stabilize blood pressure and regulate vagal activity and the autonomic nervous system.
In addition to acupuncture, herbal formulas may be prescribed to strengthen Qi, clear heat, resolve phlegm, or calm the Shen (spirit). Therapies such as cupping, gua sha, and breathing exercises can also support circulation and prevent stagnation.
Several studies have shown that acupuncture can reduce fainting episodes and improve autonomic stability.
Recent research is helping modern medical science better understand that the autonomic nervous system is, perhaps, one of reasons that acupuncture works. The needling of acupuncture points stimulate sensory nerve fibers, which are connected throughout the body, as signals moving along the spinal cord to and from the brain.
This is what allows for acupuncture treatment to positively affect the brain, nervous system activity, relieve pain, and reduce inflammation throughout the body.
One study concluded that acupuncture can affect autonomic responses by activating parts of the brain when the sympathetic and sympathetic nervous system activities are out of balance.
A study looked at the use of acupuncture as an emergency treatment for syncope and found that the effect of acupuncture treatment for helping to normalize blood pressure and heart rate and bring the body back into homeostasis.
Another study followed three patients with syncope, with different presentations, according to TCM diagnostic criteria (yin deficiency, yang deficiency, and excess phlegm with qi deficiency). All three patients found relief from their symptoms after receiving individualized treatment with acupuncture and herbs.
Acupuncture Near Me for Syncope in Los Angeles
Living with syncope or vasovagal fainting can feel limiting and unpredictable. Acupuncture and TCM provide time-tested methods to calm the nervous system, restore healthy circulation, and strengthen your overall resilience. If you or someone you know struggles with fainting or frequent dizziness, integrative care can provide relief and help you regain a sense of stability. Contact Art of Wellness Acupuncture today to schedule a consultation and learn how acupuncture can help you prevent syncope episodes and feel more balanced and secure in your daily life.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Tingling in one arm? Stiff neck and shoulder? Neck pain or headache back of head? These can be symptoms of thoracic outlet syndrome (TOS), or compression of the nerves and blood vessels that run through the neck and shoulder. Acupuncture and TCM offer thoracic outlet treatment to help relieve pain and numbness in the arm and hand.
Tingling pain and weakness in the arm and hand are the most common signs of thoracic outlet compression syndrome. You might wake up with pins and needles in your arm, or have a feeling of weakness in your hand after lifting things overhead or working for long hours at your computer.
What Causes Thoracic Outlet Syndrome?
There is a narrow space between your top rib and your collarbone, known as the thoracic outlet, through which a complex network of nerves and vessels run, connecting the neck and shoulder to the arm.
These nerves and arteries can become constricted due to tight or misaligned muscles (particularly the scalene or pectoralis minor), poor posture, or repetitive movements at work or while participating in a sport, resulting in impaired circulation, and nerve irritation.
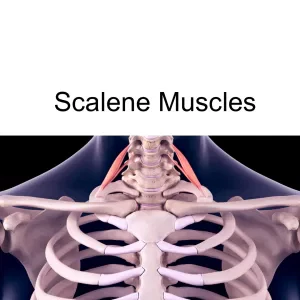
The three scalene muscles (anterior, middle, and posterior) attach the cervical vertebrae of the neck to the top two ribs. Key blood vessels (the brachial plexus, subclavian artery and vein) run through the narrow space between the scalene muscles. When these muscles become tight or pushed out of their proper alignment, this can cause compression or entrapment of the blood vessels, affecting blood flow and sometimes also putting pressure on the ulnar nerve, which extends from the neck all the way down to the hand.
Injury or trauma to the area due to a car accident (such as whiplash) could lead to thoracic outlet syndrome. Sports injuries or simply the repetitive movements involved in a sport could cause thoracic outlet syndrome to develop, particularly movements where the arm is extended above the head, as in swimming or baseball. Physical changes that occur during pregnancy and affect the posture can also aggravate nerves and blood vessels.
People with Ehlers-danlos syndrome may be more prone to developing thoracic outlet syndrome because of instability in the shoulder girdle.
In rare cases, a person might have an extra rib or other anatomical variation, which can contribute to TOS.
Top 10 Symptoms of Thoracic Outlet Syndrome
Symptoms of thoracic outlet compression syndrome can come and go and change over time. Common signs include: tingling and numbness in ring finger or pinky finger, pain in neck, pain in shoulder blade, soreness in the armpit or front of chest.
Common symptoms of thoracic outlet:
- Tingling, numbness, or a “pins and needles” sensation in the arm or hand
- Feeling of fatigue in the arm, or arm feels heavy
- Weakness in the hand grip or difficulty lifting objects, loss of fine motor skills in the hand, clumsiness, dropping things
- Aching pain or tenderness and sensitivity in the neck, shoulder, collarbone or chest, sometimes radiating down the arm
- Shoulder appears to be drooping, slumped posture
- Swelling, discoloration, and/or a sensation of cold in the affected arm or hand
- Headaches, especially pain in the back of the head, headache at the base of the skull
- Loss of muscle in the base of the thumb
- Weak pulse in the affected arm
- Blood clots or deep vein thrombosis
Symptoms like tingling and weakness of the arm and hand usually become worse after the arm has been in an elevated position, performing activities that require the arm to be raised over the head.
Signs of thoracic outlet syndrome can appear similar to those of other conditions, like carpal tunnel syndrome, cubital tunnel syndrome, cervical radiculopathy, or other cervical spine issues. Some of the symptoms of thoracic outlet syndrome are also similar to the symptoms of a heart attack.
Typical Thoracic Outlet Syndrome Therapies
Diagnosis of TOS generally begins with a detailed medical history and physical exam, in which maneuvering the arm or neck rotation may reproduce symptoms. Imaging tests such as X-rays, MRI, CT scans, or Doppler ultrasound help assess anatomical contributors and vascular involvement. Nerve conduction studies can also confirm nerve compression.
Conventional treatment for thoracic outlet syndrome typically starts conservatively. A central focus is on physical therapy, aimed at stretching tight muscles, improving posture, and strengthening supportive muscle groups. Pain may be managed with medications like NSAIDs or muscle relaxants. If symptoms persist or worsen, interventions such as targeted injections (e.g., botulinum toxin into tight scalene muscles) or surgical options (like first-rib resection) may be suggested.
These methods can offer relief, especially when implemented early. Still, recovery can be prolonged and some patients may experience recurring symptoms. Acupuncture and TCM offer alternative management for thoracic outlet syndrome.
Can Acupuncture Help Thoracic Outlet Syndrome?

In Traditional Chinese Medicine, thoracic outlet syndrome is viewed as a problem of Qi (energy) and blood stagnation within the meridians that traverse the neck and shoulders, especially the Liver, Gallbladder, and Lung channels. Emotional stress, poor posture, or physical strain may disrupt the smooth flow of Qi, leading to obstructions that manifest as pain, numbness, or movement difficulty.
Additional contributing factors may include Wind-Cold-Damp invasion, which contracts muscles; Liver Qi stagnation, which impairs flexibility; and Spleen or Kidney weakness, which fails to support the body’s structural integrity and recovery.
TCM addresses both the symptomatic blockage and the deeper systemic imbalances underlying the condition.
TCM Treatment for Thoracic Outlet Syndrome
TCM takes a multi-dimensional approach to treating TOS. Acupuncture uses fine needles to stimulate key points that encourage the release of stagnant Qi and improve blood flow.
Cupping and Gua Sha techniques help soften fascia, reduce muscle tension, and encourage lymphatic and blood circulation.
Herbal formulas may include herbs that invigorate blood, relax sinews, and strengthen muscles and fascia.
Lifestyle changes, emphasizing improved posture, ergonomic adjustments, mindful movement, stress management, and dietary tips can help reduce inflammation and support healing.
Controlled trials and case studies suggest acupuncture effectively reduces pain and improves function in conditions involving neurovascular compression. For instance, a controlled study published in 2019 reported significant decreases in pain and disability among patients receiving acupuncture for TOS symptoms.
Another case study found that acupuncture combined with TCM herbal therapy provided thoracic outlet syndrome relief by alleviating shoulder tightness, restoring flexibility, and reducing numbness.
Several clinical groups are exploring acupuncture-mediated modulation of microcirculation, inflammatory markers, and nerve conduction—underscoring its role as a promising complement to standard care.
Acupuncture Near Me for Thoracic Outlet Syndrome in West Los Angeles
TCM modalities are excellent for helping to relieve pain and tingling and improving range of motion for a wide variety of conditions. Acupuncture can provide symptom relief and fundamental improvement of conditions like nutcracker syndrome, carpal tunnel syndrome, cubital tunnel, syndrome, nerve pain, shoulder pain, neck pain, and thoracic outlet syndrome. Drs. Tan and Cai at Art of Wellness in Santa Monica/West Los Angeles have over 35 years of experience in treating vascular and nerve conditions.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.


