-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

May 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31
Moxibustion
How To Treat Addison’s Disease With Acupuncture and TCM
By Qineng Tan, L.Ac,. Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Always tired? Craving salty foods? Thirsty all the time? Adrenal fatigue? Addison’s disease is a condition in which the adrenal glands do not produce enough cortisol. Acupuncture and TCM can help to balance the adrenal hormones and relieve adrenal insufficiency symptoms.
Addison’s, also known as adrenal insufficiency, happens because of damage to the adrenal glands. What do the adrenal glands do? The adrenals are small glands that are located just above the kidneys. They produce hormones, including cortisol and aldosterone. These hormones are important in metabolic functions, and are also a big part of our stress response.
Cortisol is released from the adrenal glands into the bloodstream, and it aids in the body’s use of macronutrients: protein, carbohydrates, and fats. Cortisol regulates blood pressure and blood sugar levels, and it also gives us an extra energy boost when we need it because of sudden and/or stressful circumstances.
In many cases, Addison’s disease is the result of an autoimmune disorder. In these cases, the immune system mistakenly attacks the adrenal cortex, the part of the adrenal glands that produce cortisol and aldosterone.
In some parts of the world, tuberculosis infection is still common, and tuberculosis can lead to damage of the adrenal glands.
Other infectious diseases like HIV/AIDS, or fungal infections like histoplasmosis, can cause adrenal damage.
People with other autoimmune diseases may be more susceptible to developing Addison disorder, too. For example, Addison’s disease can happen concurrently with:
- Dermatitis herpetiformis
- Graves disease
- Type 1 diabetes
- Pernicious anemia
- Hashimoto’s disease, thyroiditis
- Vitiligo
- Myasthenia gravis
Some people may develop Addison’s disease in addition to having hypothyroidism or diabetes.
Addison’s Disease Symptoms

In the early stages, Addison’s disease symptoms may feel like a flu, causing fatigue, muscle weakness and joint pain. But as the illness progresses, these symptoms may become chronic.
Adrenal insufficiency symptoms include:
- Extreme fatigue
- Dehydration
- Loss of appetite
- Unexplained weight loss
- Darkening of skin in areas, hyperpigmentation, darkening of gums
- Blue-black color to skin around mouth, nipples, or genitals
- Low blood pressure, hypoglycemia
- Dizziness
- Fainting, light-headedness
- Craving salt
- Abdominal pain
- Nausea, vomiting
- Diarrhea
- Joint pain
- Muscle pain
- Depression
- Irritability
- Loss of body hair
- Sexual problems
- Irregular periods, no menstrual periods, missed periods
Primary ovarian insufficiency (POI), has been found to be more common among those with Addison’s disease, with about 1 in 10 women with Addison’s going through early menopause (before 40).
In extreme situations, Addison’s sickness can lead to kidney failure, or going into shock. Early warning signs of adrenal crisis include nausea, fever, headache, and confusion. This sudden worsening of Addison’s disease is known as Adrenal crisis, and requires immediate medical attention.
Medical Treatment for Addison’s Disease
Accurate diagnosis and appropriate treatment are crucial for individuals with Addison’s disease.
A doctor will typically diagnose Addison’s disease through blood tests. These tests measure the levels of cortisol and aldosterone in the blood. Low levels of these hormones are indicative of adrenal insufficiency.
If blood tests suggest adrenal insufficiency, an ACTH stimulation test may be performed. In this test, synthetic adrenocorticotropic hormone (ACTH) is administered, and cortisol levels in the blood are measured. Patients with Addison’s disease typically do not show a significant increase in cortisol after receiving ACTH.
The primary treatment for Addison’s disease involves hormone replacement therapy. Patients are prescribed synthetic cortisol (usually hydrocortisone or prednisone) to replace the insufficient natural cortisol production.
If aldosterone production is also insufficient, patients may be prescribed fludrocortisone to replace this hormone. This helps regulate salt and water balance in the body.
Dosage and frequency of cortisol replacement are adjusted to meet the specific needs of each patient. Patients often need to take multiple doses of medication daily to mimic the body’s natural cortisol rhythms.
These steroid medications can cause side effects like dizziness, nausea, and changes in the menstrual cycle.
Patients with Addison’s disease require ongoing medical supervision to monitor hormone levels, adjust medication as needed, and ensure that they are responding well to treatment.
Acupuncture offers an adjunct or alternative treatment for Addison’s disease that can help regulate hormones.
Can Acupuncture Help Addison’s Disease?
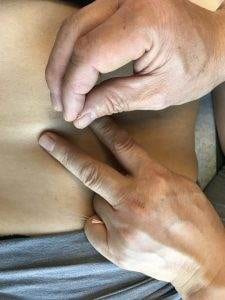
According to TCM theory, the kidneys are responsible for storing and controlling not only Qi, but “essence,” which represents a person’s foundational life force energy.
Addison’s disease, or adrenal insufficiency, is usually related to some variation of kidney deficiency according to TCM diagnosis.
Possible TCM diagnosis for Addison’s might be:
- kidney qi deficiency
- kidney yang deficiency
- kidney yin deficiency
- liver yin deficiency
- spleen blood deficiency
- spleen yang deficiency
By listening to a person’s range of symptoms, an acupuncturist will determine which pattern is emerging, and choose acupuncture points to bring energy and strength to the affected organs.
Moxibustion treatment is also an excellent modality to help build up Kidney Qi and blood.
Chinese herbs can help nourish and support kidney Qi.
For some people, acupuncture treatment and herbal supplements can be a good alternative treatment for Addison’s disease. For others, TCM treatment for adrenal insufficiency can be used as an adjunct to conventional treatment, and help to alleviate side effects of steroids, like dizziness, nausea, or menstrual changes.
Acupuncture Near Me for Addison’s Disease in West Los Angeles
Acupuncture can help address autoimmune diseases that are difficult for conventional medicine to treat. TCM modalities, including moxibustion and herbs, can provide a holistic treatment that works on the root level, restoring proper function of the immune system, as well as helping to relieve all kinds of symptoms.
Addison’s disease requires an individualized approach. Dr. Tan and Dr. Cai at Art of Wellness Acupuncture have over three decades of experience helping patients overcome all types of autoimmune disorders. Art of Wellness was recently named one of the top acupuncture practices in Los Angeles. Please do not hesitate to call us.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Scleroderma With Acupuncture and TCM
By Xiaomei Cai, L.Ac., Ph.D. and Qineng Tan, L.Ac., Ph.D.

Hard, thickening, tight skin? Itchy, dry skin that is shiny? Changing skin color? These could be symptoms of scleroderma, an autoimmune disorder that causes your body to produce too much collagen. Acupuncture and TCM treatment can help relieve inflammation and pain while helping to resolve the underlying cause of scleroderma.
Scleroderma can be considered a type of dermatosis (skin lesion), and also a type of connective tissue disease (negatively impacting tissues that connect structures in the body), as it usually affects skin and cartilage, often starting in the extremities, and then extending up the limbs towards the trunk.
Collagen is a form of fibrous protein that the body produces to maintain the structure of skin cells, muscles, bones, and connective tissue. The immune system triggers collagen production when we are injured, but in the case of scleroderma, the body is overproducing and accumulating too much collagen.
Localized scleroderma affects primarily the skin tissue, but can also spread to subcutaneous tissues, like fascia and muscles.
In some cases, scleroderma can also impact internal organs, like the esophagus, lungs, heart, and kidneys. This is known as systemic scleroderma.
Top 3 Types of Scleroderma
Localized scleroderma can be differentiated into 3 types:
- Localized scleroderma – a few patches of discolored skin (circumscribed morphea); these skin lesions can vary in size, may be oval shaped, and are usually yellow in the center with a red border.
- Generalized scleroderma – also called generalized morphea, with this type there are more patches of thick, hard skin on various parts of the body, which may overlap.
- Linear scleroderma – more common in children, may show up as one band of affected skin on a limb or on the trunk, with a few patches of morphea. Linear scleroderma on arms and legs may affect the growth and development of that limb, as scleroderma may impact the muscle and bone tissues as well as the skin.
Systemic scleroderma is rare, but happens more commonly in women between the ages of 30 and 50. This type of scleroderma can manifest in different ways.
Systemic scleroderma can sometimes first show up as Raynaud’s phenomenon, or Raynaud’s syndrome, in which the blood vessels in the hands and feet close up when the weather is cold and cause color changes to the skin, as well as sensations of numbness, prickling, tingling, or pain. Stress can also trigger Raynaud’s.
Systemic scleroderma can cause scarring on the skin and internal organs, which can lead to gastrointestinal problems like acid reflux, cardiovascular and pulmonary problems, or renal disease.
Acupuncture treatment can be used as an adjunct treatment to help relieve symptoms of pain related to skin hardening, as well as helping to alleviate heartburn and GERD type symptoms in patients with esophageal symptoms of scleroderma. TCM can also help address the root causes of scleroderma and other autoimmune disorders.
What Causes Scleroderma?

As with most autoimmune disorders, medical science has not yet discovered exactly why some people develop this condition. While it is not passed from parent to child the way genetic diseases are, you are more likely to have scleroderma if someone else in your immediate family has it, too.
It is believed that factors like environmental toxins and/or viral infections can trigger scleroderma symptoms to flare up. The overproduction of collagen is due to abnormal functioning of the immune system.
Because women develop scleroderma more often than men do, it may be that there is a hormonal factor that affects the disease, as well.
Diagnosis and Medical Treatment for Scleroderma
There is no cure for scleroderma, so conventional medical treatments aim to alleviate symptoms and slow down the progression of the disease. The treatment plan may vary depending on the specific manifestations and severity of the disease.
To diagnose scleroderma, doctors rely on a combination of clinical assessments, medical history review, physical examinations, and lab tests. A doctor will first observe skin changes, such as thickening and hardening, then look for internal organ involvement and other symptoms.
Blood tests can help identify specific antibodies associated with scleroderma, such as antinuclear antibodies (ANA), anti-centromere antibodies (ACA), and anti-Scl-70 (anti-topoisomerase I) antibodies. Additionally, blood tests can assess organ function, including kidney and liver function, as well as inflammatory markers.
X-rays, ultrasound, or CT scans may be used to evaluate internal organ involvement, such as lung fibrosis, gastrointestinal complications, and cardiac abnormalities.
A skin biopsy sample may be taken to confirm the presence of fibrosis and assess the degree of inflammation.

Medications that may be recommended for treating scleroderma symptoms include:
- Immunosuppressants: Medications such as methotrexate, mycophenolate mofetil, and azathioprine may be prescribed to suppress the immune response and reduce inflammation.
- Corticosteroids: Oral or topical corticosteroids can help manage inflammation and alleviate symptoms in certain cases. However, long-term use may have potential side effects and is usually minimized.
- Vasodilators: Medications like calcium channel blockers and prostacyclin analogs may be prescribed to improve blood flow and manage Raynaud’s phenomenon.
- Proton pump inhibitors (PPIs): These medications can help manage gastroesophageal reflux disease (GERD) symptoms, which are common in scleroderma patients.
Patients are often advised to make lifestyle changes to manage their condition effectively. These may include:using skin moisturizers and avoiding excessive sun exposure, and using sunscreen with a high SPF, avoiding cold temperatures and stress to prevent triggering Raynaud’s, quitting smoking, and eating an anti-inflammatory diet.
Can Acupuncture Help Scleroderma?
TCM treatment for scleroderma focuses more on addressing the underlying causes of the condition, rather than simply trying to relieve symptoms. An acupuncturist will look closely at the whole person, listen carefully to hear all the symptoms they are experiencing, even those which may seem unrelated, feel their pulse and make other observations, and then ascertain which diagnostic pattern may apply.
According to TCM theory, scleroderma symptoms may occur due to:
- Blood stagnation
- Yang deficiency
- Kidney Qi deficiency or yang deficiency
- Liver and Gallbladder damp heat
- Liver blood deficiency
- Liver win
- Spleen yang deficiency
- Stagnation of cold, wind, and/or damp
Depending on the diagnosis, the TCM practitioner will then plan a treatment protocol to address the root cause, using acupuncture and herbs. For example, herbs can help move stagnant blood, relieving the skin conditions related to scleroderma. Herbs can even help to inhibit collagen production, to help reduce skin hardening.
Acupuncture has been shown to help reduce the number of Raynaud’s attacks.
Moxibustion treatment may also be used to help relieve symptoms related to Raynaud’s phenomenon.
The use of acupuncture for stress relief is also integral to treatment for scleroderma, as stress can trigger a worsening of symptoms.
Acupuncture can help reduce esophageal reflux in cases where esophageal strictures have developed due to scleroderma in the digestive tract and help improve kidney function when kidneys have been impacted by fibrosis.
TCM herbal formulations for scleroderma will be individualized for each patient’s needs. Herbs may be used to help warm and nourish the organs, while clearing dampness and activating stagnant blood and Qi.
Acupuncture Near Me for Scleroderma in Los Angeles
Acupuncture and TCM herbal medicine can be excellent modalities for helping with difficult to treat skin conditions, connective tissue disorders, and autoimmune disorders, including:
- Dermatitis
- Eczema
- Psoriasis
- Vitiligo
- Rheumatoid Arthritis
- Lupus
- Herpes simplex
- Hives, urticaria
- Ehlers-Danlos syndrome (EDS)
If you are experiencing painful skin problems or digestive problems, consider seeking out alternative care in addition to conventional treatments.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Hay Fever With Acupuncture and TCM
By Qineng Tan, L.Ac. Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

Itchy eyes, runny nose and sneezing? These are some of the classic seasonal allergy symptoms, also known as allergic rhinitis, or hay fever. Acupuncture and TCM herbs can help relieve allergies, including pollen allergy symptoms.
Seasonal allergies affect about 20% of Americans. Allergic rhinitis is an immune system reaction to an allergen in the air that can be inhaled, like pollen from budding trees, growing grass, and plants like ragweed. Hay fever is a common term that typically describes being allergic to pollen.
“Pollen” are tiny seeds from plants that can be carried by the wind. When there is lots of pollen in the air, this is called a high pollen count. You can check the pollen count, like a weather report, to see when it is particularly high, and thus may affect people who suffer from seasonal allergies and asthma.
While having an allergic reaction to common airborne allergens happens most often during the spring, summer, and early fall, when plants are giving off a lot of pollen, people can actually experience hay fever at any time of the year.
Similar allergy symptoms can occur due to exposure to dust mites, molds, and pet dander.
Acupuncture and TCM can help relieve the irritating symptoms caused by allergic reactions by helping to strengthen and balance the immune system so that it is not so easily triggered.
Top 10 Seasonal Allergy Symptoms

The body’s histamine response causes inflammation of the mucus membranes in the sinuses and throat. The increased mucus production occurs in order to drive out the offending allergens.
Pollen allergy symptoms are similar to those of the common cold. Signs of hay fever include:
- Sneezing
- Nasal congestion
- Runny nose, itchy nose
- Itchy eyes, watery eyes (allergic conjunctivitis)
- Itchy throat
- Postnasal drip
- Headaches, sinus pain
- Dark circles under eyes, puffy eyes, “allergic shiners”
- Fatigue, malaise, generally feeling under the weather
- Wheezing, coughing, trouble breathing
Skin rash is a less common symptom of seasonal allergies, but some people do develop a hay fever rash. The itchy allergy rash may look similar to hives: raised red welts on the skin.
Treatment for Hay Fever
The common medical treatment for hay fever is an antihistamine. Histamines are chemicals that occur naturally in the body as part of the immune response to allergens in the environment. The release of histamines is what leads to allergy symptoms like a runny nose and itchy eyes.
Antihistamines come in pill or spray form, and they block the histamine response, which can temporarily relieve the hay fever symptoms. However, these medications do have side effects, the most common of which is drowsiness.
If someone is not getting relief from antihistamines, then corticosteroids, or steroids, may be prescribed. These work as anti-inflammatories, which in this case means that they reduce the swelling of mucous membranes. Steroids, too, can have significant side effects, especially when used over a long period of time.
Nasal sprays for allergies, like Flonase or Mucinex, are decongestants that are designed to be sprayed into the nose to help reduce allergy runny nose. Again, these may provide some temporary relief, but people can quickly get used to them, so they stop being effective.
Acupuncture and TCM offer an alternative treatment for allergies that can help relieve hay fever symptoms without side effects.
Can Acupuncture Help Hay Fever?

According to TCM theory, allergies fall under the category of illnesses that are caused by “wind” as a pathogenic force that can invade the body. In the TCM view, hay fever occurs due to wind-heat getting into the lungs.
Weakness of the kidneys and spleen can also contribute to hay fever; when they are sluggish, mucus tends to build up, and we become more easily fatigued.
When the defensive Qi is strong, it can protect us from cold, heat, wind, and dampness getting into the body and causing problems. Defensive Qi is roughly analogous to what we think of as the immune system in conventional medicine.
TCM treatment for allergic rhinitis may include acupuncture, herbal supplements, moxibustion, and nutrition counseling. TCM can be used either as an alternative therapy for allergies, or as an adjunct treatment for hay fever, along with pharmacological treatment.
Chinese herbs have been used for many centuries to treat allergy symptoms. Now, we are able to see scientific evidence that these herbs, such as astragalus, magnolia flower, and licorice root, do actually have an effect on the immune response and histamine function by helping to regulate the production of chemicals like cytotoxic T-cells and immunoglobulin G. Compounds found in scutellaria root have been found to inhibit the production of inflammatory cytokines, and stephania root can help prevent anaphylaxis.
With Chinese herbal medicine, we are able to create customized formulas for each patient, depending on their particular presentation of symptoms.
Acupuncture is a highly effective modality for all types of allergies, from allergic rhinitis to atopic dermatitis or eczema, and can help relieve the nasal sinus symptoms that affect the eyes, nose and mouth if someone is allergic to pollen. It can also help reduce itching due to allergic skin rashes.
A clinical trial conducted at a hospital in China showed that a regimen of acupuncture and herbs resulted in over 90% of patients reporting that their nasal symptoms were greatly reduced.
Another published study showed that acupuncture reduced levels of Immunoglobulin-E, an antibody that is associated with allergy responses.
A review of studies of acupuncture for allergic rhinitis showed that this treatment has both short-term and long-term efficacy.
TCM treatment for seasonal allergies allows us to get to the root cause of allergy symptoms and help prevent them from happening. In this way, acupuncture and herbs can function as preventive medicine for hay fever. Getting acupuncture periodically throughout the year can help you avoid allergy attacks when the pollen count is high.
Top 3 Tips for Hay Fever Prevention
Here are some things you can do to help prevent spring hay fever and relieve pollen allergy symptoms:
- Avoid dairy food and cold foods, which promote more mucus production.
- Apply warm compresses to the face to soothe the eyes and nasal area.
- Use an air purifier in your home to keep allergens out of the environment.
To relieve allergies, emphasize more cooked foods that help warm the body.
Acupuncture Near Me for Hay Fever in Los Angeles Area, Santa Monica
The multifaceted approach of TCM makes it uniquely suited to help relieve seasonal allergy symptoms. Acupuncture can help reduce hay fever symptoms right away and help prevent allergies from knocking you down every time the pollen count is high. Please do not hesitate to seek relief from hay fever by giving acupuncture and herbs a try.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Diarrhea With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

Chronic diarrhea, explosive diarrhea, diarrhea after eating? Diarrhea may be related to IBS (irritable bowel syndrome), or an IBD (inflammatory bowel disease), or a reaction to a food allergy, parasites, or stress. Acupuncture and TCM offer an alternative diarrhea treatment, so you can get relief from stomach pain and diarrhea.
Why Do I Have Diarrhea?
There can be many different causes of diarrhea, also known as loose stool. Acute diarrhea, which only lasts one or two days, will usually go away on its own.
Watery diarrhea that lasts a few days is usually due to food poisoning. Eating something that was rotten, or not cooked properly to destroy bacteria, can cause vomiting and diarrhea. Watery diarrhea can also happen when you have some type of viral infection, such as the “stomach flu.”
Chronic diarrhea, or persistent diarrhea, which lasts for weeks, or bouts of diarrhea that come and go frequently, may be related to IBS symptoms, IBD symptoms, Celiac disease, SIBO, or some other problem.
More than 6% of adults in the U.S. report having chronic diarrhea. Chronic diarrhea in children is also a serious health concern worldwide.
Top 10 Causes of Diarrhea
Diarrhea is a common condition that everyone experiences sometimes. Usually it is temporary, but it can become persistent and serious enough to require diarrhea treatment. The most common reasons a person experiences loose bowel movements include:
- Bacterial infection, traveler’s diarrhea, food poisoning, unsafe drinking water
- Viral infection, such as rotavirus, viral gastroenteritis, stomach flu
- Parasite infection, such as giardiasis
- Food allergy, food intolerance, food sensitivity, Celiac disease
- Reaction to medications like antibiotics, antidepressants, or Metformin
- Reaction to radiation therapy, cancer treatment
- IBS – diarrhea, constipation, and stomach cramps are common IBS symptoms
- IBD – colitis or Crohn’s disease, inflammatory autoimmune disorders that affect the gut
- Malabsorption of food, poor absorption of nutrients
- Menstrual cycle or Perimenopause – changes in hormones/estrogen can cause diarrhea
Certain foods can cause diarrhea, including: too much coffee, artificial sweeteners like mannitol and sorbitol, and red food coloring. Magnesium supplements can also cause loose stools.
If diarrhea lasts more than a few days, it is important to seek healthcare advice. Chronic diarrhea can lead to dehydration and fatigue, and may be happening because of some more serious condition that needs to be addressed.
What Causes Chronic Diarrhea?

Bouts of diarrhea that keep recurring can be a symptom of disorders such as:
- IBD (inflammatory bowel disease) – the most common IBDs are ulcerative colitis and Crohn’s disease. IBD symptoms usually include bloody diarrhea and abdominal pain. IBDs can cause chronic or recurring diarrhea, which can lead to dehydration, fatigue, and weight loss. IBDs can be mild, or so serious that they cause long-lasting damage to the gastrointestinal tract.
- Ulcerative colitis – an autoimmune disorder that causes inflammation and ulcers, or open sores, in the lower gastrointestinal system, including the colon and rectum.
- Crohn’s disease – an autoimmune disorder that causes inflammation mainly in the small intestine, but can affect any part of the GI tract.
- IBS – Irritable bowel syndrome can seem similar to IBDs, also causing recurring bouts of diarrhea and stomach pain. However, IBS is considered a functional gastrointestinal disorder. It is quite common. People with IBS symptoms may have alternating bouts of diarrhea and constipation. People who tend to have more diarrhea-dominant IBS have “IBS-D.”
- Celiac disease – an autoimmune disorder in which a reaction to eating wheat gluten causes serious inflammation of the GI system, leading to abdominal pain, bloated stomach, diarrhea, malnutrition, fatigue, and skin rashes.
With these conditions, diarrhea is brought on periodically—sometimes alternating with constipation, as in some cases of IBS—by factors having to do with the diet or stress, or with autoimmune processes.
Some surgeries that affect the gastrointestinal organs—like gastric bypass, gastric sleeve, or gallbladder removal—can cause chronic diarrhea.
Chronic diarrhea can be caused by an inability of the intestinal walls to absorb nutrients, and/or of the walls of the colon to absorb liquid. It may also be due to excessive action of the intestine in terms of peristalsis, the squeezing of the intestine to move matter through.
Diarrhea Treatment
Acute diarrhea usually goes away on its own in a day or two. Often, people will use OTC remedies for diarrhea and stomach pain, such as Immodium or Pepto-Bismol.
If you have been experiencing persistent diarrhea and seek medical advice, a doctor will perform tests to figure out what is causing the diarrhea, and will offer electrolyte fluids to help with dehydration. Blood tests or a stool test will show if the diarrhea is due to a bacterial infection or parasitic infection.
If chronic diarrhea is determined to be related to a medication you are already taking, then that may need to be adjusted.
Discovery of IBS or an IBD usually involves more diagnostic testing, including a colonoscopy and/or endoscopy, to see if there is inflammation or blockage in the GI tract.
Medical treatment for IBS may involve being offered antispasmodic medications that relax the intestinal walls and slow down the movement of the bowels and can help relieve stomach cramps and abdominal cramping. Dietary changes and behavioral therapy may be recommended.
Pharmacological treatment for IBDs like colitis and Crohn’s usually involves taking a combination of anti-inflammatories and immunosuppressants, to reduce inflammation in the gut and to block the inappropriate autoimmune responses that are triggering the inflammation. Unfortunately, steroids and medications like Xeljanz can cause other side effects and health problems.
Medical treatment for chronic diarrhea may help relieve symptoms and reduce the frequency of bouts of diarrhea, but it does not necessarily address the underlying causes of diarrhea.
Acupuncture and TCM offer an effective alternative treatment for diarrhea that is more suited to each patient’s individual situation.
Can Acupuncture Help Diarrhea?
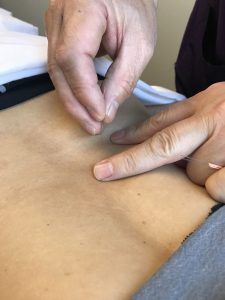
Chronic diarrhea, according to TCM theory, is usually considered to be related to the health of the spleen. In TCM, the organ systems all interact harmoniously, unless there is imbalance. The imbalance of one organ system may throw off other systems, leading to various symptoms.
In TCM, the spleen is responsible for breaking down the nutrients from food and converting them into energy. If the spleen is not functioning properly, watery stool is often the result. Diarrhea, stomach pain, and other symptoms may differ from person to person, depending on how the spleen is interacting with the liver, stomach, or kidneys.
Common Chinese Medicine diagnosis patterns for chronic diarrhea include:
- Spleen Deficiency with Liver Qi stagnation: mucus in the stool, abdominal pain, cramping, gassiness, bloated stomach, irritability, and feelings of depression
- Spleen Deficiency with Stomach deficiency: watery stools, poor appetite, feeling full quickly, stomach distended after eating, pallor, and fatigue
- Spleen Deficiency with Kidney Deficiency: diarrhea in the morning, partially digested food in the stool, abdominal pain, lower back pain, knee pain, feeling cold
Acupuncture treatment for diarrhea, which may include moxibustion and herbs, aims to support the health of the spleen and other organs. Acupuncture has been shown to help relieve diarrhea and constipation related to IBS. Acupuncture treatment can also help with reducing stress and anxiety, which are common triggers for IBS symptoms.
Acupuncture can also help with diarrhea due to IBDs like ulcerative colitis and Crohn’s disease by reducing inflammation and helping to balance immune responses. TCM treatment for Crohn’s disease or colitis, incorporating nutrition and herbal supplements, can help improve the gut biome and strengthen the lining of the intestinal walls.
Acupuncture for Diarrhea Near Me, Los Angeles, West L.A., and Santa Monica
TCM treatment with an experienced acupuncturist near me can be very beneficial for anyone dealing with ongoing gastrointestinal distress. Both adults and children can find relief from diarrhea, constipation, stomach cramps, bloating, and abdominal pain related to conditions like IBS, IBDs, or celiac disease through acupuncture and herbs. At Art of Wellness, we have over 30 years of experience helping people with gastric disorders of all kinds.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Colitis With Acupuncture and TCM
By Xiaomei Cai, L.Ac., Ph.D. & Qineng Tan, L.Ac., Ph.D.

Diarrhea, bloody stool, fatigue, fever? These could be colitis symptoms. Ulcerative colitis is an inflammatory bowel disease (IBD) that causes swelling in the large intestine, abdominal pain, bloating and bloody diarrhea. Acupuncture and TCM can offer an alternative colitis treatment to help relieve ulcerative colitis symptoms.
Colitis is a gastrointestinal disease in which the colon—also known as the bowel, or the large intestine—becomes inflamed and can develop open sores, or ulcers.
Ulcerative colitis is the term for colitis that is caused by an autoimmune disorder. The immune system launches an attack on the tissues of the intestinal lining, causing inflammation and sores. It is similar to Crohn’s disease: an autoimmune disease that can affect any part of the digestive tract.
What causes colitis? There are several problems that can lead to abdominal pain and diarrhea, and sometimes it can be difficult to discover what is causing a person to have colitis symptoms.
Parasites, bacterial infections, or food poisoning can cause pain, inflammation in the colon, and diarrhea. For example, e coli bacteria, sometimes found in improperly cooked beef, can cause colitis symptoms. This is known as e colitis, or hemorrhagic colitis.
IBS (irritable bowel syndrome) symptoms can seem similar to those of colitis. People who suffer from IBS can have abdominal pain and diarrhea, urgency and mucus in their stool. However, IBS is considered a functional gastrointestinal disorder, not a disease. IBS does not cause permanent damage to the intestinal lining, while colitis can.
Ischemic colitis is a specific type of colitis caused by a blockage of blood flow to the intestine. This is more common in older adults, and can be the result of a blood clot in an artery, or low blood pressure due to heart failure or recovery from some major surgery. Some conditions, like lupus or sickle cell anemia, can restrict blood flow to the gastrointestinal tract. It could also happen due to a bowel obstruction caused by a tumor or hernia. Some medications can also restrict blood flow to the intestine.
TCM and acupuncture treatment, whether alone or as an adjunct to conventional treatment, can help relieve the symptoms of colitis by reducing inflammation in the intestine, helping to stop bleeding and helping to restore normal bowel movements.
Colitis Symptoms

Ulcerative colitis symptoms can be mild at first and become more persistent and/or severe over time. Some common symptoms of colitis, or IBD symptoms, include:
- Loose stool, loose bowel movements, diarrhea
- Urgency to go to the bathroom, feeling like you have to poop all the time
- Feeling like you have to poop, but not being able to
- Bloody stool, bloody poop
- Mucus in stool
- Abdominal pain
- Abdominal cramps, cramping
- Rectal pain
- Fatigue, feeling tired all the time, no energy
- Fever
- Weight loss
Symptoms of ulcerative colitis can come and go, or “flare up” at times. When symptoms abate, this is called “remission.”
Children can have colitis, which may cause them to not grow properly.
Colitis Treatment
Testing for IBDs might start with some basic blood tests and a stool sample test to see if there are any bacterial or parasitic causes of diarrhea. If inflammation needs to be looked at more closely to discover its location and cause, a colonoscopy or sigmoidoscopy may be done. Imaging—X-ray, ultrasound, or MRI—may be used to show if there is some kind of obstruction of the intestine.
If testing and treatment have ruled out IBD and other potential causes, a tissue biopsy may be used to diagnose ulcerative colitis, the autoimmune form of colitis.
Generally, once colitis or inflammatory bowel disease has been diagnosed, the main goal is to reduce inflammation in the colon. Anti-inflammatory drugs will usually be prescribed. Anti-diarrheal medications and pain relievers provide some symptomatic relief.
Ulcerative colitis is usually treated with a combination of anti-inflammatories and immunosuppressants. Unfortunately, these types of medications can have significant side effects. Long term use of corticosteroids can cause bone loss and swelling, while immunosuppressants can stress the liver and pancreas.
Newer pharmacological treatments include “small molecules,” like Xeljanz, which act as anti-inflammatories and immunosuppressants. However, these drugs have been flagged for potentially causing heart problems, and maybe even cancer.
When medications and dietary changes don’t help enough, surgery to remove part of the large intestine may be sought.
Acupuncture and TCM offer an alternative treatment for colitis, which may help relieve symptoms without side effects.
Can Acupuncture Help Colitis?
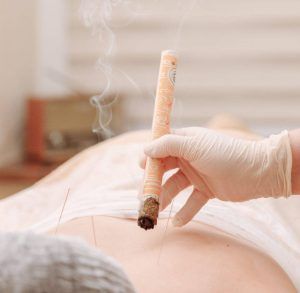
TCM herbs and acupuncture treatment are excellent modalities for helping to reduce inflammation. In the case of colitis and ulcerative colitis, the central problem is that the body is producing an inflammatory response in the large intestine that leads to pain and dysfunction. According to TCM theory, imbalances in the internal organs can cause heat, dampness, or blood stasis. In different people, the ways that colitis shows up may vary, depending on the pathogenic forces at work.
Acupuncture points to help relieve diarrhea, bloating, and bleeding in the colon will be combined with beneficial herbs to help clear heat and dampness. One study done in China showed that patients with ulcerative colitis who received acupuncture and herbal supplements in addition to conventional pharmaceutical treatments healed more quickly than those who did not receive TCM. They also reported feeling less anxiety and depression.
A systematic review of studies done regarding TCM for colitis concluded that acupuncture and herbs were effective compared to medical treatments.
Studies have shown that acupuncture can help balance the gut biome and help strengthen the intestinal walls.
Acupuncture has been shown to help people whose colitis is in remission to maintain better function.
TCM herbs, used in combination with conventional treatment, may help improve the healing of the mucosal lining of the intestine. One study showed that herbs helped stop bleeding from the colon in patients with ulcerative colitis.
Moxibustion has also been shown to help as a treatment for IBD, helping to relieve diarrhea, nausea, and abdominal cramping.
Acupuncture is believed, in part, to help regulate inflammatory bowel diseases by providing positive stimulation of the vagus nerve, which plays an important role in inflammatory responses.
Acupuncture Near Me for Ulcerative Colitis in Los Angeles and Santa Monica
Acupuncture can be an excellent adjunct to standard treatment for gastrointestinal disorders of all kinds, including: IBS, Crohn’s disease, Celiac disease, and Candida. At Art of Wellness, we have over 30 years of experience helping people with IBD and colitis to improve their quality of life.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.