-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

March 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31
Uncategorized
How to Treat a Herniated Disc With Acupuncture & TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.
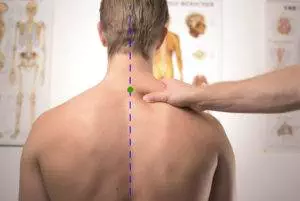
Why do I have a sharp shooting pain down one leg? What should I do if my neck is stiff and hurts to turn? What can I do to help a spasm in lower back? Any of these kinds of pain may be caused by a herniated disc, which presses on the spinal nerves. Acupuncture can be an effective treatment for relieving the symptoms of a slipped disc, while also speeding the healing process–all without negative side effects.
A herniated disc, often referred to as a “slipped disc,” or a bulging disc, occurs when damage to one of the shock-absorbing discs of cartilage that sit between the vertebrae creates pressure on the nerves and muscles of the spine. Also called a prolapsed disc, this condition creates inflammation and swelling in a localized area of the spine and can cause severe pain in the neck, lower back pain, sciatica pain, and tingling that radiates down the leg.
The vertebral column, or backbone, is made up of vertebrae (individual bones) and intervertebral discs. These discs provide cushioning in between the bones and act as ligaments that hold the bones together. The discs create a shock absorption system that protects the spinal column, and are made up of tough, fibrous outer layers of cartilage, with a gel-like substance on the inside. If there is damage to the tissues of the outer layer, the soft, gel interior can be pushed outwards and breach the outer wall. This can create pressure against the nerves of the spinal column, resulting in symptoms of nerve entrapment: pain, numbness, and/or loss of ability.
A herniated disc, also referred to as a “ruptured disc,” most often occurs in the lumbar spine. A lumbar herniated disc may cause severe lower back pain if it is pressing on a nerve. Pressure on the sciatic nerve area can also cause shooting pain, burning pain, numbness, and/or tingling in one or both legs–a condition commonly referred to as sciatica, also known as lumbar radiculopathy. The sciatic nerve is actually a large bundle of smaller nerves that connects the base of the spine to the top of the leg, travelling through the buttock area. There is a sciatic nerve bundle on each side. About 90% of cases of sciatica are related to herniated discs.
Cervical disc herniation refers to a prolapsed disc between one of the seven vertebrae of the cervical spine, or neck area. Compression of the nerves due to a herniated disc in the C2 area can cause headache, or pain in the eye or ear. Herniation of a disc further down the cervical spine happens most commonly in the C5, C6, or C7 area, which can lead to neck pain and/or shoulder pain.
Most of the time, sciatic pain or neck pain due to nerve compression in the spine goes away gradually on its own, but it can cause a lot of suffering over the course of several weeks or months before resolving itself. Medical treatment for herniated disc pain typically involves the recommendation of rest and immobilisation and the use of anti-inflammatory medications, muscle relaxers, and pain relievers. However, lack of movement does not really help improve the root cause of the pain, and the use of pain medications or steroids is often accompanied by unwanted side effects. Acupuncture treatment can significantly reduce acute pain related to sciatica, neck pain, shoulder pain, and low back pain due to slipped discs, often providing immediate, short-term relief of severe pain, while helping, long-term, to reduce inflammation and help heal nerve damage.
Signs of Herniated Disc
When a disc herniates, pain can be sharp and intense. Depending on which disc is affected, there may be neck pain, low back pain, or sciatic pain in the leg, foot, or buttock area. Pain or numbness are caused by the inflammation of the nerve area that is being compressed by the extrusion of the center of the disc.
- A cervical herniated disc (in the neck) may cause burning pain in the side of the neck or sharp pain in the back of the neck. Or there may be a more subtle sensation where the neck is tender to the touch. The pain is usually worse when performing vigorous activities or when twisting or turning the head at a certain angle. The overall movement of the neck and head may feel limited and stiff.
- Pain may radiate down the arm and cause an “electric shock-like” sensation in the hand and fingers.
- Weakness in the muscular movement of the shoulder, arm, hand, thumb and fingers may result from the pinching of the nerves of the cervical spine.
- A lumbar herniated disc (in the lower back) is more likely to cause pain down the leg than in the back. Usually the pain is just on one side of the body. This radiating pain caused by compression of the sciatic nerve can be sharp, burning, and very intense.
- Herniation of a lumbar disc can also cause pain in the low back or buttock. This pain may be of the “throbbing” type, or feel like a spasm. It may be helped by applying cold or heat to the area. The pain typically is worse after sitting or hunching over for a while, or when bending over from the waist.
- The sensation in the buttock, hip, leg and foot may be more like tingling or numbness than searing pain.
- “Foot drop” is when the nerve compression makes it difficult to fully pick up the foot when walking, so that the toes drag on the floor.
The kind of pain caused by a herniated disc can come on quite suddenly and strongly. Fortunately, the pain caused by most herniations of spinal discs resolves in a matter of time without surgery.
What Causes Herniated Disc?
Slipped discs, or bulging disks, happen most often to people between the ages of 30 and 50. The ruptured disk may happen due to one sudden movement, like lifting something heavy, twisting an awkward way, or even a strong sneeze. But prior to such an event, there was probably some weakness already developing in the outer walls of the disc.
Degeneration of the discs can occur over time due to aging. A chronic herniation can develop slowly over years and cause mild symptoms. An acute herniation might happen as the result of some trauma, like an accident, which could create more serious damage to the outer layers of the disc (the annulus fibrosus), allowing the jelly-like material inside (the nucleus pulposus) to extrude, or squeeze out of containment.
Surgery for herniated disc is only recommended in rare cases (10-20%), sometimes if the prolapsed disc is affecting the nerves in such a way that bladder or bowel function is negatively impacted. Surgery may also be considered if pain is severe and continues for a long time without getting better. Herniated disc surgery attempts to relieve the nerve compression by removing some of the disc tissue. In cases where there is more extensive degeneration of the spine, a spinal fusion procedure may involve “fusing” the vertebrae together with screws while removing the original disc tissue and replacing it with an implant. These types of surgeries for herniated disc may help alleviate pain, but there can still be a long recovery period, and the pain is not guaranteed to go away.
Can Acupuncture Help a Herniated Disc?

Traditional Chinese Medicine (TCM) has been developed over the course of thousands of years to deal with all types of pain conditions. In the TCM view, herniated disc pain is caused by:
- Injury to the spine
- Invasion of cold, wind, or damp
- Liver and/or kidney deficiency
In addition to acupuncture treatment, which involves the insertion of very fine needles into specific points along the meridians of the body, we also use treatments such as moxibustion and infrared heat lamps to bring warm energy to parts of the body. TCM treatment for herniated disc will often focus on strengthening the Qi (life force energy) and blood flow to the kidneys, and clearing dampness and bringing warmth to the whole lower back area.
One clinical trial conducted in a hospital demonstrated that acupuncture treatment combined with the application of moxa warm needle therapy with infrared heat and gentle exercise resulted in reporting of 95% improvement in pain related to lumbar herniated disc.
A recent systematic review of acupuncture treatment for disc herniation concluded that acupuncture provided better results than pain medications or lumbar traction.
A study that focused on long-term outcomes for patients with lumbar disc herniation showed that ten years after receiving electric acupuncture treatment for their pain they reported positive long-term results, acupuncture having helped to resolve their sciatica symptoms.
Top 5 Tips for How to Heal a Herniated Disc Naturally

Most pain due to herniated disc will resolve itself in about six weeks without medical treatment. In the meantime, there are some things you can do to help reduce pain and restore freedom of movement.
- Seek out treatment from a qualified acupuncturist. A combination of acupuncture, herbal supplementation, tuina massage, moxibustion, and infrared heat therapy will go a long way towards relieving pain and encouraging healing.
- Heat and Cold Therapy. Try using a heating pad or hot water bottle to apply gentle heat to the lower back or neck. Alternate with icing the affected area. This helps bring more blood flow to the area, reduces inflammation, and soothes stiffness.
- Stay active. It can be tempting to stay in bed when lower back pain and sciatica are causing intense pain or tingling sensations. But immobilisation does not really do anything to help heal nerve pain, and it is actually more beneficial to keep the muscles of the back body strong. Engaging regularly in low-impact activities like walking, biking, or swimming will help keep endorphins flowing and your mood positive better than bed rest will.
- Check your sleeping position. Staying in bed can also hurt when you have a slipped disc. Use a pillow to bolster your knees to help relieve tension in the lower back and keep the spine in proper alignment. Use a firm orthopedic pillow to keep the neck aligned.
- Nutrition for nerve health. Certain nutrients can be especially beneficial for building and maintaining nerve tissues. Emphasize B-6 and B-12 vitamins, Vitamin E and Omega-3 and Omega-6 fatty acids in your diet and with high quality supplements. Nuts, fish, and good plant-based oils should be consumed regularly.
Regular exercise, plenty of sleep, and good nutrition, as always, will go a long way towards helping ensure that a pain condition resolves itself fully and does not return.
Acupuncture Near Me for Herniated Disc
At Art of Wellness, Dr. Tan and Dr. Cai have over 30 years of experience helping patients with acute and chronic pain due to neurological conditions. Pain due to a herniated disc can be effectively reduced by regular acupuncture treatment, while Chinese herbs and therapeutic massage can help bring healing to the nerves and spine, and help prevent future problems with herniated disc and sciatica.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat High Blood Pressure With Acupuncture & TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

What is high blood pressure? Blood pressure (BP) is the force with which blood, pumped by the heart, pushes against the inner walls of the arteries and veins. When this force is consistently high, it puts a strain on the delicate tissues of the blood vessels and makes your heart work harder. This is also called hypertension. Most people take medications to control high blood pressure. In this article we’ll discuss how to manage high blood pressure with TCM and acupuncture.
High blood pressure is very common in older adults; about half of people over the age of 60 have high blood pressure. It is very important to have your doctor regularly monitor your blood pressure, because high blood pressure, if left untreated, can lead to heart disease, arrhythmia, heart attack, stroke, kidney disease, and many other serious, life-threatening conditions.
Your blood pressure reading is made up of two parts: systolic, which measures the force of blood being pumped away from the heart, and diastolic, the force of blood moving in between heart beats, when blood is flowing back into the heart. A normal blood pressure reading is usually considered 120/80 (systolic over diastolic). A consistent reading of BP over 130 would indicate hypertension stage 1, while a BP over 140 would be classified as hypertension stage 2. A BP over 180 signals a hypertensive crisis, and should be treated as an emergency, as it could lead to a stroke or other serious organ failure.
People with high blood pressure are advised to make lifestyle changes, including following a healthier diet, getting more exercise, and quitting smoking. Even a modest weight loss of ten pounds or so can make a big difference to reduce high blood pressure. Most people end up taking antihypertensive medications to lower blood pressure, often for the rest of their lives. Integrative care for high blood pressure that includes acupuncture treatment and herbal supplements according to TCM principles can provide natural remedies for high blood pressure, restoring the health of the circulatory system so that it might not be necessary to take drugs indefinitely.
Signs of High Blood Pressure
In many cases, there are no clear signs that a person has high blood pressure. Most people do not realize they have high blood pressure until it is measured by a medical professional. While people may think that a flushed, red face, or bouts of dizziness are symptoms of high blood pressure, these sorts of signals are not necessarily directly caused by high blood pressure. A flushed face caused by dilated blood vessels can happen for many reasons, usually because of a temporary rise in blood pressure due to heat, or cold weather, physical activity, spicy foods, hot drinks or alcohol, or a reaction to cosmetic skin products. Dizziness can actually be related to the side effects of medications prescribed for high blood pressure. The only way to know for sure is to check your blood pressure.
Many older people, especially women, with high blood pressure, experience bouts of dizziness that may be part of a hypertensive crisis – a sudden increase in blood pressure that can cause temporary dizziness or vertigo, tinnitus (ringing in the ears), or headache. A hypertensive emergency is sometimes the reason that a person visits a doctor to have a blood pressure check. It may be that hypertension has an effect on the peripheral auditory and vestibular systems, which can affect a person’s sense of equilibrium and orientation in space. High blood pressure can also contribute to problems with memory or cognitive function.
Top 10 Causes of High Blood Pressure
Many factors can lead to high blood pressure. Aging is one factor. If there is a family history of hypertension, you may be genetically predisposed to having high blood pressure, too. Other risk factors also increase the chances of high blood pressure:
- Smoking
- Diet high in salt and/or fat
- Lack of exercise, sedentary lifestyle
- Being overweight
- Stress
- Too much alcohol consumption
- Sleep apnea, snoring
- Thyroid and adrenal problems
- Kidney problems
- Diabetes
Medical diagnosis and treatment for high blood pressure don’t really focus on finding a root cause of the problem. General guidelines for eating less salt and fat, losing weight, and finding ways to reduce stress may help people reduce high blood pressure, but for most people, modest lifestyle modifications aren’t enough to solve the problem.
High Blood Pressure During Pregnancy
Some women develop high blood pressure during pregnancy. Called gestational hypertension, this occurs when a woman has elevated blood pressure during the last 20 weeks of pregnancy. While this type of high blood pressure usually goes away after birth, it can be an indicator of becoming hypertensive later in life. In some cases, having high blood pressure while pregnant can cause problems, such as fetal growth restriction, which may happen if not enough nutrients are being carried to the growing fetus through the blood vessels. If high blood pressure and high levels of protein in the urine are both detected, a woman may have preeclampsia, a serious problem that is believed to be caused by restricted blood flow to the placenta. Women with high blood pressure during pregnancy are more likely to experience preterm birth and to have unplanned delivery Caesarean section.
Conventional treatment for gestational hypertension typically involves monitoring and managing high blood pressure with medications. While not many clinical studies have been done regarding acupuncture treatment for gestational hypertension and preeclampsia, TCM has been used to treat high blood pressure and complications of pregnancy for thousands of years. From the TCM point of view, high blood pressure during pregnancy may be due to a deficiency of Liver and/or Kidney Yin, or rising Liver Yang energy in response to a Kidney Yin Deficiency, or Blood or Yin Deficiency. A TCM provider would use diagnostic methods to determine the differentiation and use acupuncture points to nourish the appropriate organs, promote better flow of Blood and Qi, and to help alleviate stress.
How to Control Blood Pressure with Acupuncture and TCM
Naturally, for many centuries, TCM practitioners had no way of measuring blood pressure with medical devices. They depended on observations of people’s symptoms, appearance, and careful checking of the pulse by hand. Thus, TCM does take into consideration the patient’s feelings and experience of symptoms of high blood pressure like:
- Dizziness or vertigo
- Palpitations
- Headache
- Fatigue
- Shortness of breath
- Weakness in the knees
- Memory loss
- Vision loss
TCM views dizziness as being a result of too much Liver Yang energy, stagnant Phlegm, Liver-Kidney deficiency, and deficiency or stagnation of Blood and Qi. Hypertension type headaches are caused by the addition of Fire energy coming from the stomach or intestine. Liver Fire can cause irritability and flushing in the face, while Heart Fire can cause chest distress, nervousness, and insomnia. Weakness and fatigue would be caused by the addition of Dampness and accumulated excess fluid. Fluid retention can lead to a distended abdomen, edema, and low back pain.
TCM philosophy also takes into consideration the emotional state as it relates to the physical health of the body. More recent scientific research also confirms that feelings of anger stimulate the sympathetic nervous system and contribute to high blood pressure and heart disease. Finding practices that help how to control anger and find calm are another important part of managing high blood pressure.
A TCM practitioner can treat all of these various symptoms with a combination of acupuncture treatment and herbal supplements individually customized for each patient’s specific circumstance.
One randomized study compared patients receiving acupuncture versus patients receiving sham acupuncture to treat hypertension over a six-week period. The patients who had real treatments showed significantly lower daytime and nighttime blood pressure readings. Another study showed that acupuncture treatment given to patients in conjunction with antihypertensive medications showed significant reduction in both systolic and diastolic BP readings.
As the results of this research study of many clinical trials concluded, regular acupuncture treatments have the effect of reducing blood pressure, with the effects lasting several days after each treatment. Acupuncture treatment generally has a cumulative effect, and it is necessary to stick with it to get results. It is also crucial that you work with your healthcare practitioner to determine which dietary changes and forms of exercise will best help how to reduce high blood pressure.
Acupuncture Near Me for High Blood Pressure
Managing high blood pressure takes commitment to making long-term lifestyle changes and regular monitoring. Adding acupuncture and TCM to your integrative care regimen may help you reduce high blood pressure, improve related problems like fatigue, dizziness, and headache, and avoid more serious health problems down the line.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Manage IBS Diet With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. & Xiaomei Cai, L.Ac., Ph.D.

What is irritable bowel syndrome (IBS)? IBS is a chronic gastrointestinal problem that causes uncomfortable changes in the body’s elimination process. One day you’re constipated, then a day or two later, you may have diarrhea. Pains move around the whole abdominal area, and your belly feels full and tight with excess gas. IBS treatment typically involves taking medications and following a special IBS diet, but many people continue suffering with no IBS cure. In this article, we’ll talk about how to get rid of IBS naturally with acupuncture and TCM.
IBS is a common digestive problem that can cause a lot of pain and anxiety around your daily bathroom habits. IBS can cause stress and even depression, compromising your ability to live life without worrying about when you’re going to have to go to the bathroom. Conversely, stress and anxiety function as triggers for bouts of IBS, so the problem becomes cyclical.
This gastrointestinal problem is called Irritable Bowel Syndrome because people who suffer from this disorder seem to have a more sensitive intestinal tract that is highly reactive to IBS triggers. Sometimes this condition is referred to as “spastic colon.” People who have primarily loose stools as a result of this condition are said to have “IBS-D” (diarrhea-predominant IBS), while people who suffer more from sluggish bowels have “IBS-C” (constipation-predominant IBS).
Many people never seek help from their medical providers for IBS treatment, perhaps because they think their discomfort is normal. The ever-changing nature of IBS means it’s hard to get a handle on what is actually happening. The pain in the gut seems to move around all the time, and bathroom habits can feel totally unpredictable. IBS can also lead to the bleeding and discomfort of hemorrhoids.
IBS Causes
According to conventional medicine, there is no one specific cause for Irritable Bowel Syndrome. Having a more highly reactive intestinal tract may be due to many factors, some more clearly mechanical in nature, others more having to do with psychological factors. Inflammation in the gut, gastroenteritis, stressful or traumatic situations, heightened sensitivity to movements and sensations within the abdomen, and miscommunications of the autonomic nervous system between the digestive organs and brain may all play a role in IBS.
We usually think of serotonin as being a hormone in the brain that affects mood and the ability to fall asleep. But serotonin is a neurotransmitter that also plays a key role in the function of the gut, affecting how the intestines move and secrete gastric juices, as well as how we viscerally perceive these functions. Changes or abnormalities in serotonin release or uptake seem to be one of the issues related to IBS.
Top 5 IBS Triggers are:
- Stress
- Abnormal levels of serotonin in the digestive tract
- An infection or abnormal level of bacteria in the digestive tract
- Strong reactions to certain foods/Celiac disease
- Weak colon muscle action
IBS involves, on some level, problems with both the motor function of the bowel itself and the extent to which a person is physically aware of “stuff going on” in their intestines and colon. Inflammation from infections or hormone changes caused by the menstrual cycle can also directly affect bowel motility. Those same things can cause a person to be hypersensitive to every little movement of the intestines, making them feel like painful cramps.
IBS and Gut Health
The balance of gut bacteria, or “flora” in the intestines, has been more recently shown to play a vital role in overall health. Gut bacteria are instrumental in the proper functioning of the immune system and the assimilation of nutrients from our food. The balance of the gut flora can be disturbed by taking antibiotics or a gastric infection, such as norovirus or other flu-type illnesses. Medical science is still making strides in learning how the health of the gut is very closely connected with the brain. It is becoming clear that gut health is inextricably related to mental health.

We know that stress, both chronic and acute, can cause all kinds of health issues. The mind-body connection is particularly apparent when it comes to IBS triggers. Feelings of anxiety create a ripple effect through the middle of the body, affecting the whole digestive system, causing pain and volatile action. Fear, shame, and even feelings of panic about having to run to the bathroom keep the whole process in a repeating loop.
IBS treatment often involves antibiotics or probiotics, but this has not been shown to be effective long-term. Many times doctors will prescribe medicines for anxiety (like Valium or Atavan) or depression to help provide IBS relief. However, these pharmacological treatments do not really address the root causes of the syndrome, and they may cause negative side effects, and sometimes create a dependency on the medication.
Top 5 Signs of IBS
A syndrome is a collection of symptoms that often appear together for which there is no clear medical explanation. According to conventional medicine, irritable bowel syndrome is evident when a person has frequent abdominal discomfort, which could mean a “stomach ache” or cramping, and bouts of constipation or diarrhea, or sometimes both, in alternation. In other words, IBS is signified by changes in the frequency or consistency of bowel movements, accompanied by marked discomfort before having them.
Top 5 Symptoms of IBS are:
- Abdominal pain
- Bloating and excess gas
- Constipation and/or diarrhea
- Mucus in the stool or other irregularities
- Nausea
IBS is more common among women than men. This may be due to fluctuations in hormones that affect the chemical balance and muscle action of the intestines. Women may experience more IBS symptoms in conjunction with their menstrual periods, or as a PMS symptom.
Conventional treatment for IBS typically involves the offering of various medications to deal with these symptoms. Anti-spasmodics may be used to help reduce cramping and contractions in the bowel, and anti-diarrheal medications such as Imodium may slow down the movements of the bowel, but these IBS medications do not help to restore true balance to the digestive system.
How to Treat IBS With Acupuncture
TCM and acupuncture work according to holistic principles, meaning that we are careful to look at the whole picture of what is going on with a person: emotionally, spiritually, physically, nutritionally, and energetically. According to TCM philosophy, the spleen is the organ responsible for processing our food and turning it into energy. IBS treatment with acupuncture is a matter of aligning the communications between the Shen (the mind) and the Spleen. Deficiency of the spleen is the primary TCM diagnosis for most patients with IBS symptoms. It is equally important to address problems of the Shen at the same time.
The most common TCM differentiations of IBS patterns are:
- Spleen Deficiency with Liver Qi stagnation: symptoms of this condition include diarrhea, mucus in the stool, abdominal pain, cramping, gassiness, bloating, irritability, and depression with lots of heavy sighing.
- Spleen Deficiency with Stomach deficiency: shows symptoms like watery stools, feeling of fullness and distension after eating, poor appetite, a pale complexion and fatigue.
- Spleen Deficiency with Kidney Deficiency: symptoms include diarrhea, especially in the morning, partially digested food in the stool, aches and pain in the abdomen, lower back, and knees, with a sense of coldness.
Moxibustion is a TCM treatment used in addition to acupuncture to treat IBS. One study showed that acupuncture treatment combined with moxibustion to get rid of IBS was extremely effective for reducing both the discomfort and frequency of bowel movements.
Another study that tested both herbal formulations and acupuncture treatment on patients with IBS showed that both methods were effective at reducing symptoms.
Acupuncture treatment will also focus on reducing stress, anxiety, and fatigue. Acupuncture has been shown to help restore the balance of serotonin levels, as well.
IBS Diet According to TCM
Chinese herbs, as always, are also integral to the successful treatment of IBS. In the TCM philosophy of healthcare, nutrition is considered to be just as important as acupuncture, moxibustion, herbal formulae, and other forms of therapeutic treatment. Herbs are a way to get nutrients into the body that are not necessarily present in the foods we commonly eat. TCM practitioners are trained extensively in the energetic and nutritional values of food and will spend time working with patients to modify eating habits and focus on a special IBS diet. Apart from reducing common problems like excessive coffee and alcohol intake, your acupuncturist will work with you to discover which foods act as IBS triggers for you and help you to make the most beneficial modifications to your IBS diet plan.
Top 5 Acupressure Points to Help IBS
Acupressure can be a very effective means how to treat IBS naturally yourself. Acupressure uses the same collection of points located along the meridians of the body as acupuncture to help eliminate blockages and encourage blood and Qi to move freely through the body. These points located along the spleen, bladder, stomach and “conception vessel” meridians can help provide IBS relief. The conception vessel meridian runs up the front and center of the torso, from the pubic area to the mouth. Also known as the “Sea of Yin,” this channel is instrumental in directing all the yin energy in the body. As it is very exposed, this energy center can feel vulnerable, and may be where we tighten up, hunch over, and try to hide and protect ourselves. Tension along this channel can be a major energetic factor in the cramping and spasming actions of IBS.
Try these top 5 acupressure point for IBS relief:
- CV6 – located two finger-widths beneath the navel, gently rubbing this point with circular motions helps to relieve belly pain, cramping,

Spleen 4 acupressure point and constipation.
- CV12 – located at the midpoint between the lower end of the sternum and the navel, rubbing this point in a circular motion can help relieve gas pain, bloating and acid reflux.
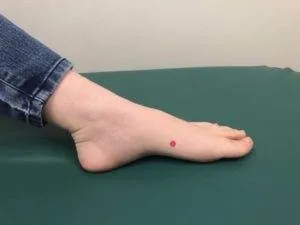
- SP4 – located on the inner edge of the foot, right above where the arch begins, stimulating this spleen point can help relieve gastric spasms and diarrhea.
- UB25 – these two points in the lower back, right beneath LV-4, can help relieve abdominal distension, constipation, and lower back pain.
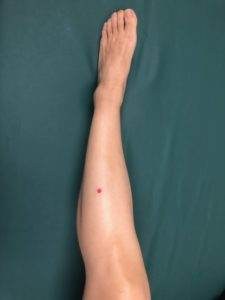
- ST37 – also known as the “Upper Great Hollow,” these points are located along the outside edges of the shin bones, a few inches below the knees. Pressing firmly here can help relieve abdominal pain, constipation and diarrhea.
Acupuncture Near Me for How to Solve IBS
If the IBS signs described here sound familiar because you or someone you know has been suffering from frequent abdominal discomfort and constipation or diarrhea, or both, it is important to seek help and advice from your healthcare providers. When conventional IBS treatment doesn’t seem to be helping, acupuncture and TCM may help you find IBS relief. Call us at Art of Wellness to get started with an IBS diet plan and course of acupuncture treatment.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Neuropathy With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D.
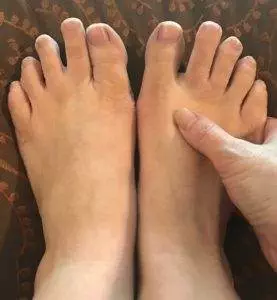
Neuropathy pain and tingling, often in the hands or feet, is caused by damage to the nervous system. Dysfunction of the sympathetic nervous system can also interfere with autonomic internal processes like blood pressure and digestion. Relieve the effects of nerve damage with integrative care that includes acupuncture and TCM.
Neuropathy refers in general to the dysfunction or disease of one or more nerves, causing pain, sensitivity, and/or degenerative atrophy in parts of the body, usually the extremities. The most common form of neuropathy is peripheral neuropathy, in which damage to the peripheral nervous system–the signalling system that allows the brain and spinal cord to communicate with the rest of the body–leads to a breakdown in communication.
Peripheral neuropathy is believed to affect about 30 million people in the U.S. In some cases, neuropathy causes severe pain and can be disabling. Neuropathy in feet may be the most recognizable form of this condition, but different kinds of nerve damage can affect many parts of the body.
Symptoms of neuropathy vary widely from person to person, so it can be challenging to get a specific diagnosis. Some types of neuropathy develop slowly over many years (chronic neuropathy), while others can come on quite suddenly (acute neuropathy). There is currently no cure for neuropathy, and conventional medicine has limited ways of addressing the underlying causes of most neuropathies. Medical treatment mostly focuses on relieving painful symptoms with medications.
Studies have shown that acupuncture and TCM present an effective form of complementary or alternative treatment that can work upon the deeper dysfunctions that led to the degeneration of the nervous system in the first place.
Symptoms of Neuropathy
The signs of neuropathy can be subtle or severe, and appear in widely different combinations. The most common symptoms of peripheral neuropathy include:
- Tingling or numbness in hands and feet
- Burning or sharp pains in the limbs
- High sensitivity to touch, temperature
- Conversely, an inability to sense temperature or external pressure–loss of sensation
- Lack of coordination, balance, tendency to fall
- Muscle twitching, cramping, or weakness
- Lightheadedness or dizziness when rising to standing position
- Problems with control of the bladder and/or bowel
- Loss of sexual function
- Unintentional weight loss
Diagnosis of neuropathy usually involves a combination of electrodiagnostic tests to measure the electrical activity of nerves and muscles and blood tests to determine deficiencies, toxicity and/or abnormal immune responses. Quantitative Sensory testing can help determine the extent of nerve damage that exists, and Autonomic testing can assess whether there is damage to the autonomic nervous system, which controls things like blood pressure and sweating to manage body temperature.
Top 10 Types of Neuropathy
In general, the major types of neuropathy are known as: peripheral, proximal, cranial, autonomic and focal. There are over 100 different kinds of specific neuropathies that affect different parts of the body in various ways, depending on where nerve damage has manifested. The most common types are discussed in detail below.
-

carpal tunnel syndrome is a type of compression neuropathy Peripheral neuropathy – The peripheral nervous system transmits messages from the brain and spinal cord to the rest of the body.The somatic nervous system is made up of the cranial nerves and spinal nerves, which send messages between the brain and the periphery regarding voluntary movements, such as rising, walking, and picking up objects. When these systems sustain damage and become compromised, symptoms such as tingling, burning, numbness in the extremities, extreme sensitivity to touch, muscle weakness, loss of balance and coordination, or even paralysis can result.
- Autonomic neuropathy – The autonomic nervous system controls the body’s basic functions, such as the pumping of blood, the emptying of the excretory organs, and the digestive processes. When the small fibers of nerves lose their function, the fine movements necessary for the contraction of blood vessels are compromised, leading to inabilities of the organs to perform their usual activities.
- Sympathetic Nervous System Neuropathy – The sympathetic nervous system controls the body’s ability to react under urgent circumstances, triggering the “fight or flight” response. The rush of hormones causes a rise in heart rate and extra blood to flow to the muscles. Problems with the nerves that control this response are especially common in patients with diabetes and can have a negative impact on cardiovascular function, impairing coronary blood flow.
- Central neuropathic pain syndrome – due to damage to the central nerve system or spinal nerves, usually caused by a spinal cord injury, brain injury, or stroke. Can cause sharp, burning pain in localized areas, or throughout the body. Sometimes accompanies other chronic conditions like multiple sclerosis or Parkinson’s disease.
- Compression mononeuropathy – Damage to a single nerve can cause pain, numbness, and/or loss of use of a specific part of the body, as in carpal tunnel syndrome, which affects the hand, wrist and arm, cubital tunnel syndrome (ulnar neuropathy), in which ulnar nerve entrapment compresses the ulnar nerve of the elbow, radial tunnel syndrome compressing the radial nerve, and femoral nerve dysfunction, which affects the leg, causing numbness in thigh or femoral nerve pain.
- Neuropathic arthropathy or Charcot’s Joint – a progressive condition that causes severe damage to the bones, cartilage, and soft tissues of joints, usually the ankle and foot area. This extreme form of arthritis occurs when a person has nerve damage to the extent that they cannot feel the grinding of bone on bone.
- Neuropathies of the 12 Cranial Nerves – damage to the nerves of the brain and brainstem can lead to dysfunction of the muscles that manage the movements of the eyes (optic nerve), or Bell’s Palsy, which affects the muscles of the face.
- Thoracic and Lumbar Radiculopathy – A rare type of neuropathy, pinching or damage of the spinal nerves can cause pain around the chest (thoracic) or pain that radiates from the lower back (lumbar).
- Proximal Neuropathy – causes pain and weakness in the muscles of the hip, thigh and/or buttock, usually on just one side of the body.
- Unilateral Foot Drop – compression of the peroneal nerve in the leg causes difficulty in lifting the front part of the foot. People with this type of neuropathy, sometimes called “drop foot,” may drag their toes along the floor as they walk.
What Causes Neuropathy?
Chronic neuropathy is usually a secondary condition related to some other form of chronic disease. Diabetes is the most common and well-researched cause of neuropathies. Upwards of 60% of people with diabetes experience some form of nerve damage. Over time, high blood sugar levels cause weakening of the blood vessels that provide nutrients to nerve endings.
The main factors that can lead to various neuropathies include:
- Diabetes
- Traumatic injury that damages nerve tissues
- Side effects of medications or chemotherapy
- Autoimmune and inflammatory conditions
- Cardiovascular disease – narrowing of the arteries
- Kidney problems
- Poor diet, overuse of alcohol
- Exposure to toxins
Damage to peripheral nerves is a common side effect of chemotherapy treatment for cancer. Many people who undergo chemotherapy experience some form of neuropathy that continues long after the round of treatment has ended.
Medical treatment of neuropathy often involves the management of the related chronic conditions, especially diabetes, with lifestyle changes. Proper management of diet can certainly help prevent and improve neuropathy symptoms, but it is difficult for most medical practitioners to spend much time counseling patients on nutrition and behavioral modification. Medications such as Lyrica, Neurontin, Cymbalta and Elavil are often prescribed to help manage the painful symptoms of nerve damage. These can help dull pain, but do not fundamentally treat the condition, and possible negative side effects include leg swelling, weight gain, and fatigue.
Acupuncture and TCM offer a safe alternative for treating neuropathy symptoms stemming from diabetes, chemotherapy, inflammatory and other conditions.
How Does Acupuncture Help Neuropathy?
According to TCM theory, peripheral neuropathy is related to dampness hampering the smooth flow of Qi and blood to the limbs. Acupuncture treatment, therefore, will focus both on resolving the underlying condition causing the dampness to accumulate and clearing the blockages in the energy pathways (meridians) so that Qi and blood can move freely again.
Nutrition is an integral part of TCM, and a qualified acupuncturist will be able to give specific advice for each individual on how to modify diet to help address underlying conditions affecting the health of the nervous system. Your acupuncturist will likely also introduce herbs that provide additional nutrients to balance the system. These medicinal herbs are sourced from plants and contain properties we do not get from the and vegetables we eat on a daily basis. TCM considers herbal supplements to be an important extension of the diet to enhance health.
One study conducted with patients with Type 2 diabetes compared results of patients using medications only versus those who also received acupuncture treatment. The acupuncture group saw vast improvement over the medication-only group, not only in relief of painful symptoms, but in disability scores as well.
A study comparing a group of patients who got acupuncture versus those who received sham acupuncture showed that the people who had real treatment showed improvement in sensory and motor function in a fifteen-day period.
Another study designed to look at the long-term effects of acupuncture on neuropathy pain showed that people who had received ten weeks of acupuncture treatment were able to reduce their use of medications, and the majority of patients reported that they were still feeling the benefits up to a year later.
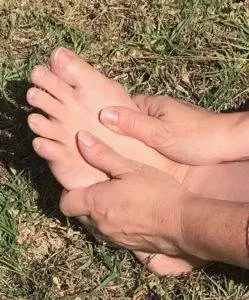
Top 5 Tips for Care of Neuropathy in Feet
People with neuropathy are highly susceptible to seemingly small injuries to the feet that can quickly turn into serious infections. Because sensation is diminished, sometimes a small stub is not felt until it has already become problematic.
- Wash feet and dry them carefully every day. Check for any sores or swelling, and address immediately with ointment and appropriate bandaging.
- Massage your feet every day. Rub the tops and bottoms until they are warm. This encourages circulation and stimulates good sensitivity.
- Wear socks and shoes that provide support and cushioning without compression or irritation.
- Move the feet regularly. Even when you must sit for long periods, make a point of removing your shoes to stretch and wiggle your toes. Elevate the feet when possible.
- Don’t go barefoot or wear flimsy shoes. It is so easy to injure the feet this way, and you may not be conscious of a small abrasion until it is already infected.
Acupuncture Near Me for Neuropathy
Our doctors at Art of Wellness have over 30 years of experience helping patients with chronic pain and neurological conditions. If you or a loved one has been suffering with neuropathy pain, please contact us to set up an initial consultation. We partner with you and other members of your healthcare team to provide the very best in integrative care.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Acid Reflux with Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Acid reflux, also known as heartburn, is the most common symptom of GERD (gastroesophageal reflux disease), a chronic disease in which the contents of the stomach move upwards into the esophagus, irritating the lining of the food pipe and causing burning pain in the chest, among other symptoms.
It is estimated that at least 40% of adults experience heartburn symptoms at some point in their lives, while up to 20% experience heartburn at least weekly, making GERD one of the most commonly diagnosed digestive disorders in the US. If a person is experiencing GERD symptoms frequently, doctors will usually try to treat acid reflux with medications called proton pump inhibitors (PPIs) and lifestyle changes. However, in many cases, patients will continue to suffer with symptoms beyond chest pain and regurgitation, often in concert with other common digestive complaints like dyspepsia (indigestion), IBS (irritable bowel syndrome), and ulcers in the stomach, necessitating further investigation and treatment.
TCM and acupuncture offer an alternative course of action to deal with acid reflux and many other digestive disorders. Acupuncture treatment has been shown to be even more effective than medications for heartburn relief. Acupuncture and herbal natural remedies for heartburn provide long-term positive results for GERD symptoms by helping to resolve the digestive disorder at its origin.
Acid Reflux Symptoms
Gastroesophageal reflux disease is characterized mainly by the reverse flow of digestive fluids up into the esophagus. When this occurs regularly over time, it can damage the lining of the esophagus and cause other problems. The sensation of “heartburn” is the most commonly known symptom of acid reflux, but it is possible to have GERD and not experience this burning sensation. GERD can occur with other non-acidic digestive fluids and may not cause the type of pain caused by acidic stomach juices. GERD symptoms include:
- Burning in chest, worse after eating and when lying down
- Chest pain, even when you haven’t eaten
- Difficulty swallowing
- Regurgitation of food or sour-tasting liquid
- Excessive salivation
- Sensation of a having a lump in the throat
- Excess gas in stomach and bloating
- Intolerance of certain foods and beverages
- Bad breath, or a constant sour taste in the mouth
- Hoarse voice or laryngitis
- Constant need to clear the throat
- Chronic dry, sore throat
- Burning sensation in the mouth
- Inflammation of the gums and other dental problems
Acid reflux symptoms may appear at the same time as other symptoms like stomach pain, stomachache, and stomach cramps. These may be stomach ulcer symptoms, gastritis symptoms, or signs of dyspepsia, as it is common for two or more of these digestive issues to coexist.
Heartburn Causes

While there is no single clear cause of GERD, it is usually related to the functioning of the lower esophageal sphincter (LES), the ring of muscle that separates the esophagus from the stomach. The LES, when it works correctly, allows chewed food matter to pass into the stomach, then closes to prevent matter from the stomach from flowing upwards. When this sphincter is relaxed or weakened, the contents of the stomach can breach this barrier. This can happen due to pregnancy or excess weight in the belly pushing upwards on these organs. Sometimes it may be due to a hiatal hernia, which can cause the upper part of the stomach and LES to push through the diaphragm muscle into the chest area.
Heartburn can be triggered by eating spicy or acidic foods, by smoking or inhaling second-hand smoke, or the use of aspirin or ibuprofen, as well as some blood pressure medications. If abstaining from these triggers does not help, patients may be referred to a gastroenterologist for investigative testing to pinpoint the problem. Endoscopy of the upper GI tract can show whether there is a hiatal hernia, stomach ulcers, or damage to the esophagus.
Acid Reflux Treatment
Many people take over the counter antacids (like Tums, Rolaids, Maalox, or Mylanta) to try to get heartburn relief. These may help alleviate the burning sensation temporarily, but using antacids frequently can actually exacerbate the problem by creating more stomach acid. Histamine (H2) blockers (like Pepcid and Zantac) can help reduce production of acid, but they don’t work for everybody. PPIs (like Prevacid, Prilosec, and Nexium) work by blocking the production of stomach acids.
These GERD medications can help with healing stomach ulcers and reducing acid reflux, but there are downsides. These drugs are very expensive, and many people end up using them on a daily basis. PPIs also inhibit the output of certain enzymes, which creates a negative interaction with common heart disease medications. They can also reduce absorption of calcium in the digestive tract, which can lead to weaker bones and increased risk of fractures. PPIs can also affect kidney function and increase the levels of bacteria in the stomach; if this bacteria makes its way up into the chest area due to reflux, it can get into the lungs and cause higher risk of pneumonia and other respiratory infections.
Asthma and GERD are often considered to be related conditions, because acid reflux can irritate tissues that trigger asthma attacks, while asthma attacks can cause a weakness in the LES that triggers reflux. Asthma medications like theophylline can also cause heartburn attacks. People who suffer from both GERD and asthma need to manage both conditions in tandem.
Prescribed medications called prokinetics cause the stomach to empty more quickly, reducing the chances of reflux. However, they can also cause side effects like nausea, diarrhea, fatigue, anxiety and depression, as well as having contraindications with other prescriptions.
All of these medical treatments focus on the stomach acids that cause heartburn. Currently, there is no conventional treatment that helps to restore the normal functioning of the LES. Research has indicated that acupuncture treatment, in addition to helping regulate gastric secretions, may help to strengthen the motor function of the LES.
Acupuncture and Herbs for GERD
Traditional Chinese Medicine (TCM) is a holistic system of medicine founded on over 3000 years of recorded research and practice. In TCM, all health problems are viewed as imbalances caused by blockages of Qi (life force energy) in the body. Disorders of the organ systems are often linked to emotional disturbances. According to TCM, acid reflux and other digestive problems are influenced by stress and anxiety. Long-term, ongoing feelings of worry, frustration, and anger impact the liver, spleen and stomach, increasing acidity and inflammation in these organ systems.
An “upset stomach” and feelings of tightness and pain in the chest are caused by Qi rising inappropriately, causing the backflow of acids. Acupuncture treatment for GERD focuses on calming anxiety, and restoring the downward flow of Qi, while toning the stomach and LES to improve their motor function.
TCM uses herbal formulations, developed over many centuries, to support the proper functioning of the internal organs on a deep nutritional level. Herbal remedies for acid reflux in TCM work to increase healthy mucus in the esophagus, soothing and healing damage from stomach acids.
An acupuncturist is also likely to ask questions about dietary habits, as certain foods are likely to be part of the problem. Working together with a qualified TCM practitioner to plan meaningful lifestyle changes, specific to each individual, will also help resolve heartburn, stomach pain, and indigestion.
TCM for Heartburn During Pregnancy
Many women experience acid reflux, which can happen at any time during pregnancy. This is due to hormone changes that can relax the LES so that it doesn’t close completely. In the later stages of pregnancy, the uterus pushes up on the digestive organs and diaphragm. According to TCM, stomach fire, indicated by a craving thirst for cold drinks, may need cooling. Stagnation in the digestive organ system can cause belching and bloating. Acupuncture treatments can be tailored to address these conditions, improving digestive flow and balancing hormones. Acupuncture can also help if baby is showing signs of colic or infant reflux.
Top 10 Tips for GERD Diet and Lifestyle

Creating and maintaining balance between Yin (cool) and Yang (warm) energies in the body and spirit is central to treating heartburn with TCM.
- High fiber diet – eat oatmeal and plenty of cruciferous vegetables like cauliflower and broccoli.
- Avoid citrus fruits (oranges, lemons, limes, grapefruits) and emphasize melon, bananas, apples and pears. Tomatoes and pineapple are also highly acidic and can cause problems, as can onions and garlic. Citric acid is also a common food additive and should be avoided.
- Eat several small meals per pay – eating larger amounts at one time increases the chance of the stomach becoming distended.
- Reduce fatty foods – high-fat foods stay in the stomach longer. Avoid fried foods, dairy ingredients and marbled meats.
- Avoid alcohol, especially red wine
- Avoid caffeinated drinks: coffee, tea and sodas can all trigger heartburn.
- Drink ginger or chamomile tea, which are both soothing to the stomach. Green tea can also positively stimulate the LES.
- Don’t lie down after you eat. Eat at least two hours before you intend to go to bed.
- Watch your workout positions: movements that affect your abdomen can cause reflux. Crunches, sit-ups, leg lifts, headstands, downward dog and other poses should be done carefully if at all. Never exercise on a full stomach.
- Sleep with your head elevated above your feet. A wedge-shaped foam lift will work much better than stacking pillows. Or, attach risers to the feet at the head of your bed.
Best Acupuncture Near Me for Heartburn Relief
Acupuncture treatment for heartburn is a safe and effective acid reflux remedy. If you or someone you know is suffering from GERD, acid reflux, gastroparesis, stomach pain, or symptoms of ulcer, we hope that you will not hesitate to find an acupuncturist in your area to schedule an initial consultation. We are practicing at Art of Wellness in Santa Monica, one of the top 20 acupuncture clinics in the greater Los Angeles area.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.