By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Fast heart rate or irregular heartbeat? Feel faint or dizzy when standing up? Fatigue, brain fog? Chest pain? These can all be Dysautonomia symptoms, or autonomic dysfunction. Acupuncture and TCM offer treatment for dysautonomia and autonomic neuropathy.
“Dysautonomia” is a general term that refers to multiple conditions related to autonomic dysfunction. There are many different types of autonomic nervous system disorders that fall under the umbrella of dysautonomia.
The autonomic nervous system (ANS) controls body functions like:
- Blood pressure
- Heart rate
- Breathing
- Digestion
- Temperature regulation
- Urinary function
- Sexual function
- Sweating
Basically, the ANS is in charge of all of the things our bodies do automatically—sometimes called involuntary functions—without us having to think about them.
Dysautonomia symptoms are fairly common, especially later in life, but medical science still has limited options for diagnosing and helping relieve these conditions.
Dysautonomia can be a primary condition, caused by genetic or degenerative disorders, or by damage to nerves (autonomic neuropathy). Secondary dysautonomia can occur as a result of another condition, such as an autoimmune disease, neurological disease, or injury.
Recent studies are beginning to show that dysautonomia, especially POTS, can be linked to long Covid. Even if a person had a Covid infection that was not particularly severe, the long-term effects of the virus have been shown to linger in the body, in the brain and nervous system, causing autonomic dysfunction long after the acute phase of the virus has passed.
TCM offers a way to treat dysautonomia, as acupuncture has been shown to have a positive effect on nervous system function.
Dysautonomia Symptoms
Different types of autonomic dysfunction will cause various symptoms in individuals. The most common symptoms of ANS include:
- Dizziness when standing up or changing position, light-headedness
- Vertigo
- Fainting, passing out
- Arrhythmia, irregular heartbeat, heart palpitations
- Fatigue, feeling tired
- Chest pain
- Shortness of breath
- Trouble swallowing
- Excessive sweating, or lack of sweating, clammy feeling
- Thirst
- Headaches, migraines
- Dry eyes, or excessive tears
- Digestive issues: constipation, diarrhea, etc.
- Frequent urination, incontinence
- Erectile dysfunction (ED)
- Sensitivity to sounds
Top 10 Types of Autonomia

Dysautonomia symptoms can seem similar to those of other nervous system conditions. This is why it can be difficult to be correctly diagnosed. It is fairly common for a person presenting with symptoms of dysautonomia to be told that they are suffering from anxiety or panic disorder.
Secondary dysautonomia occurs when another condition is the cause of symptoms. For example, dysautonomia systems can be the result of having disorders, such as:
- Parkinson’s disease
- Ehlers-Danlos Syndrome
- Celiac disease
- Guillain-Barre syndrome
- Lupus
- Lyme disease
- Sjogren’s syndrome
- Ulcerative Colitis
- Multiple Sclerosis (MS)
- Rheumatoid arthritis
- Sarcoidosis
- Crohn’s Disease
- IBS
- Fibromyalgia
These conditions can all cause damage to parts of the autonomic nervous system and therefore lead to symptoms of Dysautonomia.
There are at least 15 different types of Primary Dysautonomia. POTS is probably the most common one.
POTS Postural Orthostatic Tachycardia Syndrome – POTS is a condition characterized by an excessive increase in heart rate when moving from lying down to standing up (orthostatic intolerance). Symptoms may include lightheadedness, palpitations, fatigue, and fainting. It often affects young adults, particularly women.
Hyperadrenergic POTS is a subtype of POTS characterized by excessive sympathetic nervous system activity, leading to symptoms such as palpitations, anxiety, tremors, and hypertension in addition to orthostatic intolerance.
Treatment for POTS often involves a combination of lifestyle modifications, medications, and physical therapy. Lifestyle changes may include increasing fluid and salt intake to expand blood volume, wearing compression stockings to prevent blood pooling in the legs, and gradually increasing physical activity to improve cardiovascular fitness. Medications such as beta-blockers, fludrocortisone, midodrine, and pyridostigmine may be prescribed to help regulate heart rate, blood pressure, and blood volume.
IST Inappropriate Sinus Tachycardia – Inappropriate Sinus Tachycardia (IST) is a condition characterized by a fast heart rate at rest that is not caused by exercise, fever, or stress. It is considered inappropriate because the heart rate is elevated without a physiological reason. People with IST typically experience heart rates exceeding 100 beats per minute while at rest, often accompanied by symptoms such as palpitations, chest discomfort, fatigue, and shortness of breath.
The exact cause of IST is not fully understood, but it is believed to involve dysfunction in the sinus node, the natural pacemaker of the heart, which regulates heart rate. In individuals with IST, the sinus node may become overly sensitive to normal stimuli, leading to excessive firing and a rapid heart rate.
Treatment for IST focuses on controlling symptoms and improving quality of life. Lifestyle modifications like stress reduction, regular exercise, and avoiding triggers such as caffeine and nicotine may be recommended. Medications such as beta-blockers, calcium channel blockers, or ivabradine may be prescribed to help slow the heart rate and alleviate symptoms. In severe cases that do not respond to medication, procedures such as catheter ablation may be considered to modify the electrical pathways in the heart and reduce symptoms.
NCS Neurocardiogenic Syncope or Vasovagal Syncope – NCS, also known as vasovagal syncope, is a form of dysautonomia characterized by a sudden drop in heart rate and blood pressure, leading to fainting. It can be triggered by various factors such as prolonged standing, emotional stress, or pain.
Management of NCS focuses on avoiding triggers like prolonged standing, dehydration, or emotional stress, which can lead to fainting episodes. Increasing fluid and salt intake may help prevent episodes by expanding blood volume. Medications such as beta-blockers or fludrocortisone may be prescribed to help stabilize heart rate and blood pressure. In severe cases, implantation of a pacemaker or other cardiac device may be considered to regulate heart rhythm.
AAG Autoimmune Autonomic Ganglionopathy – AAG is a rare autoimmune disorder characterized by the production of antibodies that target autonomic ganglia, leading to autonomic dysfunction. Symptoms may include orthostatic hypotension, gastrointestinal dysmotility, and urinary dysfunction.
MSA Multiple System Atrophy – Management of MSA is focused on addressing specific symptoms related to autonomic dysfunction, parkinsonism, and cerebellar ataxia. Medications such as levodopa-carbidopa may be prescribed to alleviate motor symptoms, while medications such as fludrocortisone or midodrine may be used to manage orthostatic hypotension. Physical therapy and speech therapy may also be beneficial for managing motor and speech difficulties associated with MSA.
Management of MSA is focused on addressing specific symptoms related to autonomic dysfunction, parkinsonism, and cerebellar ataxia. Medications such as levodopa-carbidopa may be prescribed to alleviate motor symptoms, while medications such as fludrocortisone or midodrine may be used to manage orthostatic hypotension. Physical therapy and speech therapy may also be beneficial for managing motor and speech difficulties associated with MSA.
PAF Pure Autonomic Failure – PAF is a rare condition characterized by dysfunction of the autonomic nervous system, leading to problems with blood pressure regulation, heart rate variability, and temperature control. Symptoms may include orthostatic hypotension, urinary retention, and gastrointestinal issues.
Treatment for PAF aims to manage symptoms related to autonomic dysfunction. Lifestyle modifications like elevating the head of the bed, wearing compression garments, and increasing fluid and salt intake may help alleviate symptoms of orthostatic hypotension. Medications such as midodrine, fludrocortisone, and droxidopa may be prescribed to raise blood pressure and improve symptoms.
FD Familial Dysautonomia – begins at birth as a result of a genetic mutation inherited from the parents. FD affects the central nervous system, breathing, digestion, ability to form tears, regulation of temperature, regulation of blood pressure, taste, and pain sensitivity. Usually diagnosed in infancy, as babies will have trouble with feeding, will not cry tears, and will show poor growth. As the disease progresses, there may be development of arrhythmia, GERD, dry eyes and vision problems, scoliosis and/or weak bones.

DBHD Dopamine-Beta Hydrolase Deficiency – a rare genetic disorder characterized by the body’s inability to produce the enzyme dopamine-beta hydroxylase (DBH). This enzyme is essential for converting dopamine to norepinephrine, a neurotransmitter involved in regulating blood pressure and other autonomic functions.
Treatment for DBH deficiency focuses on managing symptoms by increasing fluid and salt intake to help maintain blood pressure, wearing compression garments to reduce symptoms of orthostatic hypotension, and avoiding triggers such as hot environments and prolonged standing.
In some cases, medications that increase blood volume or constrict blood vessels may be prescribed to help alleviate symptoms. However, treatment options for DBH deficiency are limited, and management typically involves ongoing monitoring and adjustment of therapies to address specific symptoms and complications as they arise.
OI Orthostatic Intolerance – Orthostatic intolerance (OI) refers to a group of conditions characterized by symptoms such as lightheadedness, dizziness, fatigue, and fainting when a person moves from lying down into an upright position.
There are various types of orthostatic intolerance, including postural orthostatic tachycardia syndrome (POTS), neurally mediated hypotension (NMH), and vasovagal syncope. Each type presents with its own set of symptoms and underlying mechanisms.
Besides lifestyle modifications such as increasing fluid and salt intake, wearing compression garments, and engaging in regular exercise can help improve blood flow and cardiovascular function, medications such as beta-blockers, fludrocortisone, and midodrine may also be prescribed to help regulate heart rate and blood pressure.
BF Baroreflex Failure – Baroreflex failure is a condition characterized by the inability of the body to regulate blood pressure in response to changes in posture or stress. It can result in symptoms such as orthostatic hypotension, hypertension, and fluctuations in heart rate.
Can Acupuncture Help Dysautonomia?
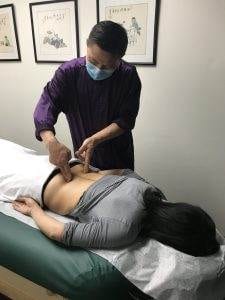
From the perspective of conventional medicine, dysautonomia is still considered a mysterious, confusing problem to solve. But TCM philosophy has recognized this type of disorder for many centuries. Acupuncture has been used since ancient times to help regulate the autonomic nervous system, although we have not always used that terminology for it.
A Chinese medical text that dates back to the first century B.C.E. describes “Ying-Wei Disharmony,” the symptoms of which include: breathing dysfunction, palpitations, irregular heartbeat, anxiety, digestive problems, nausea, dizziness, chronic pain, pressure headaches, tingling and numbness (neuropathy), and insomnia.
For a long time, medical science has looked for the mechanisms that make acupuncture work.
Recent studies have begun to show more clearly that the stimulation of acupoints affects the neural pathways, including the autonomic nervous system.
Acupuncture has been shown to help regulate ANS functions such as temperature regulation, blood pressure, heart rate, and muscle sympathetic nerve activities.
Acupuncture helps modulate transmitters in the brain, restoring balance when these activities have become dysregulated. More specifically, electro-acupuncture has been shown to work upon the hypothalamus, the medulla oblongata, the dorsomedial prefrontal cortex, and other regions of the brain that contribute to ANS function.
One study involving 30 female patients with dysautonomia symptoms showed that acupuncture treatment helped relieve heart palpitations, abdominal issues, and helped patients sleep better.
In addition to helping to regulate the autonomic nervous system, an acupuncturist will look for signs that other organ systems are out of balance and contributing to symptoms. For example, some patients with dysautonomia may need acupuncture and herbs to help balance the spleen and kidneys, which will in turn help improve adrenal function.
Stagnation of blood or phlegm can sometimes be causing blockages that contribute to nervous system dysfunction.
Acupuncture Near Me for Dysautonomia in Los Angeles Area
Dysautonomia is a complex condition to treat. A multi-faceted approach, combining conventional medical approaches with medications with acupuncture and herbal remedies can be helpful for managing the variety of symptoms a person may be experiencing. TCM is an excellent modality for working with this type of condition. If you or someone you know is struggling to get help for POTS or other autonomic disorders, call us at Art of Wellness in West L.A..
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.

