-
 Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
Art of Wellness Acupuncture & Traditional Chinese Medicine (TCM)11704 Wilshire Blvd, Suite 295, Los Angeles, CA, 90025
myartofwellness@gmail.com310-451-5522 Office Hours
MonClosedTue7:30 am --4 pmWed7:30 am --4 pmThu7:30 am -- 4 pmFri7:30 am -- 4 pmSat7:30 am -- 4 pmSunClosedOur office opens from Tuesdays to Saturdays 7:30 am to 4 pm, will be closed on Memorial day, Independent day, Labor day, Thanksgiving day, Christmas and New year.
-
Recent Posts
- How to Treat GTPS With Acupuncture and TCM
- Acupuncture for Sciatica Pain
- Can Acupuncture Help With Bladder Control?
- How to Treat De Quervain’s Tenosynovitis With Acupuncture and TCM
- Chinese New Year 2026: Year of the Horse
- Acupuncture and TCM Treatment for Perimenopause Symptoms
- How to Treat Insulin Resistance With Acupuncture and TCM
- How to Treat Metabolic Syndrome With Acupuncture and TCM
- How to Treat Syncope With Acupuncture and TCM
- How to Treat Thoracic Outlet Syndrome With Acupuncture and TCM
- How to Treat Dupuytren’s Contracture With Acupuncture and TCM
- How to Treat Nutcracker Syndrome With Acupuncture and TCM
- How to Treat Rosacea With Acupuncture and TCM
- How to Treat Perioral Dermatitis With Acupuncture and TCM
- Lymphatic Drainage With Acupuncture and TCM
- How to Treat Turf Toe With Acupuncture
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

June 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30
Inflammation
How to Treat Cervical Radiculopathy With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Neck pain? Stiff neck? These could be signs of cervical radiculopathy caused by a pinched nerve in neck. Acupuncture and TCM can provide neck pain relief and address the underlying causes of cervical radiculopathy.
Cervical radiculopathy occurs when a nerve in the neck becomes compressed or irritated where it branches away from the spinal cord. This is often referred to as a “pinched nerve.” This condition can lead to neck pain, weakness, and other symptoms not only in the neck but radiating into the arms and hands as well.
Cervical radiculopathy can be caused by several different factors, most of which involve some form of nerve compression in the neck.
One of the most common causes is a herniated disc, also known as a slipped disc in neck, or bulging disc in neck. This happens when the gel-like center of a spinal disc pushes out through a crack in the tougher exterior, putting pressure on a nearby nerve root. This can happen due to injury or degeneration over time.
Cervical spondylosis, also known as neck arthritis or cervical osteoarthritis, is a common age-related condition that affects the joints and discs in your neck. As the discs and cartilage between the cervical vertebrae wear down, this can cause neck pain and stiffness.
Degenerative disc disease and osteoarthritis are also common causes of a pinched nerve in neck. As we age, the spinal discs lose water content and shrink, leading to decreased cushioning between the vertebrae. This can cause the bones to rub against each other and lead to the formation of bone spurs, which can press on nerves and cause radiculopathy.
Another potential cause is spinal stenosis, which is the narrowing of the spaces within the spine. Lumbar spinal stenosis can result from a variety of factors, including thickened ligaments or overgrown bones, and leads to pinching or compression of the nerve roots as they exit the spinal column.
Additionally, trauma or injury to the neck, such as from car accidents or sports injuries, can directly damage the vertebrae or discs and result in a pinched nerve.
In more rare cases, tumors or infections in the spine may also cause cervical radiculopathy by compressing nerve roots.
Top 5 Symptoms of Cervical Radiculopathy
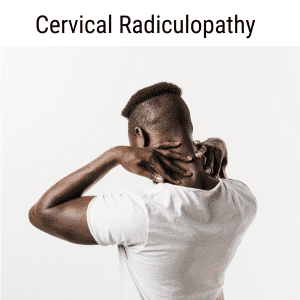
Pain in the neck and shoulders and headache are the most common symptoms associated with cervical radiculopathy. Poor reflexes and muscle weakness can also occur with a pinched nerve in the neck.
- Neck and shoulder pain – sharp or burning pain that starts in the neck and may radiate down the shoulder, arm, and hand
- Neck Stiffness – difficulty turning or moving the neck, neck muscle pain, muscle spasm in neck
- Numbness or Tingling in the shoulder, arms, or hands due to nerve compression.
- Muscle weakness in the arms or hands, trouble gripping or lifting objects.
- Neck pain and headache, headache that starts with neck pain
Diagnosis and Treatment for Cervical Radiculopathy
Diagnosing cervical radiculopathy can be challenging because its symptoms—such as neck pain, numbness, or tingling radiating down the arm—can overlap with other conditions like muscle strain, carpal tunnel syndrome, or even heart problems.
The complexity of nerve pathways makes it difficult to pinpoint the exact location and cause of nerve compression based on symptoms alone. The pain can vary in intensity, and some patients may not experience obvious arm symptoms, leading to confusion in initial assessments.
Western medicine typically relies on a combination of clinical evaluation and diagnostic imaging to confirm cervical radiculopathy.
During the clinical evaluation, a doctor will perform a physical examination, testing the strength, reflexes, and range of motion in the neck and arms. A Spurling’s test, where the head is turned and pressure is applied to the top of the head, may be used to reproduce symptoms and help localize the nerve root affected.
To confirm the diagnosis, imaging studies such as X-rays, CT scans, or MRIs are often used to visualize the spine and detect any structural issues, like herniated discs or bone spurs, that could be compressing the nerve roots. An electromyography (EMG) or nerve conduction study may also be performed to assess how well the nerves are functioning and to rule out other conditions affecting nerve function.
Conventional treatments for cervical radiculopathy, or treating a pinched nerve, generally focus on reducing pain, managing inflammation, and restoring normal function.
NSAID medications like ibuprofen or naproxen are usually recommended to reduce pain and inflammation around the pinched nerve. Corticosteroid injections may be used to reduce inflammation around the nerve root and offer temporary relief. Muscle relaxers may be prescribed to ease muscle spasms and reduce pressure on the pinched nerve.
Physical therapy exercises designed to improve neck mobility and strengthen supporting muscles, can potentially help relieve nerve compression. Using cervical traction devices to gently stretch the neck and reduce pressure on the affected nerve may be helpful in some cases.
In severe cases where non-surgical treatments don’t work, surgical options may be recommended to relieve pressure on the nerve by removing or repairing the affected disc or vertebra.
Acupuncture can be an effective modality for treating neck pain and stiffness due to cervical radiculopathy, without the unwanted side effects of taking pain medications and muscle relaxants.
Can Acupuncture Help Cervical Radiculopathy?
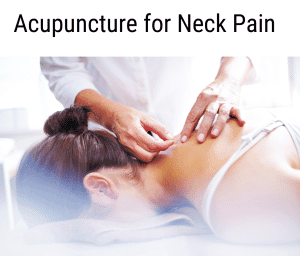
Acupuncture offers an alternative for patients suffering from neck pain who want to avoid surgery and the side effects of medication. Acupuncture treatment stimulates the body’s natural healing processes and alleviates pain by influencing the nervous system, reducing inflammation, and improving blood circulation to affected areas.
Acupuncture functions in multiple ways to help relieve nerve compression pain. It can help reduce swelling, or edema, that contribute to nerve compression. It also helps to relax muscle spasms. Acupuncture helps to increase blood flow to nerve roots.
Studies have shown that acupuncture can yield favorable outcomes, often comparable to conventional drug therapies. For instance, one randomized clinical trial found that acupuncture provided similar pain relief to drug therapy, making it a viable, safer alternative for pain management in cervical radiculopathy patients.
Additionally, some research has demonstrated the benefits of combining acupuncture with other conservative treatments, like cervical manipulations, to enhance therapeutic outcomes. In clinical trials, this combination has proven effective in reducing pain and improving mobility.
Acupuncture, used to complement other modalities, can be used as a valuable tool in the management of cervical radiculopathy, offering an effective, low-risk option to relieve pain and restore better mobility.
One case study of a patient with a C6/7 disc prolapse and radiculopathy showed that over a course of six acupuncture sessions administered within four weeks, significant improvements were observed in both pain and range of motion. Pain levels dropped from 8/10 to 2/10.
Acupuncture Near Me for Cervical Radiculopathy in West L.A.
At Art of Wellness Acupuncture and TCM in West Los Angeles, we have over 35 years of experience helping people find relief from all types of pain conditions related to nerve compression and neck pain, including herniated disks, spinal stenosis, cervical spondylosis, and cervical radiculopathy. Dr. Tan and Dr. Cai provide specialized care for each individual patient, including herbal remedies, therapeutic Chinese massage, and electroacupuncture to help relieve pain.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How To Treat Frozen Shoulder With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Can’t lift arm up? Front shoulder pain? Shoulders hurt when sleeping? Shoulder pain that doesn’t go away can be due to “frozen shoulder” and adhesive capsulitis. Acupuncture and TCM offer treatment for adhesive capsulitis frozen shoulder.
What Is Frozen Shoulder? Understanding Shoulder Pain and Adhesive Capsulitis
Frozen shoulder, medically known as adhesive capsulitis, is a painful condition that limits the range of motion in the shoulder. Over time, the shoulder joint can become stiff and difficult to move, leading to a significant loss of mobility.
Frozen shoulder typically progresses through three stages:
- Freezing – pain becomes gradually more intense, and range of motion decreases, sometimes until the arm is immobile – can last 6 weeks up to 9 months
- Frozen – pain may lessen, but the shoulder joint is still stiff and very difficult to move – can last 4-6 months
- Thawing – movement and strength is slowly regained – typically lasts anywhere between 6 months to 2 years
While frozen shoulder may be considered resolved when the pain has improved and basic functionality returns, many people continue to feel some stiffness and pain for many years.
What Causes Frozen Shoulder?
The shoulder is a ball-and-socket joint made up of three bones:
- The humerus (upper arm bone)
- The scapula (shoulder blade)
- The clavicle (collarbone)
The ball of the upper arm bone fits into a shallow socket in the shoulder blade, and this joint is surrounded by a thick capsule of connective tissue called the shoulder capsule. To help the shoulder move smoothly, synovial fluid lubricates the joint.
In cases of frozen shoulder, this capsule thickens and becomes stiff, with the development of adhesions or scar tissue, reducing the fluid in the joint. This usually leads to significant pain and often severely limited movement in the shoulder.
What Are the Risk Factors for Adhesive Capsulitis of the Shoulder?
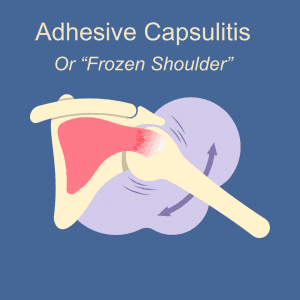
Frozen shoulder primarily affects adults, especially those between 40 and 60 years old, and it occurs more often in women than men. It is particularly common in women experiencing perimenopause and menopause, likely due to hormonal changes that can contribute to joint and connective tissue issues.
Certain medical conditions increase the likelihood of developing frozen shoulder. For example,
people with diabetes are at a higher risk for frozen shoulder, and they often experience more severe stiffness and longer recovery times.
Both hypothyroidism and hyperthyroidism are associated with an increased risk of frozen shoulder.
Immobilization of the shoulder following surgery or injury can also trigger the onset of frozen shoulder, especially if movement is restricted for long periods.
Many people wake up with a sore shoulder from sleeping in a way that restricts movement. Shoulder discomfort or front shoulder pain can happen due to sleeping positions that put pressure on the sensitive shoulder joint.
Frozen shoulder can also cause discomfort on one side, leading to reports of sore right shoulder or ache in left shoulder depending on which shoulder is affected.
Treatment for Frozen Shoulder/Adhesive Capsulitis
A doctor will typically diagnose frozen shoulder after an examination to determine passive range of motion and active range of motion in your shoulder. They may choose to order X-rays to rule out other problems.
In most cases, using hot and cold therapy with compresses and icing may be recommended, as well as pain medications/anti-inflammatories like Ibuprofen. If pain continues to be severe, a physician may offer steroid injections (corticosteroids).
Patients may be referred for physical therapy or massage to help with stretching and improving range of motion.
If pain and immobility persists past a year, surgery may be recommended. A “capsular release” procedure involves making small incisions in the tissues of the shoulder capsule. Manipulation and massage, while a person is anesthetized, can also help loosen up the tissues to allow for more mobility.
Acupuncture treatment can help relieve pain and improve mobility for frozen shoulder treatment without negative side effects that can come from the ongoing use of OTC pain medication and cortisone shots/corticosteroids, so it may be considered as an adjunct or alternative treatment for adhesive capsulitis.
Can Acupuncture Help Frozen Shoulder?
The TCM Chinese term for “frozen shoulder” translates into English as “shoulder at the age of 50 years.” Clearly, people in their middle age have been experiencing this pain and limitation in the shoulder joint for centuries. TCM has developed ways of helping to improve this condition.

According to TCM theory, frozen shoulder may fall under the category of “Bi Syndromes.” “Bi” refers to an obstruction of some sort, and Bi Syndromes typically cause pain and stiffness in a part of the body, due to a blockage of the flow of Qi (life force energy).
In TCM, “wind,” “damp,” and “cold” are considered pathogenic forces that can settle in an area of the body and cause blood and Qi to stagnate. This can cause stiffness, lack of movements, tenderness, swelling, and pain in that area. Most types of arthritis, for example, are considered Bi Syndromes.
Conventional medicine tends to treat each person presenting with a condition with the same types of treatments and waits to see if they work. In TCM, there is an understanding that different people can have the same symptoms, and yet have different underlying problems that are causing pain and other symptoms.
Different people may experience pain and stiffness due to different factors. One person may have a stiff, sore shoulder due to an invasion of cold or damp, while another person may show signs of heat or wind. In other words, the very specific presentation of symptoms can help the acupuncture practitioner to determine the underlying causes of the condition and treat them accordingly, with acupuncture and herbal remedies.
The stimulation of specific acupoints can help bring more blood flow to the shoulder joint, so that more nourishment can help reduce inflammation. Electroacupuncture, in particular, can help activate the release of endorphins that reduce pain.
A review of 13 controlled studies of the usage of acupuncture treatment for frozen shoulder determined that it is a good modality for both reducing pain and restoring proper shoulder function.
A randomized, single blind controlled trial looked at 35 patients with frozen shoulder symptoms. Some of the patients were assigned to a group that would engage in physical therapy sessions twice per week, practice exercises at home daily, and not use any pain medications, except in “emergency” situations.
The other group also engaged in physical therapy and exercise, plus they also were given acupuncture treatment twice per week, with functional movement exercises being performed during the acupuncture session.
After six weeks of treatment, patients who had only had PT showed an average 39.8% improvement, while the PT plus acupuncture patients showed an average 76.4% improvement.
One recorded case study detailed that, after 24 acupuncture treatments, a patient regained full range of motion in their shoulder and reported that pain was entirely gone.
Acupuncture for Frozen Shoulder Near Me in West L.A. and Santa Monica
At Art of Wellness Acupuncture in West Los Angeles, we have over 35 years of experience helping patients find relief from joint pain of all kinds. Dr. Tan is a specialist in treating orthopedic pain. We successfully treat joint pain conditions like frozen shoulder, osteoarthritis of the knee, tennis elbow, bone spurs, bursitis/hip pain, gout, and more. If you are suffering from a lack of mobility and pain in shoulder, please consider visiting our acupuncture office in Los Angeles for a consultation.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Splenomegaly (Enlarged Spleen) With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.
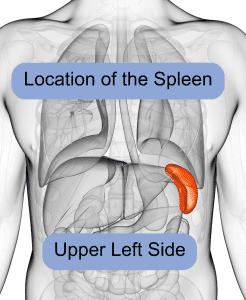
Left side abdominal pain that is tender to the touch? Feeling full after eating a small amount? Signs of anemia, bleeding easily? These may be enlarged spleen symptoms. Acupuncture and TCM can help with splenomegaly, along with spleen function and swollen spleen symptoms.
Splenomegaly is the medical term for an enlarged spleen. In conventional medical wisdom, the spleen is an organ that stores and filters blood, regulating the amounts of red blood cells, white blood cells, and platelets that are in circulation.
The spleen removes waste products and damaged blood cells from the bloodstream. It also produces antibodies (white blood cells) that fight germs and infection.
The spleen is located inside the left side of the ribcage, just above the stomach. Usually, the spleen is about the size of your fist—on average, about 12 centimeters long.
People often will not be aware of an enlarged spleen, but in some cases, there will be noticeable signs, such as pain in upper left abdomen and feeling “full.”
Spleen function is considered very important for overall health and happiness in TCM. Acupuncture treatment and Chinese herbs can provide an adjunct or alternative treatment for enlarged spleen.
Enlarged Spleen Symptoms
The most common swollen spleen symptoms include:
- Left upper quadrant pain, pain behind left ribs, left abdominal pain (upper abdomen), left side abdominal pain
- Pain that radiates to the left shoulder
- Feeling full even when you haven’t eaten
- Feeling full after eating only a small amount
- Anemia, low red blood cell count
- Bruise easily
- Bleeding easily
- Fatigue
- Catch colds frequently or suffer from other infections often
If you experience tenderness or serious left abdominal pain and feel dizzy, and/or have a rapid heartbeat, it is important to seek care immediately. These could be signs of ruptured spleen, which can lead to internal bleeding that could be life-threatening.
Enlarged Spleen Causes

There are several different conditions that can cause the spleen to become enlarged. What causes a big spleen, or should we say, bigger spleen?
Some of the health issues that can cause splenomegaly include:
- Liver cirrhosis, or other liver disease
- Viral hepatitis, Mononucleosis, or other viral infections
- Different types of hemolytic anemia
- Blood cancers, including: polycythemia vera and other myeloproliferative neoplasms, Leukemia, lymphoma, Hodgkin’s disease
- Blood clot near the spleen or liver
- Autoimmune disorders, including Lupus or Sarcoidosis, or rheumatoid arthritis (RA)
- Malaria, or other parasitic infections
- Bacterial infections
- Gaucher disease or Niemann-Pick disease
Medical Treatment for Enlarged Spleen
The treatment of splenomegaly in Western medicine primarily depends on addressing the underlying cause of the condition.
When an enlarged spleen is caused by infections like viral hepatitis or mononucleosis, the focus is typically on treating the infection itself. Antiviral medications may be prescribed to manage viral hepatitis, while mononucleosis, caused by the Epstein-Barr virus, usually requires supportive care. Rest, hydration, and over-the-counter pain relievers like acetaminophen or ibuprofen may be recommended to alleviate symptoms. In some cases, particularly when there’s a risk of the spleen rupturing, patients may be advised to avoid contact sports or strenuous activities.
For blood disorders that cause an enlarged spleen, treatment typically involves managing the specific blood condition. For example, in hemolytic anemia, where red blood cells are destroyed faster than they can be produced, treatments may include blood transfusions, corticosteroids to suppress the immune system, or medications like rituximab.
In conditions like polycythemia vera, where there’s an overproduction of red blood cells, treatment might involve phlebotomy (removing blood from the body) to reduce blood volume, or medications like hydroxyurea to suppress the bone marrow’s production of blood cells.
When liver disease such as cirrhosis is the cause of splenomegaly, the treatment approach focuses on managing the liver condition. Cirrhosis management may include lifestyle modifications such as reducing alcohol intake, using medications to control liver damage, and managing complications like portal hypertension. In severe cases, a liver transplant may be considered. Controlling the liver condition can help reduce spleen enlargement.
In cases where the spleen enlargement is due to cancers like leukemia or lymphoma, treatment usually involves chemotherapy, radiation therapy, or targeted drug therapies to address the cancer. The goal is to reduce the size of the spleen by shrinking the cancerous cells that are contributing to its enlargement. In certain situations where the spleen is significantly enlarged and causing symptoms, or if it’s not responding to other treatments, splenectomy (surgical removal of the spleen) might be recommended.
Autoimmune disorders like lupus or rheumatoid arthritis can also cause splenomegaly. Treatment for these conditions often involves immunosuppressive medications such as corticosteroids, methotrexate, or biologic agents that target specific parts of the immune system. By controlling the underlying autoimmune disorder, the symptoms associated with spleen enlargement can often be managed effectively.
When does an enlarged spleen need to be removed?
In some cases, if the spleen is severely enlarged or if it’s causing significant symptoms or complications (such as a high risk of rupture), a splenectomy may be considered. This surgical procedure involves removing the spleen entirely. While splenectomy can relieve symptoms and prevent complications, it also has long-term implications, as the spleen plays an important role in the immune system. Patients who undergo splenectomy may require vaccinations and prophylactic antibiotics to reduce the risk of infections.
Unless the spleen is ruptured, in most cases, a splenectomy is not necessary. Trying a holistic approach with TCM and acupuncture may be able to help relieve symptoms and improve spleen function.
Can Acupuncture Help Enlarged Spleen?
Traditional Chinese Medicine takes a different few of key organs and organ systems than we are used to in modern medicine.
In TCM, the spleen is considered vital to the digestion of food, working in harmony with the stomach. The spleen is also partially responsible for the transport of blood and water throughout the body, delivering nutrition to the muscles.
The spleen is also vital to the proper excretion of waste. When there is a buildup of excessive fluids or “dampness” in the body, it is often due to a deficiency of the spleen.
Fatigue and a sense of fullness after eating are considered signs of spleen deficiency, which can affect whether or not other organs are getting the nutrition they need.
Problems with the spleen may also be related to the liver and/or the stomach, so the acupuncture practitioner will carefully look at all of a patient’s presenting symptoms to determine the appropriate diagnostic pattern and course of treatment.
In TCM, organs are related to certain emotions, and the spleen is connected to anxiety. Thus, worrying, overthinking, and other manifestations of anxiety are believed to negatively impact the spleen.
TCM treatment to help strengthen spleen function may focus on clearing stagnation and dampness, and improving circulation of blood and Qi. Your acupuncture provider can develop a course of treatment with acupuncture and herbs to address the underlying causes of an enlarged spleen, while also helping to relieve any symptoms of splenomegaly.
Acupuncture for Enlarged Spleen Near Me in West Los Angeles
If you are experiencing enlarged spleen symptoms, acupuncture and TCM offer holistic approaches that can support spleen function and address the root causes of various health issues. At Art of Wellness, our experienced practitioners can help tailor a treatment plan to your unique needs. Contact us today to learn more about how TCM can benefit your health and well-being.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Shin Splints With Acupuncture and TCM
By Qineng Tan, L.Ac., Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Shin pain, especially during or after exercise? Tenderness and swelling around the shin bone? These may be signs of shin splints, or a shin strain. Acupuncture and TCM can provide shin splints treatment.
Shin splints, also known as medial tibial stress syndrome (MTSS), are a common condition characterized by pain along the inner edge of the shinbone (tibia). This discomfort typically occurs during or after exercise, particularly activities that involve running, jumping, or repetitive stress on the legs.
Shin splints are often attributed to overuse or excessive strain on the muscles, tendons, and bone tissue of the lower leg. This condition involves stress to the soft tissues that causes them to become swollen and hard.
Shin splints pain can be similar to compartment syndrome symptoms, but these are two distinctly different conditions. Compartment syndrome occurs when swelling in the calf area causes a blockage of blood flow to the lower leg. This usually happens due to an injury (acute compartment syndrome) or extreme exertion (chronic exertional compartment syndrome) and causes a severe lack of oxygen in the area. Compartment syndrome usually causes severe pain, sometimes with a tingling or burning sensation, and requires medical attention.
What Causes Shin Splints?

Several factors can contribute to the development of shin splints. One of the primary causes is repetitive stress or overloading of the leg muscles, particularly those responsible for dorsiflexion (lifting the foot upwards) and supporting the arch of the foot. This can occur due to sudden increases in activity level, such as starting a new exercise regimen or intensifying training too quickly, without allowing adequate time for the body to adapt and recover.
Some people may be more prone to developing shin splints because of issues like flat feet, overpronation (excessive inward rolling of the foot), and muscle imbalances in the lower limbs can place additional strain on the shinbone and surrounding soft tissues, increasing the risk of injury.
Wearing footwear with insufficient cushioning or support, running on hard or uneven surfaces, and running downhill or on inclined terrain can all exacerbate the stress on the lower legs and contribute to the development of shin splints. Additionally, factors such as tight calf muscles, weak shin muscles, and not warming up or stretching before exercise can further increase susceptibility to this condition.
Taking care to stretch and warm up before working out, wearing shoes with enough support, and gradually increasing intensity of training can help prevent shin splints.
However, runners and athletes who play basketball or soccer are likely to experience shin splints when they are training and competing.
Shin splints treatment generally requires time and patience. Acupuncture can provide pain relief and help speed recovery from shin splints.
Top 10 Signs and Symptoms of Shin Splints
These signs and symptoms may vary in severity and duration depending on the individual and the underlying causes of shin splints.
- Pain along the inner edge of the shinbone (tibia), typically felt during or after physical activity.
- Tenderness and soreness along the shinbone, especially upon palpation or pressure.
- Swelling or inflammation of the lower leg, often localized to the area of pain.
- Dull, aching pain that may worsen with activity and subside with rest.
- Discomfort that initially occurs at the beginning of exercise but may progress to persist throughout the activity.
- Pain that gradually increases in intensity or becomes more widespread over time.
- Pain that may be accompanied by a feeling of tightness or stiffness in the muscles of the lower leg.
- Pain that persists even after cessation of activity and may interfere with daily activities.
- Possible development of small lumps or bumps along the inner border of the shinbone due to inflammation or irritation of the surrounding tissues.
- Pain that improves with rest but recurs upon resuming physical activity, especially activities that involve impact or weight-bearing on the legs.
Shin Splints Treatment

Conventional treatment of shin splints usually involves rest and over the counter pain relief. Typically, a doctor will recommend that a person with shin splints limits their exercise to low-impact activities. Icing the area several times per day is advised.
Acupuncture treatment for medial tibial stress syndrome can help relieve shin pain quickly.
One case study showed that a patient who had been suffering from shin splints for six weeks got pain relief after one session of acupuncture treatment, and at a four week follow, was still pain-free.
Can Acupuncture Help Shin Splints?
Acupuncture treatment helps with the healing of soft tissue injuries by increasing circulation to the area, relieving inflammation, and aiding in the release of endorphins for pain relief. It does this by activating Qi to move blood and energy more efficiently through the body.
One study of three groups of athletes with shin splints looked at patients who received conventional sports medicine, patients who received acupuncture, and patients who received both. The groups who received acupuncture treatment reported significantly lower pain levels and used less NSAIDs than those who did not receive acupuncture.
Acupuncture Near Me for Shin Splints in West Los Angeles
Acupuncture is an effective modality for treating many kinds of repetitive stress injuries and nerve pain conditions, including sprained ankles, Baker’s cyst, tendinitis, and carpal tunnel syndrome. Dr. Tan has over 35 years of experience helping patients find pain relief and improved mobility through treating all kinds of orthopedic and musculoskeletal conditions. While each case is unique, it is possible to get pain relief quickly with TCM treatment, including acupuncture, electro-acupuncture, therapeutic massage like Tui Na, topical herbal patches, and herbal ointments. If you are in pain and need to heal quickly to get back to your regular activities, acupuncture can help.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.
How to Treat Costochondritis With Acupuncture and TCM
By Qineng Tan, L.Ac. Ph.D. and Xiaomei Cai, L.Ac., Ph.D.

Chest pain? Rib pain, sternum pain? These can be costochondritis symptoms, caused by inflammation of the cartilage that connects the ribs to the sternum. Acupuncture and TCM can provide costochondritis treatment to relieve pain and inflammation.
Costochondritis is a pain condition caused by inflammation of cartilage in the rib cage. It can be scary, because the pain can feel like a heart attack or a symptom of heart disease.
It is quite common for people who are experiencing costochondritis pain to visit the emergency room complaining of chest pain. Almost 10% of ER visits are related to chest pain symptoms, and a significant number of those turn out to be related to something other than heart problems.
Sometimes called “chest wall pain syndrome,” or costosternal syndrome, costochondritis is considered a syndrome because it presents as a set of symptoms that often does not have a clear cause.
Possible causes of costochondritis include:
- Trauma or injury to the chest or ribs
- Persistent cough
- Repeated bouts of vomiting
- Chest or lung infection
- Allergies that affect the lungs
- Fibromyalgia
- Tietze syndrome
Suddenly doing some kind of heavy labor or intense workout that you’re not used to, that causes you to be winded, could cause inflammation of the chest. Playing contact sports in which you may be tackled or collide with another player or get hit hard with a ball in the chest could also cause costochondritis.
Tietze syndrome is a rare condition in which the cartilage connecting the ribs to the breastbone becomes inflamed and swollen. With Tietze syndrome, the pain and swelling in the chest is usually higher up, around the second and third ribs.
Costochondritis pain usually is felt more on the left side of the chest, radiating outward, and there isn’t any swelling involved.
Rib pain may be exacerbated when lying down, which can make it difficult to sleep comfortably.
Costochondritis is most commonly experienced by people in middle age (40-50s), but it can occur in children and adolescents, as well as adults.
In most cases, costochondritis is temporary. However, costochondritis pain can limit your activities and be debilitating for weeks, or even months. One study showed that up to a third of adults reported pain persisting beyond a year.
Acupuncture has been shown to help alleviate costochondritis pain, often in a matter of weeks.
Costochondritis Symptoms
Costochondritis pain can range anywhere from a slight tenderness to severe chest pain. In mild cases, the pain may go away in a matter of days, but in other cases, the pain can become serious.
Symptoms of costochondritis include:
- Sharp chest pain
- Chest pressure, chest ache, tenderness in breastbone
- Pain on the left side of chest, to the left of the breastbone
- Rib pain in more than one rib
- Pain radiating to shoulders and/or arms
- Chest pain when coughing, sneezing, or taking a deep breath
- Pain in chest when reaching up or twisting the torso
- Rib pain when lying down
- Pain when hugging someone
- Pain when putting on a seatbelt
Medical Diagnosis and Costochondritis Treatment

Other than the doctor palpating the area around your breastbone and ribs, there is no specific test to determine if you have costochondritis.
Chest pain can be an indicator of a variety of health conditions, including heart problems or lung problems, so it is always important to get it checked out with a healthcare professional. They will rule out other problems by ordering an EKG or chest X-ray in order to get to a diagnosis of costochondritis.
Treatment will consist of recommendations for ways to alleviate pain. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen (Advil, Motrin IB) or naproxen (Aleve) can help reduce inflammation and pain.
In cases of more severe or persistent pain, a doctor may prescribe stronger pain medications such as prescription-strength Motrin or muscle relaxers.
Applying heat or cold packs to the affected area can help reduce inflammation and alleviate pain. Some individuals find relief by alternating between heat and cold therapy.
In cases where pain is severe and not responding to other treatments, corticosteroid injections directly into the affected area may provide temporary relief by reducing inflammation.
Acupuncture treatment is a great way to relieve pain and reduce inflammation, without the side effects that can result from using pain medications or steroids for several weeks or months.
Can Acupuncture Help Costochondritis?
Acupuncture has been used for many centuries to treat pain and inflammation. Now, research is able to show how and why this modality is able to regulate inflammatory responses. Acupuncture affects the nerve signaling that produces hormones like dopamine and can reduce the production of cytokine storms. This is why acupuncture can help relieve inflammation and chest pain of costochondritis.
In TCM theory, pain and inflammation are usually considered to occur because of stagnation, or stasis, of blood and/or Qi (life force energy). The same symptoms can occur in different individuals because of different imbalances in the organs systems that are causing the blockages and different pathogenic factors, such as excess heat, dampness, etc.
Costochondritis inflammation can occur due to dampness and stagnation of Qi in the liver, spleen, and/or kidney systems. Depending on each patient’s specific situation, your acupuncturist will choose acupoints to open channels, clear dampness, heat, and phlegm. This allows for Qi and blood to flow smoothly again, cooling down the inflammation and relieving pain.
One case study of six women who were treated for costochondritis pain with acupuncture found that all patients reported improvement and were able to discontinue taking OTC pain medications.
One pediatric study looked at young students suffering from costochondritis; they were missing school, limiting their sports, dance, and work, and having trouble sleeping. After 4-6 weeks of acupuncture treatment, these patients reported a significant reduction in pain, and were able to resume their usual activities.
Not only is acupuncture treatment effective for relief of costochondritis pain; it can work quickly. In many cases, patients feel better after one or two treatments.
Acupuncture Near Me for Costochondritis in Los Angeles Area
Dr. Tan and Dr. Cai of Art of Wellness Acupuncture in West L.A. have been helping treat pain conditions for over 35 years. Our office is a home away from home where patients are able to relax and find relief from pain and inflammation. If you or someone you love is experiencing chest pain due to costochondritis, please do not hesitate to come in for a consultation.
*This article is for education from the perspective of Traditional Chinese Medicine only. The education provided by this article is not approved by FDA to diagnose, prevent, treat and cure human diseases. It should not stop you from consulting with your physician for your medical conditions. Traditional Chinese Medicine is based on Qi, which is an invisible force that usually cannot be observed by modern science. Because science focuses on testing ideas about the natural world with evidence obtained through observation, these aspects of acupuncture can’t be studied by science. Therefore acupuncture and Chinese herbs are often not supported by double-blind, randomized trials, and they are considered alternative medicine therapies in the United States.