-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

March 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31
Pain
How to Treat Hemorrhoids With Acupuncture and TCM
By Xiaomei Cai, L.Ac., Ph.D. & Qineng Tan, L.Ac., Ph.D.

Bleeding and discomfort when you go to the bathroom? Burning or itching around the anus? Hemorrhoid pain is caused by swollen blood vessels around the rectum. Acupuncture and TCM reduce inflammation and can bring swift hemorrhoid relief.
Sometimes called “piles,” (from the Latin “pila,” meaning “balls”), hemorrhoids often do resemble little balls or clusters of grapes. The word “hemorrhoid” actually refers to the specific formation of blood vessels and cushioning tissues that surround the anus. Colloquially, though, the term is usually used to describe the condition of inflammation and irritation that can occur in this area.
Hemorrhoids are very common; probably more than half the population experiences them at some point in their life. However, the discomfort of talking to a doctor about hemorrhoids can be almost as miserable as the physical discomfort of having them, so many people avoid getting hemorrhoid help.
How do you know if you have a hemorrhoid? Sometimes people have a lot of itching, burning and discomfort after a bowel movement, or throughout the day. Sometimes there is no pain, but you may see a little bit of blood in the toilet bowl, or when you wipe with toilet paper. When you touch the area, you may feel a lump, or swollen tissue.
Hemorrhoids are generally classified into two categories based on their location: internal hemorrhoid and external hemorrhoid. Internal hemorrhoids form inside the anus and lower rectum and can cause bleeding, usually without pain. In some cases, though, the swollen veins can protrude out from the anal sphincter during or after a bowel movement and then need to be pushed back in. This is called a “prolapsed internal hemorrhoid.” The situation can become more serious if the internal hemorrhoid can’t be pushed back in, or if a blood clot develops in the vessel (thrombosis); then, it becomes painful to go to the bathroom, or even sit. In some cases, a prolapsed hemorrhoid becomes “strangulated,” meaning the blood supply is cut off, which can cause severe pain. Hemorrhoids become prolapsed because the connective tissues in the area weaken due to intense pressure, usually due to straining during a bowel movement, or because of the extra weight of pregnancy or obesity.
External hemorrhoids develop outside the anus, under the skin. These are the kind of hemorrhoids that tend to cause itching and a little bit of bright red bleeding. Again, they are aggravating, but not too serious unless a blood clot forms; then, it is called a “thrombosed external hemorrhoid.” This type of hemorrhoid can turn blue or purple in color and become acutely painful. In some cases, surgery will be performed to drain blood from the clot, or remove the hemorrhoid.
Most of the time, people suffer quietly with hemorrhoids, waiting for them to go away on their own. Only when they cause severe pain and bleeding are medical treatments considered. However, TCM and acupuncture offer a way to deal with hemorrhoids so that they heal more quickly and reduce the chance to return.
Top 10 Hemorrhoid Causes

What causes hemorrhoids? The tissues and blood vessels around the anal area can become weak, irritated, and inflamed. The upright posture of our human bodies naturally puts pressure on the elimination organs. Many women get hemorrhoids during pregnancy and/or birth because of intense pressure on the perineal area.The major reasons for hemorrhoids include:
- Pregnancy
- Constipation
- Diarrhea
- Sedentary lifestyle
- Straining while on the toilet
- Sitting too long on the toilet without progress
- Lack of dietary fiber
- Obesity
- Family history of hemorrhoids
- Aging
Overall, focusing on eating a diet that includes plenty of fiber, drinking enough water, maintaining good bathroom habits (going when you feel the urge and not waiting) and a healthy weight will go a long way towards preventing hemorrhoids. But what can you do when you already have hemorrhoids?
Treatment for Hemorrhoids

Often, people will just deal with hemorrhoid itching and pain on their own by using over-the-counter products like creams that contain phenylephrine, which constricts blood vessels (Preparation H), or disposable wipes impregnated with witch hazel and other soothing ingredients (Tucks medicated pads). These treatments may help reduce pain and swelling temporarily, but they do not get rid of hemorrhoids at their root.
When people do talk to their doctor about hemorrhoids, they may be prescribed something stronger, like a steroid cream, or hydrocortisone rectal suppositories.
If the situation persists or becomes more severe, there are several types of outpatient procedure to treat hemorrhoids, including rubber band ligation, sclerotherapy, infrared photocoagulation, and electrocoagulation. All of these procedures cut off blood supply to the hemorrhoid, so that it will form scar tissue and fall off. Hemorrhoid stapling and hemorrhoidectomy are outpatient procedures in which the hemorrhoids are surgically removed, and/or prolapsed tissues are affixed back inside the anus. While these surgeries may be helpful in some cases, recovery can be painful, and there can be problems with the way things work afterwards, potentially leading to more surgery later on.
When hemorrhoids are severe, it is a good idea to consult your doctor, as there are more serious conditions that may produce similar symptoms of pain, itching, or bleeding, including anal fissure (torn tissue or open sore in the anus due to trauma or Crohn’s disease complications), anal abcess (infected cavity in the anus) or anal fistula (an opening from the anal or rectal area that drains pus and/or fecal matter). Sometimes skin tags develop around the area where a hemorrhoid has healed. These can be irritating and difficult to keep clean, so they may need to be surgically removed.
For the treatment of hemorrhoids, TCM methods can provide relief from symptoms and help to reduce the inflammation that caused them.
Can Acupuncture Help Hemorrhoids?
According to TCM philosophy, hemorrhoids can often be related to a build-up of heat and/or dampness in the lower abdominal area; it’s the heat and dampness that cause the blood vessels to swell. You might be concerned by the idea that acupuncture treatment for hemorrhoids would involve needles being placed in a highly sensitive, private area. Let us reassure you this is not the case. The Du Mai meridian, also known as the “Sea of Yang,” is the channel which runs from the rectum area up along the spine to the top of head and then down to the mouth, controlling Yang energy throughout the body. We use points along this meridian, on the top of the head, and in other parts of the body to draw excess heat and dampness away from the area where the hemorrhoids are.
Other presentations of hemorrhoids include:
Top 5 Types of Hemorrhoids Presentation in TCM
- Spleen Qi Deficiency – This is when people tend to have poor digestion, bloating, gas, and diarrhea, going to the bathroom very often; the hemorrhoids feel swollen, but not as red. We use moxibustion to work on stomach point 36 meridian point, CV points 6 and 4, and spleen 6 in the middle of the abdomen to help digestion.
- Spleen Qi Sinking- This presentation tends to happen to people who are thinner, not only having hemorrhoids, but all the organs tend to be lower than usual; may also have prolapsed bladder or uterus, and poor digestion. Moxibustion applied to the middle of the top of the head will head the Qi rise up. For both types, doing Kegel type exercises regularly can help to strengthen the rectal area, also the uterus and bladder. Do three sets, increasing a bit every time: for example squeeze 30 times, release, do again 35, rest, next 40, then rest. Do this exercise every morning and evening.
- Blood Stasis – This type is more and more common because of our modern lifestyle, due to sitting a lot for work, which causes blood circulation to be compromised. In Chinese, we have a proverb: “for 10 people who sit too long, 9 will have hemorrhoids.” These manifest more as red, swollen, maybe bleeding. Kegels will also be helpful here, too.
- Lower Jiao Fire/Heat – This is when the lower part of the body has too much fire. For this type of hemorrhoids, people tend to have more bleeding, especially triggered by having alcohol, spicy food, crunchy food. These are the kind that may feel very sore with a burning sensation and tend to bleed, especially when wiping.
- Intestinal Dryness – especially here in California, where we have hot, dry weather, without a good habit of drinking water, people can tend to constipation, even going only once or twice a week. These types of hemorrhoids are due to dry, uncomfortable bowel movements, and may have itching and bleeding. Adding more water (warm is better) and more moisturizing foods (sesame oil and lots of ripe bananas, flax seeds, chia, sweet potato/yam, prunes) will be helpful.
Kegel type exercise is helpful for all of these types, to strengthen the sphincter muscle and bring more circulation to the area. Add more movement overall. At bedtime, leg lifts, bicycle movements in the air, upside down, are a good way to exercise without putting pressure on the lower body.
Ideally, when there is good digestion, between 5:00 – 7:00 a.m. is when people should naturally want to go, quickly, without too much need to push. Sitting on the toilet for too long creates the pressure that leads to hemorrhoids.

Moxibustion treatment–the burning of the herb mugwort near an area–can be very effective for reducing pain quickly. Chinese herbal formulations, used both internally and externally, can help relieve inflammation and pain. An herbal tea formula may include herbs to help strengthen the energy of the spleen, and to lubricate the digestive tract.
We also recommend sitz baths as a home remedy for hemorrhoids: short, 15-minute baths in warm water, to help soothe the area and keep it clean. Your acupuncturist may give you an herbal bath sachet to use to help reduce inflammation and soother the tissues.
One study of acupuncture treatment for internal hemorrhoids showed that, after 24 days, 86% of patients were “cured,” while another 8% showed significant improvement.
Your acupuncture practitioner will also talk with you about changes you can make in your diet and bathroom habits that will help you get things moving more easily.
Acupuncture Near Me for Hemorrhoids
Hemorrhoids are not only irritating; they are a sign that you may need to pay more attention to what you’re eating, and that you need to give yourself a little more time for relaxation, in and out of the bathroom. A combination of acupuncture, herbs, and other TCM treatment for hemorrhoids can help get the pain and swelling behind you.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat TMJ With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.
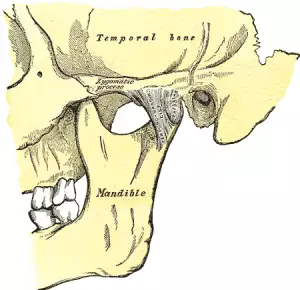
What is TMJ? “TMJ” is an acronym for “temporomandibular joint,” which is the double joint structure that attaches the lower jaw to the skull. “TMJ” is also used as a general term to refer to disorders of the jaw joint. Popping or clicking of the jaw joints, tension or pain in the jaw, grinding teeth, headaches, neck pain, and shoulder pain can all be signs of a TMJ disorder, or TMD. Acupuncture and TCM offer relief from TMJ jaw pain and inflammation.
The jaw joint is totally unique among joints in the human body in a few ways. It is really two joints that must always work together; you cannot choose to just move one side of your jaw. Also, the temporomandibular joint has two ways in which it moves; it “hinges,” and then, it “slides.”
Hinge joints, like the knees and elbows, allow flexion and extension on one plane, while remaining stabilized by a complex group of muscles, ligaments, and other connective tissues. Most of these joints are made of bones that are “molded” to fit and move together. Gliding joints, also called plane joints, like those in the ankles, wrists, and vertebrae, have flat sides that slide alongside each other when they move. The jaw joint combines both of these actions. Essentially the movement of the jaw is a kind of dislocation by design. Small discs of cartilage help to cushion the areas where the jawbone interacts with the sides of the skull in front of the ears.
It can be difficult to determine the exact causes of “TMD,” or temporomandibular disorders that cause pain and dysfunction. Injury to the jaw, dislocation of the jaw, inflammation of tissues, arthritis, and bruxism (clenching or grinding the teeth and jaw) can all potentially lead to jaw pain or clicking in the jaw. Erosion or damage to the cartilage sometimes causes TMD, impacting the usually smooth motion of the opening and closing of the jaw. Structural issues like missing teeth or an uneven bite can cause jaw problems. Dental and orthodontic work that requires the patient to hold the mouth open for long periods of time can sometimes lead to TMJ pain. Habitual movements like teeth grinding, biting on things like pencils, nail biting, or leaning your chin on your hand can also contribute to TMJ pain. Chronic pain syndromes like fibromyalgia can also cause jaw pain.
Most cases of TMJ disorders resolve themselves over time, usually within a few to several months. Resting the jaw and eating soft foods is usually recommended. Medical treatment usually involves medications to reduce inflammation and relieve pain while waiting for the jaw joint to gradually regain its normal function. Only in rare cases is surgery necessary to get rid of jaw pain.
TMJ, or myofascial pain in the muscles around the jaws, is experienced by a third or more of all adults at some point in their lives. TCM modalities like acupuncture can help alleviate the pain and impeded mobility of the jaw joint caused by TMJ disorders.
Top 10 Symptoms of TMJ

Pain around the jaw joints that comes and goes is the most common complaint of people with TMJ disorders. However, problems with the jaw can contribute to pain and tension in other parts of the head and shoulders, too. The most common signs of TMJ include:
- Pain in cheeks, tension in the jaw
- Jaw clicking, popping of jaw bones
- Limited movement of jaw, can’t open jaw normally
- Clenching of jaw, grinding teeth at night
- Tooth pain, pain in the back teeth
- Ear pain, ringing in the ears, tinnitus
- Headaches, migraines, pain behind eye, sensitive to light
- Stiffness in shoulders or neck, pain in neck, shoulder pain
- Numbness or tingling in arms, hands, or fingers
- Dizziness, vertigo
The combination of hard bony structures, muscles, and cartilage that are all involved in TMD causes TMJ pain that is hard to pinpoint because it may move around, and come and go. Most people describe the sensation as a dull ache. Some people don’t experience pain, but still have trouble with jaw clicking or opening and closing the jaw.
What Is the Treatment for TMJ?

A doctor or dentist may check for signs of TMJ by observing and manually examining the movement of the jaw joint. Dental X-rays may be used to help determine the cause of jaw pain. CT scan or MRI may be recommended to get a more detailed look at the bones and cartilage.
The primary recommendations for jaw pain and clicking is to rest the jaw as much as possible and eat only soft foods. Physical therapy (PT) can help strengthen the muscles of the face and encourage people to change habitual behaviors that might be contributing to TMJ. Wearing a splint or bite plate keeps the mouth and jaw in place and prevents grinding teeth in the night. This combination of PT and splinting is called stomatognathic treatment. If pain is serious enough to require further medical treatment, doctors will usually prescribe either pain relievers, anti-inflammatories, muscle relaxants, or some combination of these. Surgery is only used in rare cases when the jaw has become “locked,” or TMJ inflammation and pain has become chronic.
Acupuncture and TCM treatment offer a way to reduce inflammation and pain related to TMJ disorders without risky surgical procedures or the adverse side effects sometimes caused by corticosteroids and other medications.
Acupuncture Treatment for TMJ
Acupuncture can work to reduce inflammation and pain from many different conditions, including musculoskeletal disorders like TMD. Acupuncture is effective at reducing sensations of pain, both by reducing inflammation in areas from which the pain is originating and by stimulating the release of endorphins and other neurotransmitters that help boost feelings of well-being. Acupuncture treatment can also help the muscles involved with jaw function to relax, alleviating the “clicking” or “popping” associated with TMJ disorders.
In TCM theory, TMJ is often related to what we call different types of “obstruction” syndrome. Stress and trauma, both physical and emotional, can cause Qi stagnation and/or blood stagnation. Pathogenic forces like cold, heat, wind, and damp can cause painful obstruction, or blockages of energy and blood in certain areas of the body. People suffering from TMJ do not necessarily only have dental pain or myofascial pain, a clicking jaw, or limited movement. They may also be experiencing a variety of other symptoms that are actually related. A TCM practitioner will look at the whole picture of what each patient is feeling, and treat accordingly.

For example, a person with Liver Qi stagnation may have:
- tension in the facial muscles
- neck pain
- feelings of anger or anxiety,
- ringing in the ear, tinnitus
- headaches
A person with a Wind/Cold Bi Syndrome presentation might feel:
- acute onset of pain
- pain moves around from one area to another
- aversion to wind and cold
- fever, chills
- ear ache, ringing in the ears
As a holistic form of medicine, TCM works not only to relieve jaw pain and swelling, but to get to the root of the problem.
A comparative study designed to evaluate TCM treatment for TMJ found that patients who received acupuncture treatment reported less pain and muscle tenderness than those that did not.
A clinical study that compared groups of patients who received acupuncture treatment for TMJ pain and limited motion to patients treated with decompression splints. Both groups experienced reduction in pain and increased mobility, and the researchers concluded that acupuncture can be considered beneficial as either an adjunct or alternative treatment.
In some cases, a stiff, painful jaw joint can be a secondary symptom of another, more systemic problem like rheumatoid arthritis or fibromyalgia. These conditions can also be addressed with acupuncture.
Acupuncture Near Me for TMJ Disorders
TMJ disorders interfere with a person’s most basic activity: eating. While most cases of TMD improve within a matter of months with the proper rest, they can cause a lot of pain and frustration while a person is waiting to heal. Acupuncture and TCM herbs can help relieve TMJ pain and restore normal jaw function, helping people get back to normal more quickly than rest alone. At Art of Wellness, we have over 30 years of experience helping patients with musculoskeletal disorders and pain of all kinds find relief and a return to their usual mobility.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Lyme Disease With Acupuncture and TCM
By Xiaomei Cai, L.Ac., Ph.D. & Qineng Tan, L.Ac., Ph.D.

Red, circular rash that looks like a “bulls-eye?” Joint pain, muscle aches, and fatigue? These are signs that a person may have Lyme disease, an infectious disease that humans can contract when they are bitten by an infected tick. Lyme, a bacterial infection, can take a while to develop, and can cause chronic symptoms if it is not treated effectively. Acupuncture and TCM offer an alternative or adjunct way to help resolve the painful, debilitating symptoms of long-term Lyme disease.
Lyme disease is a type of bacterial infection transmitted by ticks. Ticks are parasitic arachnids, small spider-like creatures who bite other animals and feed on blood. If a tick is infected with a disease, it can infect the person or other animal it bites. Lyme disease, which is caused by the Borrelia burgdorferi bacterium, is just one of several infectious diseases that ticks can spread, including Rocky Mountain Spotted Fever (RMSF).
These critters are sometimes called “deer ticks” or “bear ticks” because they generally thrive in forest environments where they live symbiotically with these kinds of animals. But being bit by deer tick (tick on deer) doesn’t only happen in deeply wooded areas; anywhere that deer, squirrels, lizards, or birds may come into suburban areas, it is possible to be bitten by a tick. Actually, ticks, and therefore the infectious diseases they carry, are growing more prevalent because of humans encroaching into animals’ habitats. Tick bites most commonly occur in spring and summer.
Ticks do not fly; they can only get onto dogs or humans by crawling on them. This can happen quite easily if a tick is on a bush or other plant, and a person or dog brushes up against it. Ticks attach themselves to a host, and slowly suck their blood.
Lyme disease in dogs cannot be transmitted to humans, nor is lyme disease contagious, passing from human to human; you can only get Lyme disease by being bitten yourself. In order to pass Lyme disease to a person, a tick generally has to have been attached to that person’s skin for 36 hours or more. Ticks can be as small as the head of a pin, and they burrow in moist, hairy areas of their host’s body, so it is actually quite easy to have a tick on you without knowing it. After the tick drops off, a person may not feel anything at all, or only have a small, red bump that resembles a mild insect bite. In some cases, though, a person may feel right away that the area of the bite is hot, swollen, or causing a burning sensation.
If the tick was carrying Lyme disease, it can take several days to a few weeks for the more serious symptoms of Lyme to develop. Even then, the symptoms are not necessarily distinctive.
The early symptoms of Lyme disease can feel like a flu; fever, fatigue, aches and pains. Not everyone infected with Lyme will have the characteristic tick bullseye rash that develops around the site of the tick bite. When treated promptly with antibiotics, most cases of Lyme disease will resolve within a few weeks. However, many cases of Lyme disease are not diagnosed right away, and if it goes undetected, chronic problems can develop in the ensuing months. Once the bacteria has spread throughout the body, even a long course of antibiotics may not be able to get rid of it. Long-term Lyme symptoms may appear similar to other chronic inflammatory, autoimmune, or neurological conditions, such as fibromyalgia, Bell’s palsy, MS, chronic fatigue syndrome, or PTSD.
In extreme cases Lyme disease causes shoulder pain, hip pain, knee pain, fatigue, and other symptoms so severe that people can’t go about their regular daily routine. Sometimes diagnosis and treatment is further complicated by coinfections: concurrent other infections, that can also have been transmitted via the tick bite, or occur independently of it. Lyme and other tick-borne illnesses like RMSF can also trigger sepsis infections, which can be life-threatening, or lead to chronic pain, and/or PTSD (post-traumatic stress disorder). An MRSA skin infection (Methicillin-resistant Staphylococcus aureus), a type of staph infection that enters the skin through a wound, can develop around the infected tick bite; this staph skin infection is particularly resistant to antibiotics.
Unfortunately, symptoms of Lyme can become progressively worse over time, leading to disability and even death. Acupuncture and TCM offer an alternative for helping to heal Lyme disease, whether it is still in the early stages, or when it has become a chronic infectious disease.
Top 10 Symptoms of Lyme Disease

Signs of Lyme disease develop slowly, in stages, and can vary widely from person to person. Without the presence of the tell-tale bulls’ eye rash, both patients and doctors may have difficulty linking the spectrum of symptoms to a Lyme infection.
- Joint pain, swollen joins, arthritis
- Neuropathy, numbness or tingling, Bell’s palsy (face drooping)
- Fatigue
- Bulls-eye rash, also known as erythema migrans rash
- Headaches, migraines
- Sleep problems, sleep apnea, snoring
- Brain fog
- Trouble breathing
- Vertigo, dizziness
- Blurred vision
Other possible symptoms of Lyme include: ringing in the ears (tinnitus), heart palpitations, problems with memory and concentration, vision problems or inflammation around the eyes, and liver problems, like hepatitis. Symptoms of lyme disease in dogs are similar to those in humans, including stiff, swollen joints, tiredness, and loss of appetite.
Long-term effects of Lyme disease are sometimes referred to as “post-treatment Lyme disease syndrome.” Doctors are not sure why some people, even after being treated with antibiotics, seem to still be affected by long-term effects of Lyme disease.
Medical Diagnosis and Treatment of Lyme Disease
Getting a clear diagnosis of Lyme disease can be difficult. Currently, there is a two-step diagnostic process recommended to determine if a person has contracted Lyme disease. Two main kinds of tests can detect antibodies the body’s immune system creates to fight off the infection. However, it takes a while–at least several weeks, usually–for the body to build up enough of the antibodies that they become detectable. Often when people are aware early on that they may have been infected, and they get a test, it turns out to be negative. Usually, doctors try first one type of antibody test, and then the other to see if they get a positive result. Even then, medical science acknowledges that many (perhaps half of) Lyme disease cases are not detected this way.
A newer, still somewhat unproven form of testing involves taking a blood culture and trying to grow the bacteria that cause Lyme in a laboratory setting. This testing is more advanced and may be difficult for patients to access.
Once physicians have determined that Lyme infection is present, the usual treatment is a course of antibiotics that lasts a few to several weeks. In many cases, this seems to clear up the infection. In others, though, the antibiotics do not resolve the myriad symptoms patients are experiencing. Using antibiotics on a long-term basis is often not effective, and carries other risks to a person’s health.
Ongoing joint pain and inflammation is then usually treated with steroid medications or NSAIDS. Sleep problems and fatigue are often treated with antidepressants. These medications may help relieve symptoms temporarily, but they come with side effects, and do not address the root causes of the chronic symptoms of Lyme disease.
3 Stages of Lyme Disease
When early detection occurs, the Western medical approach of using antibiotics can often resolve Lyme disease within a few to several weeks. However, if the infectious disease is not found soon enough, Lyme disease will progress to more advanced stages. TCM methods can be helpful during all three stages of Lyme.
- First Stage Lyme disease – Within the first few weeks of the infection, and with early detection, antibiotics can be very helpful, working pretty well to stop the spread of the bacteria. However, because Lyme disease is often misdiagnosed, many people do not receive this treatment soon enough. During this phase, the symptoms are similar to those of the flu: chills, fatigue, heaviness in the limbs. As the infection moves in deeper, it can cause the skin rash, or hives. TCM treatment during the first stage will focus on clearing heat and detoxifying the body to rid it of infection.
- Second Stage Lyme disease – If the bacteria causing Lyme disease is not halted in its spread, it begins to affect the organs and the blood. The central nervous system and heart can become infected. These infections can last for months, and if not taken care of, can develop into the third phase. This is when a person may begin to feel joint aches, and arthritis-like symptoms. The body’s Qi and blood become deficient. Treatment with acupuncture and herbs at this point will work to help boost the Qi, clear heat and strengthen the whole immune system, and clear inflammation.
- Advanced stage Lyme disease – As the infection drags on, it can cause joint, skin, and nerve damage can take hold. Ongoing Qi and blood deficiency and stagnation cause fatigue, dizziness, insomnia, and memory loss.
A TCM provider will recognize what stage of Lyme disease a patient is in according to their symptoms, and customize the acupuncture points and herbal formulae used depending on their needs.
Acupuncture for Infectious Diseases

For millennia, TCM has recognized a type of disease that is caused by infection and can affect all systems of the body. We call this type of illness Gu zheng, or “Gu syndrome.” This classification covers illnesses caused by “invisible” pathogens, like viruses, funguses, and parasites. Along with the toxins from the tick bite, we consider how pathogens like heat, wind, and dampness all play a role in the illness. According to TCM theory, extreme heat in the body is also considered “toxic.” This category of condition helps us understand a variety of different systemic inflammatory illnesses, and gives us a framework for addressing each individual’s presenting symptoms.
One of the key features of Gu syndrome illnesses is how terrible and hopeless they can make people feel. Not only do people suffering from chronic inflammatory or immune-related conditions feel constantly tired and ache-y, but some of the sensations seem to come and go and feel so mysterious that they can’t be explained satisfactorily. If this is then compounded with the fact that many doctors don’t understand or know how to deal with the illness, it can leave patients feeling very frustrated and helpless. After months or years of this, debilitating physical symptoms may be accompanied by feelings of depression and anxiety.
A Yale Medical University study of patients, all in their 40s, suffering from long-term Lyme complications found that they had to reduce their activities, or even give up working, and doubted that they would ever recover. In interviews, patients made it clear that working with doctors who were more holistic was far preferred, and thus many had turned to CAM (complementary and alternative medicine) providers for help with Lyme disease.
Making a full recovery from long-term Lyme disease is possible, but it can take a long time to get rid of a bacterial infection that has woven itself deeply into the body’s organ systems. The benefit of Chinese herbal medicine for Lyme is that the powerful substances in the herbs can penetrate deep into the body at a cellular level. Working with an experienced acupuncturist means that your Chinese herbs for Lyme disease can be regularly updated, according to your individual needs, as you progress. This, in combination with acupuncture treatment for Lyme disease, moxibustion, and nutrition guidelines for an anti-inflammatory diet can all help patients feel better faster and prevent any further damage to the organs and the nervous system. Our TCM detox program may also be helpful.
Top 5 Tips for Lyme Disease Self-Care

Sometimes re-prioritizing health over all else is necessary in order to heal from a serious infectious disease.
- Conserve energy. Rest as much as possible.
- Drink extra water.
- Eliminate coffee, alcohol, spicy foods, chips, roasted nuts, any food that adds heat and inflames further. Try to reduce heat.
- Eat more cooling foods. Mung bean tea is an ideal choice.
- In the later stages of the disease, we may need to add more strengthening foods, like chicken stock and soup, and will recommend different herbal formulae, as well.
Overall, reducing stress and finding a meditation practice is helpful. For more detailed instructions on how to eat right to reduce inflammation, see our article specifically addressing anti-inflammatory food and lifestyle choices.
Acupuncture Near Me for Lyme Disease
Dealing with a complicated illness like Lyme disease is challenging for people and doctors. A long process of discovery and commitment may be necessary. Working with an experienced TCM provider gives patients the benefits of a multi-pronged, holistic way of addressing multiple symptoms, both physical and emotional. Acupuncture for infectious diseases like Lyme takes into account each patient’s individual concerns, and addresses the complex symptoms of Lyme in concert.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Lupus With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

What is Lupus? Lupus is considered a chronic autoimmune disease, a condition which causes the immune system to attack the body’s own normal tissues. The most common lupus symptoms are extreme fatigue and a particularly characteristic lupus butterfly rash, a skin rash that appears on the face. Acupuncture and TCM treatment for lupus can help to relieve joint pain, inflammation, rashes, and fatigue.
Lupus is much more common in women than in men, and usually first appears during a woman’s reproductive years – between the ages of 18-45. About 90% of people who have lupus are women. Women of color have an even higher risk of developing lupus.
As with other autoimmune diseases, the precise causes of lupus are somewhat mysterious. What causes lupus is still not clear to medical researchers. It may have something to do with a person’s genetic makeup. Because lupus is so much more common in women, it is believed that it may have something to do with estrogen, the female hormone.
There are different types of lupus. Systemic lupus erythematosus (SLE lupus) is the most common form of lupus, and it can affect the whole body, causing widespread inflammation and serious chronic fatigue.
Cutaneous lupus erythematosus primarily affects the skin, causing rashes, skin lesions (discoid lupus), irritated blood vessels, photosensitivity, and hair loss. The most common chronic form of cutaneous lupus is discoid lupus erythematosus, which causes scaly, round lesions to form on the skin. People with skin lupus are very sensitive to sunlight and must take precautions to avoid too much sun exposure, or even fluorescent lights. Lupus rash may resemble a bad sunburn.
Lupus nephritis is a form of lupus that can negatively impact kidney function. Inflammation of the kidneys can lead to high blood pressure, or excess protein or blood in urine.
It can often take a long time to get a lupus diagnosis. There is no one test that can conclusively show that a person has lupus. Doctors will generally look at a person’s range of symptoms, and run a variety of lab tests. An antinuclear antibody test (ANA) can indicate if the body’s immune system is producing autoantibodies–antibodies that attack normal tissue. Lupus symptoms can change, seeming to come and go, or “flare-up” when a person is triggered by something in their environment–often light exposure or emotional stress. During other periods of remission, symptoms abate, and a person with lupus may feel well for a while until another flare occurs.
Often lupus causes extreme fatigue, to the extent that people may find it difficult or impossible to get on with their daily work and activities when they are in the throes of a flare-up. The combination of chronic pain and chronic fatigue can lead to feelings of depression. With this kind of disease, a defeating sort of cycle can develop, in which stress, anxiety, pain, and fatigue keep feeding and perpetuating each other. Lupus is also associated with fibromyalgia; sometimes the two conditions overlap. Lupus also bears some similarities to Ehlers-Danlos Syndrome (EDS), and inherited connective tissue disease.
There is currently no cure for lupus. Medical treatment usually involves the use of medications like corticosteroids to reduce inflammation. Acupuncture and TCM can be used as an alternative or adjunct therapy for lupus, as acupuncture can help alleviate systemic inflammation, reduce joint pain, and help to improve fatigue. Acupuncture can also help to relieve the physical and emotional effects of stress and depression.
Top 10 Lupus Symptoms
Lupus can affect each individual person differently. Signs of lupus that might occur in both men and women include:
- Fatigue
- Joint pain and swelling
- Swelling in hands, feet, and/or around the eyes
- Headaches
- Low grade fever
- Butterfly rash on face, sores around the mouth and/or nose (lupus erythematosus)
- Hair loss
- Sensitivity to light
- Raynaud’s disease – loss of sensation in digits, finger and/or toes turn yellow, white or blue when cold, or under stress
- Chest pain when taking a deep breath

The lupus butterfly rash, also known as “malar rash”, may be the most distinctive symptom of lupus; it covers the cheeks and nose. The rash is red and patchy, caused by the dilation of capillaries under the surface of the skin, known as erythema, or lupus erythematosus. This lupus rash does not appear in every case, but it may appear in the majority of cases.
Other lupus symptoms can include: sores around the mouth, dry eyes, a rash around the eyes, problems with memory, a tendency towards anemia, an enlarged spleen, and a higher risk of blood clots.
Lupus anticoagulant (LA) is an antibody that is abnormally produced in some people with lupus. While its name sounds like it works against clotting; it actually does the opposite. High levels of LA can cause inappropriate blood clotting, or thrombosis. This problem can cause increased risk of miscarriage in women. Some people have LA without necessarily having lupus.
Women may experience menstrual problems like irregular periods or heavy bleeding that are related to lupus. Women with lupus are also at a higher risk for developing heart disease, kidney disease, and osteoporosis. Lupus symptoms women of color, in particular, (African-American women and Hispanic women) may develop are serious complications related to lupus at a younger age, including an increased tendency to suffer from seizures, strokes, and swelling around the heart.
Lupus Treatment
Rheumatologists specialize in treating musculoskeletal problems and the autoimmune diseases that often cause joint pain and inflammation, like rheumatoid arthritis, osteoarthritis, fibromyalgia, Lyme disease, and gout, as well as lupus.
Symptoms of joint pain due to lupus are usually treated with steroid medications like prednisone that help to reduce inflammation. Hydroxychloroquine, (an anti-malarial medication), is often prescribed to help prevent flares of symptoms from SLE lupus. Unfortunately, both of these types of medications can cause serious side effects, especially when they are used on a long-term basis. They do not address the root causes of lupus.
A relatively new treatment for lupus, Benlysta, is administered intravenously. It works by blocking a kind of protein that is involved in the production of autoantibodies – the immune cells that attack healthy tissues. This treatment, while different from other immunosuppressive drugs, can also cause side effects, including being more susceptible to infections. Some people have a severe allergic reaction to Benlysta, while others experience insomnia and severe depression.
Acupuncture for lupus and other rheumatologic conditions offers relief from painful symptoms and chronic fatigue without negative side effects.
How Can Acupuncture Help Lupus?

Lupus manifests as massive systemic inflammation in the body: in the tissues, organs, skin, and joints. Western medicine tends to always rely on cortisone/steroids to deal with inflammation, but this only works temporarily, like a band-aid.
Even though we don’t know exactly what causes lupus, we do know it is an endocrine disorder, or an inherited condition, or something in the environment that is causing the body’s atypical autoimmune response.
According to TCM, inflammation comes from too much heat in the body, or what we call “empty heat:” a lack of fluid. Without sufficient water, the body can’t control excess heat. We call this yin deficiency or kidney yin deficiency. This excessive heat condition can be triggered by external forces like the heat and light of the sun’s rays, or by spending a lot of time in a hot, dry space with a heater and no humidifier. This is part of what might cause the inflammation, fevers, and skin rashes associated with lupus.
Lupus nephritis, which involves the kidneys, is viewed by TCM as being related to deficiencies of qi or yang energy in the kidneys and spleen. Blood stasis can also be a part of the presentation. Treatment with acupuncture and herbs will often focus on removing blockages that cause stagnation of blood and qi, strengthening the kidneys, and clearing heat and toxins from the body.
Clinical trials in China have compared patients with SLE lupus treated with prednisone only to those treated both with steroids and Chinese herbs, and found that patients receiving TCM treatment as an adjunct fared better overall and were able to reduce their use of the steroids.
One study showed that 80% of participants experienced a significant improvement in joint pain, fatigue, and skin rash after ten sessions of acupuncture treatment.
Another case study of patients with discoid lupus showed that lesions had improved by 87% after receiving a course of auricular-acupuncture (ear acupuncture) therapy.
Top 3 Tips for Helping Lupus Naturally
Reducing inflammation at its source usually means making some changes in behaviors. Not only lupus, but other chronic illnesses like cancer, rheumatoid arthritis, etc. have so much to do with lifestyle and habits that are not conducive to optimal health. For a more thorough discussion of how to eat right and manage your habits to reduce inflammation, see our blog article specifically addressing Inflammation. Here are some basic anti-inflammatory habits to embrace:
- Reduce or eliminate all non-necessary drugs and medications. Long-term reliance on drugs to cover up pain hampers your ability to know what is really going on with your body. It also potentially damages the immune system and organs.
- Reduce or eliminate foods that create more heat and and acidity in the body. This includes coffee, alcohol, red meat, spicy foods, and crispy, fried foods. TCM nutrition provides very specific guidelines for warming and cooling foods, so working with a qualified acupuncture professional will be very helpful to each individual patient.
- Get adequate sleep – ideally, eight hours every night. This is when the immune system repairs itself. When people go for years, only sleeping three or fours hours a night, they can do serious damage, causing massive problems like lupus to develop.
It is up to you to care for your body as if it were your most precious resource, because it is. When you make your health your top priority, every decision you make about what to eat, when to sleep, and how to spend your time and energy matters. Be mindful of your own needs; don’t cover up your pain with drugs, or trash your body with junk food. Your best chance for a happy life starts with healthy habits.
Acupuncture Near Me for Lupus
Autoimmune disorders like lupus can be devastating, not only because they are physically and mentally debilitating, but because they can be so difficult for doctors to understand and treat effectively. The TCM approach to lupus is holistic and takes into consideration a person’s foundational constitution, lifestyle, and emotions, as well as looking carefully at which imbalances in the organ systems are causing the physical symptoms. If you have been diagnosed with lupus, or are not sure about what might be causing severe fatigue, joint pain, or skin rashes to flare up periodically, working with an experienced acupuncture practitioner may help you to manage these symptoms and experience a marked improvement in your quality of life.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Heel Pain With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

Chronic bottom of heel pain, especially when you first get up in the morning? Heel pain can be due to plantar fasciitis, an inflammatory condition of the large ligament that supports the arch of the foot. Bone spurs in the foot (heel spur), Achilles tendonitis, and bursitis can also cause pain in back of heel. Acupuncture and TCM treatment offer relief from chronic plantar fasciitis pain and achilles tendon pain.
Experiencing stiffness or pain in the heel when you first get up in the morning is a sign of plantar fasciitis. The sensation may improve as you warm up and move more throughout the day, or you may have severe, burning pain whenever you put your weight on the back part of your foot. The plantar fascia provides shock absorption and cushioning for the heel; when it is overused, small microtraumas and tears lead to inflammation. People with very flat feet, fallen arches, or very high arches are more prone to plantar fasciitis, as are older people.
Stiffness above the heel is an indication of Achilles tendinitis. When the tendon that connects the muscles of the calf to the heel bone is strained, it can cause an aching sensation or pain in the back of the heel. This usually happens because of sudden overuse, like when a person decides to go for a long run when they haven’t exercised in a while, or when their sneakers are worn out. Achilles tendinitis is more common in men, and in people with high blood pressure.
Stiffness in the ankle and side of foot pain can be due to posterior tibial tendonitis, which can develop when the heel bone shifts in such a way as to put extra stress on the outside of the ankle.
Heel spurs–extra bone tissue on the bottom or back of the heel–develop due to over-stress of the foot. In most cases, the bone spurs on the foot don’t cause pain in and of themselves, but they often coincide with either plantar fasciitis or Achilles tendonitis, and the conditions aggravate each other.
TCM modalities of acupuncture, electro-acupuncture, moxibustion, and herbal formulae have been shown to help relieve heel pain and inflammation due to all types of conditions, including plantar fasciitis and Achilles tendinopathy.
Top 5 Heel Pain Causes
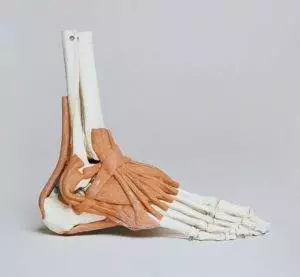
Pain in the heel and other types of bottom of foot pain can be due to one of or a combination of several different types of conditions:
- Plantar fasciitis – about 2 million people are diagnosed in the U.S. each year with plantar fasciitis, which occurs when the connective tissues that support the bottom of the foot become inflamed, usually from repetitive use or being overloaded. Some athletes are prone to this type of inflammation due to constant stress on the foot. Health conditions like obesity and diabetes also make people more susceptible to plantar fasciitis heel pain. While this type of heel pain walking is generally attributed to inflammation, it is also due to the natural degeneration of collagen that occurs with age, making the connective tissues weaker and more brittle.
- Heel spur – (bone spurs foot) refers to the extra growth of bone tissue on the bottom of the calcaneus (bone spur heel). Heel spurs often grow as the body’s reaction to plantar fasciitis; the two conditions can exist together or separately. Sometimes people with heel spurs aren’t aware of them, but bone spurs foot can cause sharp bottom of foot pain. Heel spurs often develop because of the stress of running or jogging, or wearing improper footwear. Posterior calcaneal exostosis, colloquially known as “pump bump”, is when there is abnormal growth of bone tissue on the back of the heel, usually due to wearing a certain style of shoe (pumps or high heels).
- Bursitis – Bursa are small sacs of fluid that help to provide cushioning in various joints of the body. Calcaneal bursitis occurs when the bursae that sit between the Achilles tendon and the heel bone become inflamed. Heel bursitis is usually caused by too much impact on the ankle joint and heel while running or by wearing shoes that create a lot of pressure on the back of the heel.
- Achilles tendonitis – (also spelled achilles tendinitis) When the tendon that runs from the heel up the back of the lower leg becomes inflamed, often due to a lot of jumping movements, it can create pain and stiffness in the back of the heel. This overuse injury is very common in middle aged adults who engage in sports like tennis or basketball only sporadically, and may not warm up adequately before running and jumping.
- Gout – an arthritic condition in which a buildup of uric acid crystals causes swelling and pain in the joints of the foot.
Pain in the heel can also be caused by a pinched nerve, or compression of the plantar nerve, or by bruising on the heel. Peroneal tendonitis, when the tendon that runs along the side of the ankle and then under the foot becomes inflamed and swollen, can also cause pain in the back of the heel. Sciatic nerve pain can also cause radiating pain that shoots down the leg and causes pain in the foot.
What Is the Treatment for Plantar Fasciitis?
Conventional clinical medicine considers plantar fasciitis to be a self-limiting condition, which means that it will eventually improve on its own, with rest and modifications of movement. Doctors will usually recommend that people cease weight-bearing activities as much as possible. This can be extremely frustrating for patients, though, as it often means being advised to rest the foot for six to eighteen months. Physical therapy for plantar fasciitis that focuses on stretching and strengthening the plantar ligament may be recommended. Special orthotics, arch supports, or heel cups that provide cushioning can be helpful. Night splints are sometimes used to keep the foot and ankle in a position that keeps the ligament on the bottom of the foot stretched long, rather than shortened, while sleeping.
For heel pain relief, doctors may administer steroid injections and other anti-inflammatory medications. Steroid injections do carry some risks; about one out of ten patients treated this way for plantar fasciitis pain experience a rupture of the plantar tissues, which can lead to an even more severely chronic condition. Of course, the problem with taking NSAIDS on a regular basis is that they can cause problems with the stomach lining and gastro-intestinal bleeding. If rest and other methods do not improve the situation after many months, then surgical release of the plantar fascia may be considered.
Achilles tendonitis treatment is usually similarly conservative, involving rest and pain relievers. Unfortunately, recovery from the heel pain caused by plantar fasciitis or Achilles tendinitis is often a long, tedious process of abstaining from physical activity. For many people, whether they have jobs that require them to be on their feet or simply enjoy engaging in sports, it may feel impossible to stick to the standard treatment program. Acupuncture treatment offers a way to help relieve pain and inflammation and speed the healing of plantar fasciitis.
Acupuncture for Heel Pain

TCM takes a holistic view of pain conditions such as heel pain. While undoubtedly heel pain is caused largely by inflammation in the soft tissues of the foot and calf, there are often other underlying factors that cause these kinds of injuries to happen to people in middle age. In TCM philosophy the kidneys are believed to provide support and nourishment to the bones; this concept is called “kidney governing bone.” Heel pain and heel spurs occur due to deficiencies or excesses of the kidney Qi. Soft tissues such as the plantar ligament and the Achilles tendon are governed by the liver. Thus, acupuncture treatment for heel pain, heel spurs, plantar fasciitis, and Achilles tendinitis will often involve using acupoints to strengthen and tonify the Kidney Qi and Liver Qi.
Acupuncture is known to be effective for helping to relieve pain due to inflammatory conditions of all kinds, and also for helping to increase the production of collagen, which helps to keep the connective tissues of the foot and calf strong and supple. Acupuncture helps the healing of ligaments and tendons by improving reducing inflammation, improving blood flow and cell repair. The ancient textbook of Chinese medicine, The Yellow Emperor’s Classic of Internal Medicine, even describes a specific acupuncture technique used to promote healing in the Achilles tendon.
Herbs can be used both internally and externally to help heel pain. An herbal formula that is steeped in warm water and used as a daily foot soak can be especially helpful for relieving swelling in the heel and pain in the bottom of the foot.
One research study compared patients treated with corticosteroid injections for plantar fasciitis versus patients treated with acupuncture. Six months later, the patients who had steroid shots reported a 76% effective rate, while the patients who’d had acupuncture reported a 97% effective rate.
A hospital study compared two groups of patients – some treated with integrated protocol of acupuncture and warm herbal foot baths, and the others treated with the herbal foot baths only. The effective rate for the foot-soaking only was 69%, and the effective rate jumped up another 22% for the patients who also had acupuncture.
A systematic review of four studies involving acupuncture for patients with plantar fasciitis heel pain showed a significant reduction in pain after 4-8 weeks of treatment.
Top 5 Tips for Heel Pain

Prevention of heel pain involves mindfulness around your preparations for physical activity. The right gear and the regular practice of plantar fasciitis exercises can help prevent injury to the tendons of the foot.
- Wear good-fitting, properly supportive shoes – whenever you walk, run, or work out. Replace them regularly, even if you haven’t worn them much, because cushioning materials can break down over time, even when the shoes are just sitting in your closet.
- Warm up – taking the extra time to warm up before and cool down after running and jumping is always important, for all of the muscles of the body, but especially for the feet and lower legs. Be sure to adequately warm up the calf muscles, and stretch them before and after your primary workout.
- Vary your workout – cross-training, which means alternating different types of activities, not only helps to improve your overall cardiovascular and muscular fitness, but it also prevents repetitive use injuries that can occur when you run every day. Focus on resting the feet some days, by riding your bike or swimming instead of running or doing high-intensity aerobics.
- Soak your feet – before bed, soak heels in warm water to help improve circulation.
- Manage your weight – Heel pain is usually related to how much pressure the foot has to withstand on a daily basis. Maintaining a lower body weight will help take the pressure off the heels. Losing weight while being asked to stay off your feet can be especially difficult, so talk with your TCM provider about a healthy food plan for weight loss.
Once your heel pain has improved, you will need to take these steps to prevent heel pain from returning in the future.
Acupuncture Near Me for Heel Pain
The typical treatment for heel pain can last for several months, with unpredictable results. If you have been suffering from plantar fasciitis or Achilles tendonitis, and want to heal from heel pain more quickly, it is worth it to give acupuncture a try. At Art of Wellness, we have over 30 years of experience helping patients get relief from pain conditions of all kinds. Get back on your feet again with acupuncture for heel pain!
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.